Risk of Macrovascular and Microvascular Disease in Diabetes Diagnosed Using Oral Glucose Tolerance Test With and Without Confirmation by Hemoglobin A1c: The Whitehall II Cohort Study
- PMID: 36004644
- PMCID: PMC9508989
- DOI: 10.1161/CIRCULATIONAHA.122.059430
Risk of Macrovascular and Microvascular Disease in Diabetes Diagnosed Using Oral Glucose Tolerance Test With and Without Confirmation by Hemoglobin A1c: The Whitehall II Cohort Study
Abstract
Background: It is unclear whether replacing oral glucose tolerance test (OGTT) with hemoglobin A1c (HbA1c) measurement for diagnosing diabetes is justified. We aimed to assess the proportion of OGTT-diagnosed diabetes cases that can be confirmed by HbA1c and to examine whether individuals with OGTT diagnosis but nondiagnostic HbA1c are at higher risk of macrovascular and microvascular disease.
Methods: Participants were 5773 men and women from the population-based Whitehall II prospective cohort study in the United Kingdom. New OGTT diabetes cases diagnosed in clinical examinations in 2002 to 2004 and 2007 to 2009 were assessed for HbA1c confirmation (≥6.5%) in these and subsequent clinical examinations in 2012 to 2013 and 2015 to 2016. All participants were followed up for major cardiovascular events through linkage to electronic health records until 2017 and for incident chronic kidney disease (estimated glomerular filtration rate <60 mL·min-1·1.73 m-2) until the last clinical examination. In analysis of vascular disease risk, new OGTT-diagnosed diabetes cases with and without diagnostic HbA1c and preexisting diabetes cases were compared with diabetes-free participants.
Results: Of the 378 (59.3%) participants with OGTT-diagnosed diabetes, 224 were confirmed by HbA1c during 4.1 years (SD, 4.1 years) of follow-up. We recorded 942 cardiovascular events over 12.1 years. After adjustment for nonmodifiable risk factors and compared with the 4997 diabetes-free participants, 371 participants with new HbA1c-confirmed diabetes and 405 participants with preexisting diabetes had increased risk of cardiovascular disease (hazard ratio, 1.53 [95% CI, 1.12-2.10] and 1.85 [95% CI, 1.50-2.28], respectively). The corresponding hazard ratios in the analysis of incident chronic kidney disease (487 cases; follow-up, 6.6 years) were 1.69 (95% CI, 1.09-2.62) for 282 participants with new HbA1c-confirmed diabetes and 1.67 (95% CI, 1.22-2.28) for 276 participants with preexisting diabetes. In both analyses, OGTT cases with nondiagnostic HbA1c (n=149 and 107) had a risk (hazard ratio, 0.99-1.07) similar to that of the diabetes-free population.
Conclusions: More than 40% of OGTT-diagnosed diabetes cases were not confirmed by HbA1c during an extended follow-up. However, because these individuals have a risk of cardiovascular disease and chronic kidney disease similar to that of the diabetes-free population, replacement of OGTT with HbA1c-based diagnosis appears justified.
Keywords: cardiovascular diseases; cohort studies; diabetes mellitus, type 2; glucose tolerance test; glycated hemoglobin A; renal insufficiency, chronic.
Figures

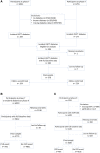


Comment in
-
Letter by Schmidt et al Regarding Article, "Risk of Macrovascular and Microvascular Disease in Diabetes Diagnosed Using Oral Glucose Tolerance Test With and Without Confirmation by Hemoglobin A1c: The Whitehall II Cohort Study".Circulation. 2023 Mar 21;147(12):987. doi: 10.1161/CIRCULATIONAHA.122.062745. Epub 2023 Mar 21. Circulation. 2023. PMID: 36944034 No abstract available.
-
Letter by Deng et al Regarding Article, "Risk of Macrovascular and Microvascular Disease in Diabetes Diagnosed Using Oral Glucose Tolerance Test With and Without Confirmation by Hemoglobin A1c: The Whitehall II Cohort Study".Circulation. 2023 Mar 21;147(12):985-986. doi: 10.1161/CIRCULATIONAHA.122.062624. Epub 2023 Mar 21. Circulation. 2023. PMID: 36944035 No abstract available.
-
Response by Tabák et al to Letters Regarding Article, "Risk of Macrovascular and Microvascular Disease in Diabetes Diagnosed Using Oral Glucose Tolerance Test With and Without Confirmation by Hemoglobin A1c: The Whitehall II Cohort Study".Circulation. 2023 Mar 21;147(12):988-989. doi: 10.1161/CIRCULATIONAHA.123.063545. Epub 2023 Mar 21. Circulation. 2023. PMID: 36944036 Free PMC article. No abstract available.
References
-
- Barry E, Roberts S, Oke J, Vijayaraghavan S, Normansell R, Greenhalgh T. Efficacy and effectiveness of screen and treat policies in prevention of type 2 diabetes: systematic review and meta-analysis of screening tests and interventions. BMJ. 2017;356:i6538. doi: 10.1136/bmj.i6538 - PubMed
-
- NCD Risk Factor Collaboration (NCD-RisC). Effects of diabetes definition on global surveillance of diabetes prevalence and diagnosis: a pooled analysis of 96 population-based studies with 331,288 participants. Lancet Diabetes Endocrinol. 2015;3:624–637. doi: 10.1016/S2213-8587(15)00129-1 - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

