Comparison of perioperative outcomes with or without routine chest tube drainage after video-assisted thoracoscopic pulmonary resection: A systematic review and meta-analysis
- PMID: 36003771
- PMCID: PMC9393739
- DOI: 10.3389/fonc.2022.915020
Comparison of perioperative outcomes with or without routine chest tube drainage after video-assisted thoracoscopic pulmonary resection: A systematic review and meta-analysis
Abstract
Background: In recent years, an increasing number of thoracic surgeons have attempted to apply no routine chest tube drainage (NT) strategy after thoracoscopic lung resection. However, the safety and feasibility of not routinely placing a chest tube after lung resection remain controversial. This study aimed to investigate the effect of NT strategy after thoracoscopic pulmonary resection on perioperative outcomes.
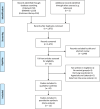
Methods: A comprehensive literature search of PubMed, Embase, and the Cochrane Library databases until 3 January 2022 was performed to identify the studies that implemented NT strategy after thoracoscopic pulmonary resection. Perioperative outcomes were extracted by 2 reviewers independently and then synthesized using a random-effects model. Risk ratio (RR) and standardized mean difference (SMD) with 95% confidence interval (CI) served as the summary statistics for meta-analysis. Subgroup analysis and sensitivity analysis were subsequently performed.
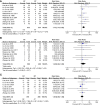
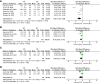
Results: A total of 12 studies with 1,381 patients were included. The meta-analysis indicated that patients in the NT group had a significantly reduced postoperative length of stay (LOS) (SMD = -0.91; 95% CI: -1.20 to -0.61; P < 0.001) and pain score on postoperative day (POD) 1 (SMD = -0.95; 95% CI: -1.54 to -0.36; P = 0.002), POD 2 (SMD = -0.37; 95% CI: -0.63 to -0.11; P = 0.005), and POD 3 (SMD = -0.39; 95% CI: -0.71 to -0.06; P = 0.02). Further subgroup analysis showed that the difference of postoperative LOS became statistically insignificant in the lobectomy or segmentectomy subgroup (SMD = -0.30; 95% CI: -0.91 to 0.32; P = 0.34). Although the risk of pneumothorax was significantly higher in the NT group (RR = 1.75; 95% CI: 1.14-2.68; P = 0.01), the reintervention rates were comparable between groups (RR = 1.04; 95% CI: 0.48-2.25; P = 0.92). No significant difference was found in pleural effusion, subcutaneous emphysema, operation time, pain score on POD 7, and wound healing satisfactory (all P > 0.05). The sensitivity analysis suggested that the results of the meta-analysis were stabilized.
Conclusions: This meta-analysis suggested that NT strategy is safe and feasible for selected patients scheduled for video-assisted thoracoscopic pulmonary resection.
Systematic review registration: https://inplasy.com/inplasy-2022-4-0026, identifier INPLASY202240026.
Keywords: meta-analysis; no routine chest tube drainage strategy; perioperative outcomes; systematic review; traditional chest tube drainage; video-assisted thoracoscopic lung resection.
Copyright © 2022 Li, Qiu, Qu, Ma, Wang, Zhang, Yue and Tian.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



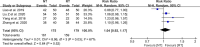
References
-
- Potter AL, Rosenstein AL, Kiang MV, Shah SA, Gaissert HA, Chang DC, et al. Association of computed tomography screening with lung cancer stage shift and survival in the United States: Quasi-experimental study. BMJ (Clinical Res ed) (2022) 376:e069008. doi: 10.1136/bmj-2021-069008 - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials

