Optimal Frequency of Retinopathy Screening in Adolescents With Type 1 Diabetes: Markov Modeling Approach Based on 30 Years of Data
- PMID: 35975939
- PMCID: PMC9643143
- DOI: 10.2337/dc22-0071
Optimal Frequency of Retinopathy Screening in Adolescents With Type 1 Diabetes: Markov Modeling Approach Based on 30 Years of Data
Abstract
Objective: Current guidelines recommend biennial diabetic retinopathy (DR) screening commencing at the age of 11 years and after 2-5 years' duration of type 1 diabetes. Growing evidence suggests less frequent screening may be feasible.
Research design and methods: Prospective data were collected from 2,063 youth with type 1 diabetes who were screened two or more times between 1990 and 2019. Baseline (mean ± SD) age was 13.3 ± 1.8 years, HbA1c was 8.6 ± 1.3% (70.1 ± 14.7 mmol/mol), diabetes duration was 5.6 ± 2.8 years, and follow-up time was 4.8 ± 2.8 years. DR was manually graded from 7-field retinal photographs using the Early Treatment Diabetic Retinopathy Study (ETDRS) scale. Markov chain was used to calculate probabilities of DR change over time and hazard ratio (HR) of DR stage transition.
Results: The incidence of moderate nonproliferative DR (MNPDR) or worse was 8.6 per 1,000 patient-years. Probabilities of transition to this state after a 3-year interval were from no DR, 1.3%; from minimal DR, 5.1%; and from mild DR, 22.2%, respectively. HRs (95% CIs) for transition per 1% current HbA1c increase were 1.23 (1.16-1.31) from no DR to minimal NPDR, 1.12 (1.03-1.23) from minimal to mild NPDR, and 1.28 (1.13-1.46) from mild to MNPDR or worse. HbA1c alone explained 27% of the transitions between no retinopathy and MNPDR or worse. The addition of diabetes duration into the model increased this value to 31% (P = 0.03). Risk was also increased by female sex and higher attained age.
Conclusions: These results support less frequent DR screening in youth with type 1 diabetes without DR and short duration. Although DR progression to advanced stages is generally slow, higher HbA1c greatly accelerates it.
© 2022 by the American Diabetes Association.
Figures
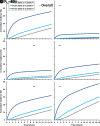
References
-
- American Diabetes Association Professional Practice Committee 14 . Children and adolescents: Standards of Medical Care in Diabetes—2022. Diabetes Care 2022;45(Suppl. 1):S208–S231 - PubMed
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical

