Visual system assessment for predicting a transition to psychosis
- PMID: 36038544
- PMCID: PMC9424317
- DOI: 10.1038/s41398-022-02111-9
Visual system assessment for predicting a transition to psychosis
Abstract
The field of psychiatry is far from perfect in predicting which individuals will transition to a psychotic disorder. Here, we argue that visual system assessment can help in this regard. Such assessments have generated medium-to-large group differences with individuals prior to or near the first psychotic episode or have shown little influence of illness duration in larger samples of more chronic patients. For example, self-reported visual perceptual distortions-so-called visual basic symptoms-occur in up to 2/3rds of those with non-affective psychosis and have already longitudinally predicted an impending onset of schizophrenia. Possibly predictive psychophysical markers include enhanced contrast sensitivity, prolonged backward masking, muted collinear facilitation, reduced stereoscopic depth perception, impaired contour and shape integration, and spatially restricted exploratory eye movements. Promising brain-based markers include visual thalamo-cortical hyperconnectivity, decreased occipital gamma band power during visual detection (MEG), and reduced visually evoked occipital P1 amplitudes (EEG). Potentially predictive retinal markers include diminished cone a- and b-wave amplitudes and an attenuated photopic flicker response during electroretinography. The foregoing assessments are often well-described mechanistically, implying that their findings could readily shed light on the underlying pathophysiological changes that precede or accompany a transition to psychosis. The retinal and psychophysical assessments in particular are inexpensive, well-tolerated, easy to administer, and brief, with few inclusion/exclusion criteria. Therefore, across all major levels of analysis-from phenomenology to behavior to brain and retinal functioning-visual system assessment could complement and improve upon existing methods for predicting which individuals go on to develop a psychotic disorder.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


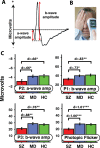
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

