Targeting the tamoxifen receptor within sodium channels to block osteoarthritic pain
- PMID: 36001977
- PMCID: PMC9523973
- DOI: 10.1016/j.celrep.2022.111248
Targeting the tamoxifen receptor within sodium channels to block osteoarthritic pain
Abstract
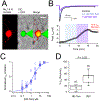
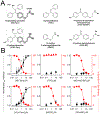
Voltage-gated sodium channels (NaV) in nociceptive neurons initiate action potentials required for transmission of aberrant painful stimuli observed in osteoarthritis (OA). Targeting NaV subtypes with drugs to produce analgesic effects for OA pain management is a developing therapeutic area. Previously, we determined the receptor site for the tamoxifen analog N-desmethyltamoxifen (ND-Tam) within a prokaryotic NaV. Here, we report the pharmacology of ND-Tam against eukaryotic NaVs natively expressed in nociceptive neurons. ND-Tam and analogs occupy two conserved intracellular receptor sites in domains II and IV of NaV1.7 to block ion entry using a "bind and plug" mechanism. We find that ND-Tam inhibition of the sodium current is state dependent, conferring a potent frequency- and voltage-dependent block of hyperexcitable nociceptive neuron action potentials implicated in OA pain. When evaluated using a mouse OA pain model, ND-Tam has long-lasting efficacy, which supports the potential of repurposing ND-Tam analogs as NaV antagonists for OA pain management.
Keywords: CP: Neuroscience; DRG neurons; molecular pharmacology; nociceptors; osteoarthritis; pain; sodium channel.
Copyright © 2022 The Authors. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Declaration of interests The authors declare no competing interests.
Figures




Similar articles
-
Pharmacologic Characterization of LTGO-33, a Selective Small Molecule Inhibitor of the Voltage-Gated Sodium Channel NaV1.8 with a Unique Mechanism of Action.Mol Pharmacol. 2024 Feb 15;105(3):233-249. doi: 10.1124/molpharm.123.000789. Mol Pharmacol. 2024. PMID: 38195157
-
NaV 1.6 regulates excitability of mechanosensitive sensory neurons.J Physiol. 2019 Jul;597(14):3751-3768. doi: 10.1113/JP278148. Epub 2019 May 13. J Physiol. 2019. PMID: 31087362
-
Cannabidiol Inhibition of Murine Primary Nociceptors: Tight Binding to Slow Inactivated States of Nav1.8 Channels.J Neurosci. 2021 Jul 28;41(30):6371-6387. doi: 10.1523/JNEUROSCI.3216-20.2021. Epub 2021 Jun 15. J Neurosci. 2021. PMID: 34131037 Free PMC article.
-
Analgesic potential of voltage gated sodium channel modulators for the management of pain.Curr Opin Pharmacol. 2024 Apr;75:102433. doi: 10.1016/j.coph.2024.102433. Epub 2024 Jan 25. Curr Opin Pharmacol. 2024. PMID: 38277942 Review.
-
Structural Pharmacology of Voltage-Gated Sodium Channels.J Mol Biol. 2021 Aug 20;433(17):166967. doi: 10.1016/j.jmb.2021.166967. Epub 2021 Mar 29. J Mol Biol. 2021. PMID: 33794261 Review.
Cited by
-
A Novel Quantitative Electrocardiography Strategy Reveals the Electroinhibitory Effect of Tamoxifen on the Mouse Heart.J Cardiovasc Transl Res. 2023 Oct;16(5):1232-1248. doi: 10.1007/s12265-023-10395-5. Epub 2023 May 8. J Cardiovasc Transl Res. 2023. PMID: 37155136
-
Sensory neuron-specific block of multifaceted sodium channels mitigates neuropathic pain behaviors of osteoarthritis.Pain Rep. 2025 May 27;10(4):e1288. doi: 10.1097/PR9.0000000000001288. eCollection 2025 Aug. Pain Rep. 2025. PMID: 40444021 Free PMC article.
References
-
- AKOPIAN AN, SIVILOTTI L & WOOD JN 1996. A tetrodotoxin-resistant voltage-gated sodium channel expressed by sensory neurons. Nature, 379, 257–62. - PubMed
-
- CASTANEDA-CASTELLANOS DR, NIKONOROV I, KALLEN RG & RECIO-PINTO E 2002. Lidocaine stabilizes the open state of CNS voltage-dependent sodium channels. Brain Res Mol Brain Res, 99, 102–13. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

