External validation of a surgical mortality risk prediction model for inpatient noncardiac surgery in an Australian private health insurance dataset
- PMID: 35979735
- PMCID: PMC9804688
- DOI: 10.1111/ans.17946
External validation of a surgical mortality risk prediction model for inpatient noncardiac surgery in an Australian private health insurance dataset
Abstract
Background: We previously conducted a systematic review to identify surgical mortality risk prediction tools suitable for adapting in the Australian context and identified the Surgical Outcome Risk Tool (SORT) as an ideal model. The primary aim was to investigate the external validity of SORT for predicting in-hospital mortality in a large Australian private health insurance dataset.
Methods: A cohort study using a prospectively collected Australian private health insurance dataset containing over 2 million deidentified records. External validation was conducted by applying the predictive equation for SORT to the complete case analysis dataset. Model re-estimation (recalibration) was performed by logistic regression.
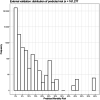
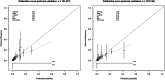
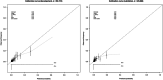
Results: The complete case analysis dataset contained 161 277 records. In-hospital mortality was 0.2% (308/161277). The mean estimated risk given by SORT was 0.2% and the median (IQR) was 0.01% (0.003%-0.08%). Discrimination was high (c-statistic 0.96) and calibration was accurate over the range 0%-10%, beyond which mortality was over-predicted but confidence intervals included or closely approached the perfect prediction line. Re-estimation of the equation did not improve over-prediction. Model diagnostics suggested the presence of outliers or highly influential values.
Conclusion: The low perioperative mortality rate suggests the dataset was not representative of the overall Australian surgical population, primarily due to selection bias and classification bias. Our results suggest SORT may significantly under-predict 30-day mortality in this dataset. Given potential differences in perioperative mortality, private health insurance status and hospital setting should be considered as covariables when a locally validated national surgical mortality risk prediction model is developed.
Keywords: anaesthesia; mortality; outcome; perioperative; risk; risk score; surgery.
© 2022 The Authors. ANZ Journal of Surgery published by John Wiley & Sons Australia, Ltd on behalf of Royal Australasian College of Surgeons.
Conflict of interest statement
None declared.
Figures
Similar articles
-
Systematic review of perioperative mortality risk prediction models for adults undergoing inpatient non-cardiac surgery.ANZ J Surg. 2021 May;91(5):860-870. doi: 10.1111/ans.16255. Epub 2020 Sep 15. ANZ J Surg. 2021. PMID: 32935458
-
Developing and validating subjective and objective risk-assessment measures for predicting mortality after major surgery: An international prospective cohort study.PLoS Med. 2020 Oct 15;17(10):e1003253. doi: 10.1371/journal.pmed.1003253. eCollection 2020 Oct. PLoS Med. 2020. PMID: 33057333 Free PMC article.
-
Recalibration and External Validation of the Risk Analysis Index: A Surgical Frailty Assessment Tool.Ann Surg. 2020 Dec;272(6):996-1005. doi: 10.1097/SLA.0000000000003276. Ann Surg. 2020. PMID: 30907757 Free PMC article.
-
Development of a Pediatric Risk Assessment Score to Predict Perioperative Mortality in Children Undergoing Noncardiac Surgery.Anesth Analg. 2017 May;124(5):1514-1519. doi: 10.1213/ANE.0000000000001541. Anesth Analg. 2017. PMID: 27575562
-
Performance of prediction models for nephropathy in people with type 2 diabetes: systematic review and external validation study.BMJ. 2021 Sep 28;374:n2134. doi: 10.1136/bmj.n2134. BMJ. 2021. PMID: 34583929 Free PMC article.
Cited by
-
An interrater reliability analysis of preoperative mortality risk calculators used for elective high-risk noncardiac surgical patients shows poor to moderate reliability.BMC Anesthesiol. 2024 Oct 30;24(1):392. doi: 10.1186/s12871-024-02771-8. BMC Anesthesiol. 2024. PMID: 39478449 Free PMC article.
-
[Preoperative risk prediction models for noncardiac surgery patients : Interpret and use risk scores correctly].Anaesthesiologie. 2024 Dec;73(12):861-870. doi: 10.1007/s00101-024-01481-7. Epub 2024 Nov 22. Anaesthesiologie. 2024. PMID: 39576320 German.
References
-
- Peden CJ, Stephens T, Martin G et al. A national quality improvement programme to improve survival after emergency abdominal surgery: the EPOCH stepped‐wedge cluster RCT. Health Services Deliv. Res. 2019; 7: 1–96. - PubMed
-
- Story DA, Shelton A, Jones D, Heland M, Belomo R. Austin health Post‐operative surveillance team I. audit of co‐management and critical care outreach for high risk postoperative patients (the POST audit). Anaesth. Intensive Care 2013; 41: 793–8. - PubMed
-
- Swart M, Carlisle JB, Goddard J. Using predicted 30 day mortality to plan postoperative colorectal surgery care: a cohort study. Br. J. Anaesth. 2017; 118: 100–4. - PubMed
-
- Campbell D, Boyle L, Soakell‐Ho M et al. National risk prediction model for perioperative mortality in non‐cardiac surgery. Br. J. Surg. 2019; 106: 1549–57. - PubMed
Publication types
MeSH terms
Grants and funding
- Australian and New Zealand College of Anaesthetists, Project Grant and PhD Scholarship
- Australian Government, Research Training Program (RTP) Scholarship
- Australian Society of Anaesthetists, Jackson Rees Research Scholarship
- Faculty of Medicine, Nursing and Health Sciences, Monash University, Graduate Excellence Scholarship
- National Health and Medical Research Council, Practitioner Fellowship
LinkOut - more resources
Full Text Sources
Medical

