Post-COVID-19 Syndrome is Rarely Associated with Damage of the Nervous System: Findings from a Prospective Observational Cohort Study in 171 Patients
- PMID: 36028604
- PMCID: PMC9417089
- DOI: 10.1007/s40120-022-00395-z
Post-COVID-19 Syndrome is Rarely Associated with Damage of the Nervous System: Findings from a Prospective Observational Cohort Study in 171 Patients
Abstract
Introduction: The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can affect multiple organs. Reports of persistent or newly emergent symptoms, including those related to the nervous system, have increased over the course of the pandemic, leading to the introduction of post-COVID-19 syndrome. However, this novel syndrome is still ill-defined and structured objectification of complaints is scarce. Therefore, we performed a prospective observational cohort study to better define and validate subjective neurological disturbances in patients with post-COVID-19 syndrome.
Methods: A total of 171 patients fulfilling the post-COVID-19 WHO Delphi consensus criteria underwent a comprehensive neurological diagnostic work-up including neurovascular, electrophysiological, and blood analysis. In addition, magnetic resonance imaging (MRI) and lumbar puncture were conducted in subgroups of patients. Furthermore, patients underwent neuropsychological, psychosomatic, and fatigue assessment.
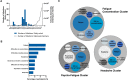
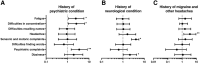
Results: Patients were predominantly female, middle-aged, and had incurred mostly mild-to-moderate acute COVID-19. The most frequent post-COVID-19 complaints included fatigue, difficulties in concentration, and memory deficits. In most patients (85.8%), in-depth neurological assessment yielded no pathological findings. In 97.7% of the cases, either no diagnosis other than post COVID-19 syndrome, or no diagnosis likely related to preceding acute COVID-19 could be established. Sensory or motor complaints were more often associated with a neurological diagnosis other than post-COVID-19 syndrome. Previous psychiatric conditions were identified as a risk factor for developing post-COVID-19 syndrome. We found high somatization scores in our patient group that correlated with cognitive deficits and the extent of fatigue.
Conclusions: Albeit frequently reported by patients, objectifiable affection of the nervous system is rare in post-COVID-19 syndrome. Instead, elevated levels of somatization point towards a pathogenesis potentially involving psychosomatic factors. However, thorough neurological assessment is important in this patient group in order to not miss neurological diseases other than post-COVID-19.
Keywords: COVID-19; Fatigue; Long COVID; Neurological deficits; Neuropsychological assessment; Post-COVID; Somatization.
© 2022. The Author(s).
Figures



Comment in
-
Letter to the Editor Regarding Fleischer et al. Neurological Study Does Not Provide Any Evidence that Long COVID is Psychosomatic.Neurol Ther. 2023 Feb;12(1):329-332. doi: 10.1007/s40120-022-00426-9. Epub 2022 Dec 12. Neurol Ther. 2023. PMID: 36508159 Free PMC article. No abstract available.
References
-
- World Health Organization. WHO Coronavirus (COVID19) dashboard. 2022. https://covid19.who.int
-
- World Health Organization . A clinical case definition of post COVID-19 condition by a Delphi consensus. World Health Organization; 2021.
LinkOut - more resources
Full Text Sources
Miscellaneous

