Suppression of Cardiogenic Edema with Sodium-Glucose Cotransporter-2 Inhibitors in Heart Failure with Reduced Ejection Fraction: Mechanisms and Insights from Pre-Clinical Studies
- PMID: 36009562
- PMCID: PMC9405937
- DOI: 10.3390/biomedicines10082016
Suppression of Cardiogenic Edema with Sodium-Glucose Cotransporter-2 Inhibitors in Heart Failure with Reduced Ejection Fraction: Mechanisms and Insights from Pre-Clinical Studies
Abstract
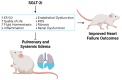
In heart failure with reduced ejection fraction (HFrEF), cardiogenic edema develops from impaired cardiac function, pathological remodeling, chronic inflammation, endothelial dysfunction, neurohormonal activation, and altered nitric oxide-related pathways. Pre-clinical HFrEF studies have shown that treatment with sodium-glucose cotransporter-2 inhibitors (SGLT-2i) stimulates natriuretic and osmotic/diuretic effects, improves overall cardiac function, attenuates maladaptive cardiac remodeling, and reduces chronic inflammation, oxidative stress, and endothelial dysfunction. Here, we review the mechanisms and effects of SGLT-2i therapy on cardiogenic edema in various models of HFrEF. Overall, the data presented suggest a high translational importance of these studies, and pre-clinical studies show that SGLT-2i therapy has a marked effect on suppressing the progression of HFrEF through multiple mechanisms, including those that affect the development of cardiogenic edema.
Keywords: HFrEF; cardiac remodeling; dilated cardiomyopathy; edema; endothelial dysfunction; excessive extracellular fluid; fluid management; inflammation.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
Sodium-Glucose Cotransporter-2 Inhibitors Improve Heart Failure with Reduced Ejection Fraction Outcomes by Reducing Edema and Congestion.Diagnostics (Basel). 2022 Apr 14;12(4):989. doi: 10.3390/diagnostics12040989. Diagnostics (Basel). 2022. PMID: 35454037 Free PMC article. Review.
-
SGLT-2 Inhibitors for Patients with Heart Failure: What Have We Learned Recently?Curr Atheroscler Rep. 2022 Aug;24(8):627-634. doi: 10.1007/s11883-022-01038-2. Epub 2022 Jun 2. Curr Atheroscler Rep. 2022. PMID: 35653033 Review.
-
Sodium-Glucose Cotransporter 2 Inhibitor Use Among Individuals Age <65 with Type 2 Diabetes and Heart Failure with Reduced Ejection Fraction: A Cost-Benefit Analysis.Clinicoecon Outcomes Res. 2022 Jul 9;14:465-477. doi: 10.2147/CEOR.S361886. eCollection 2022. Clinicoecon Outcomes Res. 2022. PMID: 35845354 Free PMC article.
-
Use of Sodium-Glucose Cotransporter-2 Inhibitors in Clinical Practice for Heart Failure Prevention and Treatment: Beyond Type 2 Diabetes. A Narrative Review.Adv Ther. 2022 Feb;39(2):845-861. doi: 10.1007/s12325-021-01989-z. Epub 2021 Dec 9. Adv Ther. 2022. PMID: 34881413 Free PMC article. Review.
-
Ventricular remodeling and hemodynamic changes in heart failure patients with non-ischemic dilated cardiomyopathy following dapagliflozin initiation.Egypt Heart J. 2024 Jun 18;76(1):76. doi: 10.1186/s43044-024-00508-z. Egypt Heart J. 2024. PMID: 38888761 Free PMC article.
Cited by
-
Sizing SGLT2 Inhibitors Up: From a Molecular to a Morpho-Functional Point of View.Int J Mol Sci. 2023 Sep 8;24(18):13848. doi: 10.3390/ijms241813848. Int J Mol Sci. 2023. PMID: 37762152 Free PMC article. Review.
-
Editorial of the Special Issue: Cellular Mechanisms of Cardiovascular Disease.Biomedicines. 2023 Sep 8;11(9):2494. doi: 10.3390/biomedicines11092494. Biomedicines. 2023. PMID: 37760934 Free PMC article.
-
Antioxidant Effects of SGLT2 Inhibitors on Cardiovascular-Kidney-Metabolic (CKM) Syndrome.Antioxidants (Basel). 2025 Jun 9;14(6):701. doi: 10.3390/antiox14060701. Antioxidants (Basel). 2025. PMID: 40563333 Free PMC article. Review.
-
The Impact of SGLT2 Inhibitor Dapagliflozin on Adropin Serum Levels in Men and Women with Type 2 Diabetes Mellitus and Chronic Heart Failure.Biomedicines. 2023 Feb 4;11(2):457. doi: 10.3390/biomedicines11020457. Biomedicines. 2023. PMID: 36830993 Free PMC article.
-
Editorial: Edema in heart failure with reduced ejection fraction.Front Cardiovasc Med. 2023 Feb 7;10:1141937. doi: 10.3389/fcvm.2023.1141937. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 36824450 Free PMC article. No abstract available.
References
-
- Virani S.S., Alonso A., Aparicio H.J., Benjamin E.J., Bittencourt M.S., Callaway C.W., Carson A.P., Chamberlain A.M., Cheng S., Delling F.N., et al. Heart Disease and Stroke Statistics-2021 Update: A Report from the American Heart Association. Circulation. 2021;143:e254–e743. doi: 10.1161/CIR.0000000000000950. - DOI - PubMed
-
- Benjamin E.J., Muntner P., Alonso A., Bittencourt M.S., Callaway C.W., Carson A.P., Chamberlain A.M., Chang A.R., Cheng S., Das S.R., et al. Heart Disease and Stroke Statistics-2019 Update: A Report from the American Heart Association. Circulation. 2019;139:e56–e528. doi: 10.1161/CIR.0000000000000659. - DOI - PubMed
-
- Bozkurt B., Coats A.J.S., Tsutsui H., Abdelhamid C.M., Adamopoulos S., Albert N., Anker S.D., Atherton J., Bohm M., Butler J., et al. Universal Definition and Classification of Heart Failure: A Report of the Heart Failure Society of America, Heart Failure Association of the European Society of Cardiology, Japanese Heart Failure Society and Writing Committee of the Universal Definition of Heart Failure: Endorsed by the Canadian Heart Failure Society, Heart Failure Association of India, Cardiac Society of Australia and New Zealand, and Chinese Heart Failure Association. Eur. J. Heart Fail. 2021;23:352–380. doi: 10.1002/ejhf.2115. - DOI - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources