Effect of Hyperthyroidism Treatments on Heart Rate Variability: A Systematic Review and Meta-Analysis
- PMID: 36009529
- PMCID: PMC9405700
- DOI: 10.3390/biomedicines10081982
Effect of Hyperthyroidism Treatments on Heart Rate Variability: A Systematic Review and Meta-Analysis
Abstract
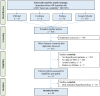
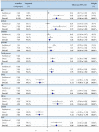
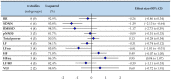
The reversibility of HRV abnormalities in hyperthyroidism remains contradictory. The design of this study involves conducting a systematic review and meta-analysis on the effect of antithyroid treatments on HRV in hyperthyroidism. PubMed, Cochrane, Embase, and Google Scholar were searched until 4 April 2022. Multiple reviewers selected articles reporting HRV parameters in treated and untreated hyperthyroidism. Independent data extraction by multiple observers was stratified by degree of hyperthyroidism for each HRV parameter: RR intervals, SDNN (standard deviation of RR intervals), RMSSD (square root of the mean difference of successive RR intervals), pNN50 (percentage of RR intervals with >50 ms of variation), total power (TP), LFnu (low-frequency normalized unit) and HFnu (high-frequency), VLF (very low-frequency), and LF/HF ratio. We included 11 studies for a total of 471 treated hyperthyroid patients, 495 untreated hyperthyroid patients, and 781 healthy controls. After treatment, there was an increase in RR, SDNN, RMSSD, pNN50, TP, HFnu, and VLF and a decrease in LFnu and LF/HF ratio (p < 0.01). Overt hyperthyroidism showed similar results, in contrast to subclinical hyperthyroidism. Compared with controls, some HRV parameter abnormalities persist in treated hyperthyroid patients (p < 0.05) with lower SDNN, LFnu, and higher HFnu, without significant difference in other parameters. We showed a partial reversibility of HRV abnormalities following treatment of overt hyperthyroidism. The improvement in HRV may translate the clinical cardiovascular benefits of treatments in hyperthyroidism and may help to follow the evolution of the cardiovascular morbidity.
Keywords: antithyroid treatment; autonomic nervous activity; biomarker; prevention; public health; thyroid.
Conflict of interest statement
The authors declare that there are no conflicts of interest that could be perceived as prejudicing the impartiality of this review.
Figures


References
-
- Demers L., Spencer C. Pathophysiology and thyroid function testing. In: Burtis C.A., Ashwood E.R., Bruns D.E., editors. Tietz Textbook of Clinical Chemistry and Molecular Diagnostics. W.B Saunders; Washington, DC, USA: 2006. pp. 2053–2096.
-
- Delemer B. Traité d’Endocrinologie. 2nd ed. Lavoisier; Paris, France: 2019. Hyperthyroïdie: Signes cliniques et diagnostic étiologique; pp. 187–192. Lavoisier Médecine Sciences.
-
- Clerc J. Traité d’Endocrinologie. 2nd ed. Lavoisier; Paris, France: 2019. Traitement de l’hyperthyroïdie et des goitres par l’iode radioactif; pp. 251–261. Lavoisier Médecine Sciences.
-
- Collet T.-H., Gussekloo J., Bauer D.C., Den Elzen P.J., Cappola A.R., Balmer P., Iervasi G., Åsvold B.O., Sgarbi J.A., Völzke H., et al. Subclinical Hyperthyroidism and the Risk of Coronary Heart Disease and Mortality. Arch. Intern. Med. 2012;172:799–809. doi: 10.1001/archinternmed.2012.402. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

