Cost reduction associated with transradial access in percutaneous coronary intervention: A report from a Japanese nationwide registry
- PMID: 35996698
- PMCID: PMC9391571
- DOI: 10.1016/j.lanwpc.2022.100555
Cost reduction associated with transradial access in percutaneous coronary intervention: A report from a Japanese nationwide registry
Abstract
Background: Percutaneous coronary intervention (PCI) is increasingly performed via transradial access (TRA). This study aimed to investigate the clinical and economic benefits of TRA compared with transfemoral access (TFA) under universal healthcare coverage system in Japan.
Methods: A total of 36,153 patients (acute coronary syndrome [ACS], 15,266; stable ischemic heart disease [SIHD], 20,052) across 714 institutions in the Japanese nationwide PCI registry (J-PCI) in 2015 were analyzed (mean age 69.9 ± 11.1 years and 23.6% female). Cost was defined as the total amount of healthcare resources used to care for the patient during hospitalization. Propensity score matching analysis was conducted to balance the baseline characteristics of patients undergoing TRA and TFA.
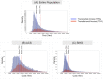
Findings: The median total cost of PCI was JPY 1,341,176 (interquartile range, 959,052), with higher expenses for ACS (JPY 1,772,116 [1,117,107]) compared with SIHD (JPY 1,119,153 [540,440]) patients. Most patients underwent PCI via TRA (73.8%), and after propensity score matching, TRA was associated with a reduced risk of in-hospital death and bleeding (0.88% vs. 1.91% [P < 0.0001] and 2.18% vs. 4.53% [P < 0.0001] in ACS, and 0.10% vs. 0.28% [P = 0.070] and 0.53% vs. 1.72% [P < 0.0001] in SIHD, respectively), which led to lower costs in both ACS (JPY 1,699,279 [1,164,554] for TRA vs. JPY 1,931,255 [1,070,222] for TFA; P < 0.0001), and SIHD (JPY 1,102,352 [505,904] for TRA vs. JPY 1,311,525 [706,450] for TFA; P < 0.0001) patients.
Interpretation: In this direct cost analysis of a nationwide registry, the use of TRA was associated with cost saving for both ACS and SIHD patients.
Funding: This study was funded by the Japan Society for the Promotion of Science (grant nos. 20H03915, 16H05215, 16KK0186, 20K22883, and 21K08064), Japan Agency for Medical Research and Development [AMED] (grant number 16lk1010004h0002), and the National Clinical Database. The J-PCI registry is led and supported by the Japanese Association of Cardiovascular Intervention and Therapeutics.
Keywords: Cost; Nationwide registry; Percutaneous coronary intervention; Transradial access.
© 2022 The Author(s).
Conflict of interest statement
SK received investigator-initiated grant funding from Novartis, Daiichi-Sankyo, and Bristol-Myers Squibb and personal fees from Bristol-Myers Squibb and Pfizer. HK, SN and HM are affiliated with the Department of Healthcare Quality Assessment. The department is a social collaboration department supported by National Clinical Database, Johnson & Johnson KK, and Nipro corporation. HK has received consultation fee from Mitsubishi Tanabe Pharma, and speaker fee from Johnson & Johnson KK. H.I. receives lecture fees from Astellas, AstraZeneca, Bayer, Bristol-Myers Squibb, Daiichi Sankyo, Kowa, Mochida, Novartis, Otsuka, Pfizer, and Tanabe-Mitsubishi. All other authors have no relationships relevant to the contents of this paper.
Figures

Similar articles
-
Impact of Access Site on Periprocedural Bleeding and Cerebral and Coronary Events in High-Bleeding-Risk Percutaneous Coronary Intervention: Findings from the RIVA-PCI Trial.Cardiol Ther. 2024 Mar;13(1):89-101. doi: 10.1007/s40119-023-00343-4. Epub 2023 Dec 6. Cardiol Ther. 2024. PMID: 38055177 Free PMC article.
-
The Rise of Transradial Artery Access for Percutaneous Coronary Intervention in Patients with Acute Coronary Syndromes in Australia.J Interv Cardiol. 2020 Nov 27;2020:4397697. doi: 10.1155/2020/4397697. eCollection 2020. J Interv Cardiol. 2020. PMID: 33312077 Free PMC article.
-
Outcomes of Transradial Approach to Percutaneous Coronary Intervention in End-Stage Renal Disease Patients on Dialysis.Cardiovasc Revasc Med. 2020 Sep;21(9):1131-1135. doi: 10.1016/j.carrev.2020.01.017. Epub 2020 Jan 25. Cardiovasc Revasc Med. 2020. PMID: 32107158
-
Left main percutaneous coronary intervention-Radial versus femoral access: A systematic analysis.Catheter Cardiovasc Interv. 2020 Jun 1;95(7):E201-E213. doi: 10.1002/ccd.28451. Epub 2019 Aug 20. Catheter Cardiovasc Interv. 2020. PMID: 31430040
-
Transradial Versus Transfemoral Access for Percutaneous Coronary Intervention of Unprotected Left Main Coronary Artery Stenosis: A Systematic Review and Meta-Analysis.Cardiovasc Revasc Med. 2019 Sep;20(9):790-798. doi: 10.1016/j.carrev.2018.10.025. Epub 2018 Nov 3. Cardiovasc Revasc Med. 2019. PMID: 30442537
Cited by
-
The importance of ankel-brachial index in prediction vascular complications in transradial access procedures.Sci Prog. 2024 Apr-Jun;107(2):368504241261853. doi: 10.1177/00368504241261853. Sci Prog. 2024. PMID: 38872465 Free PMC article.
-
Chinese expert consensus on transradial access in percutaneous peripheral interventions.J Interv Med. 2023 Nov 10;6(4):145-152. doi: 10.1016/j.jimed.2023.10.005. eCollection 2023 Nov. J Interv Med. 2023. PMID: 38312127 Free PMC article.
-
Comparison of distal and conventional transradial access on procedure duration and radiation exposure in carotid artery stenting.BMC Cardiovasc Disord. 2025 Apr 25;25(1):321. doi: 10.1186/s12872-025-04774-w. BMC Cardiovasc Disord. 2025. PMID: 40275170 Free PMC article.
-
Association of Malnutrition and High Bleeding Risk with Long-Term Prognosis in Patients with Acute Coronary Syndrome following Percutaneous Coronary Intervention.Medicines (Basel). 2023 Nov 30;10(12):62. doi: 10.3390/medicines10120062. Medicines (Basel). 2023. PMID: 38132889 Free PMC article.
-
Trends, costs, and complications associated with after-hours surgery and unscheduled hospitalization in spinal surgery.Bone Jt Open. 2024 Aug 9;5(8):662-670. doi: 10.1302/2633-1462.58.BJO-2024-0026.R1. Bone Jt Open. 2024. PMID: 39117344 Free PMC article.
References
-
- Masoudi FA, Ponirakis A, de Lemos JA, et al. Trends in U.S. cardiovascular care: 2016 report from 4 ACC National Cardiovascular Data Registries. J Am Coll Cardiol. 2017;69:1427–1450. - PubMed
-
- Inohara T, Kohsaka S, Spertus JA, et al. Comparative trends in percutaneous coronary intervention in Japan and the United States, 2013 to 2017. J Am Coll Cardiol. 2020;76:1328–1340. - PubMed
-
- Caputo RP, Tremmel JA, Rao S, et al. Transradial arterial access for coronary and peripheral procedures: executive summary by the transradial committee of the SCAI. Catheter Cardiovasc Interv. 2011;78:823–839. - PubMed
-
- Ferrante G, Rao SV, Jüni P, et al. Radial versus femoral access for coronary interventions across the entire spectrum of patients with coronary artery disease: a meta-analysis of randomized trials. JACC Cardiovasc Interv. 2016;9:1419–1434. - PubMed
-
- Khan AA, Panchal HB, Zaidi SIM, et al. Safety and efficacy of radial versus femoral access for rotational atherectomy: a systematic review and meta-analysis. Cardiovasc Revasc Med. 2019;20:241–247. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

