Adult acetonemic vomiting complicated with low body weight in a subject with Mycobacterium avium complex pulmonary disease: a case report
- PMID: 35996312
- PMCID: PMC9421232
- DOI: 10.1177/03000605221118506
Adult acetonemic vomiting complicated with low body weight in a subject with Mycobacterium avium complex pulmonary disease: a case report
Abstract
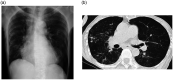
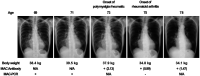
Pulmonary diseases often cause significant health issues and nutritional disorders. Weight loss and malnutrition are related to the severity of obstructive disorders. Therefore, patients with such conditions often experience low nutritional energy. Acetonemic vomiting is caused by acetonemic syndrome. Previously, it was believe that acetonemic vomiting was observed only in childhood. However, it was recently suggested that acetonemic vomiting can also occur in adults. It is also considered that acetonemic vomiting can occur in subjects with low body weight because stored carbohydrate levels are reduced and fats are mainly used for energy. Consequently, large amounts of acetone are produced, ultimately resulting in nausea and vomiting. In this study, we report a case of adult acetonemic vomiting complicated by low body weight in a subject with Mycobacterium avium complex pulmonary disease.
Keywords: Acetonemic vomiting; Mycobacterium avium complex pulmonary disease; acetone; adult; low body weight; mild hypoglycemia; obstructive disorder.
Conflict of interest statement
Figures

Similar articles
-
Comparative genome analysis of Mycobacterium avium revealed genetic diversity in strains that cause pulmonary and disseminated disease.PLoS One. 2013 Aug 21;8(8):e71831. doi: 10.1371/journal.pone.0071831. eCollection 2013. PLoS One. 2013. PMID: 23990995 Free PMC article.
-
Ribosomal internal transcribed spacer sequences are identical among Mycobacterium avium-intracellulare complex isolates from AIDS patients, but vary among isolates from elderly pulmonary disease patients.Microbiology (Reading). 1995 Oct;141 ( Pt 10):2739-47. doi: 10.1099/13500872-141-10-2739. Microbiology (Reading). 1995. PMID: 7582034
-
Mycobacterium avium complex lung disease and panhypopituitarism.Mayo Clin Proc. 2005 Jul;80(7):961-2. doi: 10.4065/80.7.961-a. Mayo Clin Proc. 2005. PMID: 16007905 No abstract available.
-
[A case of pulmonary mycobacterium intracellulare infection complicated with pneumothorax and pleurisy].Kekkaku. 2005 Aug;80(8):571-5. Kekkaku. 2005. PMID: 16218447 Review. Japanese.
-
Case report: a rare case of chylous ascites from Mycobacterium avium intracellulare in a patient with AIDS: review of the literature.Dig Dis Sci. 1996 Dec;41(12):2499-501. doi: 10.1007/BF02100149. Dig Dis Sci. 1996. PMID: 9011464 Review.
Cited by
-
Acetonemic vomiting: a potential complication of treatment with glucagon-like peptide-1 receptor agonists especially in lean type 2 diabetes patients.Diabetol Int. 2024 Oct 21;16(1):162-168. doi: 10.1007/s13340-024-00758-x. eCollection 2025 Jan. Diabetol Int. 2024. PMID: 39877456
References
-
- Onwubalili JK. Malnutrition among tuberculosis patients in Harrow, England. Eur J Clin Nutr 1988; 42: 363–366. PMID: 3396528. - PubMed
-
- Morimoto K, Yoshiyama T, Kurashima A, et al.. Nutritional indicators are correlated with the radiological severity score in patients with Mycobacterium avium complex pulmonary disease: a cross-sectional study. Intern Med 2014; 53: 397–401. doi: 10.2169/internalmedicine.53.1277. - PubMed
-
- Fitzpatrick E, Bourke B, Drumm B, et al.. The incidence of cyclic vomiting syndrome in children: population-based study. Am J Gastroenterol 2008; 103: 991–995; quiz 996. doi: 10.1111/j.1572-0241.2007.01668.x. - PubMed
-
- Lin YP, Ni YH, Weng WC, et al.. Cyclic vomiting syndrome and migraine in children. J Formos Med Assoc 2011; 110: 382–387. doi: 10.1016/S0929-6646(11)60056-9. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

