Health status of children and young persons with congenital adrenal hyperplasia in the UK (CAH-UK): a cross-sectional multi-centre study
- PMID: 36001026
- PMCID: PMC9513639
- DOI: 10.1530/EJE-21-1109
Health status of children and young persons with congenital adrenal hyperplasia in the UK (CAH-UK): a cross-sectional multi-centre study
Abstract
Objective: There is limited knowledge on the onset of comorbidities in congenital adrenal hyperplasia (CAH) during childhood. We aimed to establish the health status of children with CAH in the UK.
Design and methods: This cross-sectional multicentre study involved 14 tertiary endocrine UK units, recruiting 101 patients aged 8-18 years with classic 21-hydroxylase deficiency and 83 controls. We analysed demographic, clinical and metabolic data, as well as psychological questionnaires (Strengths and Difficulties (SDQ), Paediatric Quality of Life (PedsQL)).
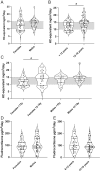
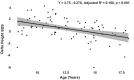
Results: Patient height SDS in relation to mid-parental height decreased with age, indicating the discrepancy between height achieved and genetic potential height. Bone age was advanced in 40.5% patients, with a mean difference from the chronological age of 1.8 (±2.3) years. Patients were more frequently overweight (27%) or obese (22%) compared to controls (10.8% and 10.8%, respectively, P < 0.001). No consistent relationship between glucocorticoid dose and anthropometric measurements or hormonal biomarkers was detected. A small number of patients had raised total cholesterol (3.0%), low HDL (3.0%), raised LDL (7.0%) and triglycerides (5.0%). SDQ scores were within the 'high' and 'very high' categories of concern for 16.3% of patients. 'School functioning' was the lowest PedsQL scoring dimension with a median (interquartile range) of 70 (55-80), followed by 'emotional functioning' with a median of 75 (65-85).
Conclusions: Our results show an increased prevalence of problems with growth and weight gain in CAH children and suggest reduced quality of life. This highlights the urgent need to optimise management and monitoring strategies to improve long-term health outcomes.
Figures

Similar articles
-
Quality of Life in Children and Young People With Congenital Adrenal Hyperplasia-UK Nationwide Multicenter Assessment.J Clin Endocrinol Metab. 2023 Dec 21;109(1):e336-e346. doi: 10.1210/clinem/dgad405. J Clin Endocrinol Metab. 2023. PMID: 37439248
-
Quality of life in adults with congenital adrenal hyperplasia relates to glucocorticoid treatment, adiposity and insulin resistance: United Kingdom Congenital adrenal Hyperplasia Adult Study Executive (CaHASE).Eur J Endocrinol. 2013 May 3;168(6):887-93. doi: 10.1530/EJE-13-0128. Print 2013 Jun. Eur J Endocrinol. 2013. PMID: 23520247 Free PMC article.
-
Glucocorticoid replacement regimens for treating congenital adrenal hyperplasia.Cochrane Database Syst Rev. 2020 Mar 19;3(3):CD012517. doi: 10.1002/14651858.CD012517.pub2. Cochrane Database Syst Rev. 2020. PMID: 32190901 Free PMC article.
-
Obesity among children and adolescents with classic congenital adrenal hyperplasia due to 21-hydroxylase deficiency.Pediatrics. 2006 Jan;117(1):e98-105. doi: 10.1542/peds.2005-1005. Pediatrics. 2006. PMID: 16396852
-
Growth patterns and final height in congenital adrenal hyperplasia due to classical 21-hydroxylase deficiency. Results of a multicenter study.Horm Res. 2001;55(4):161-71. doi: 10.1159/000049990. Horm Res. 2001. PMID: 11598369 Review.
Cited by
-
Metabolic Syndrome Spectrum in Children with Classic Congenital Adrenal Hyperplasia-A Comprehensive Review.Metabolites. 2025 Feb 2;15(2):89. doi: 10.3390/metabo15020089. Metabolites. 2025. PMID: 39997713 Free PMC article. Review.
-
Immunophenotypic Implications of Reverse-Circadian Glucocorticoid Treatment in Congenital Adrenal Hyperplasia.Int J Mol Sci. 2025 Feb 10;26(4):1479. doi: 10.3390/ijms26041479. Int J Mol Sci. 2025. PMID: 40003944 Free PMC article.
-
Cardiometabolic Aspects of Congenital Adrenal Hyperplasia.Endocr Rev. 2025 Jan 10;46(1):80-148. doi: 10.1210/endrev/bnae026. Endocr Rev. 2025. PMID: 39240753 Free PMC article. Review.
-
Mental Health Issues Associated With Classic Congenital Adrenal Hyperplasia Due to 21-Hydroxylase Deficiency.J Clin Endocrinol Metab. 2025 Jan 21;110(Supplement_1):S46-S55. doi: 10.1210/clinem/dgae668. J Clin Endocrinol Metab. 2025. PMID: 39836615 Free PMC article. Review.
References
-
- Claahsen-van der Grinten HL, Speiser PW, Ahmed SF, Arlt W, Auchus RJ, Falhammar H, Flück CE, Guasti L, Huebner A, Kortmann BBMet al.Congenital adrenal hyperplasia – current insights in pathophysiology, diagnostics and management. Endocrine Reviews 20224391–159. (10.1210/endrev/bnab016) - DOI - PMC - PubMed
-
- Speiser PW, Arlt W, Auchus RJ, Baskin LS, Conway GS, Merke DP, Meyer-Bahlburg HFL, Miller WL, Murad MH, Oberfield SEet al.Congenital adrenal hyperplasia due to steroid 21-hydroxylase deficiency: an Endocrine Society clinical practice guideline. Journal of Clinical Endocrinology and Metabolism 20181034043–4088. (10.1210/jc.2018-01865) - DOI - PMC - PubMed
-
- Bacila I, Freeman N, Daniel E, Sandrk M, Bryce J, Ali SR, Yavas Abali Z, Atapattu N, Bachega TA, Balsamo Aet al.International practice of corticosteroid replacement therapy in congenital adrenal hyperplasia: data from the I-CAH registry. European Journal of Endocrinology 2021184553–563. (10.1530/EJE-20-1249) - DOI - PubMed

