Trends in COVID-19 hospital outcomes in England before and after vaccine introduction, a cohort study
- PMID: 35977938
- PMCID: PMC9382625
- DOI: 10.1038/s41467-022-32458-y
Trends in COVID-19 hospital outcomes in England before and after vaccine introduction, a cohort study
Abstract
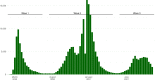
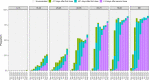
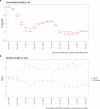
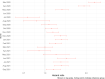
Widespread vaccination campaigns have changed the landscape for COVID-19, vastly altering symptoms and reducing morbidity and mortality. We estimate trends in mortality by month of admission and vaccination status among those hospitalised with COVID-19 in England between March 2020 to September 2021, controlling for demographic factors and hospital load. Among 259,727 hospitalised COVID-19 cases, 51,948 (20.0%) experienced mortality in hospital. Hospitalised fatality risk ranged from 40.3% (95% confidence interval 39.4-41.3%) in March 2020 to 8.1% (7.2-9.0%) in June 2021. Older individuals and those with multiple co-morbidities were more likely to die or else experienced longer stays prior to discharge. Compared to unvaccinated people, the hazard of hospitalised mortality was 0.71 (0.67-0.77) with a first vaccine dose, and 0.56 (0.52-0.61) with a second vaccine dose. Compared to hospital load at 0-20% of the busiest week, the hazard of hospitalised mortality during periods of peak load (90-100%), was 1.23 (1.12-1.34). The prognosis for people hospitalised with COVID-19 in England has varied substantially throughout the pandemic and according to case-mix, vaccination, and hospital load. Our estimates provide an indication for demands on hospital resources, and the relationship between hospital burden and outcomes.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


References
-
- Kirwan, P. D. et al. Trends in risks of severe events and lengths of stay for COVID-19 hospitalisations in England over the pre-vaccination era: results from the Public Health England SARI-Watch surveillance scheme. arXiv [stat.AP]. http://arxiv.org/abs/2103.04867 (2021).
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

