Venous waveform analysis detects acute right ventricular failure in a rat respiratory arrest model
- PMID: 36042330
- PMCID: PMC9971354
- DOI: 10.1038/s41390-022-02278-3
Venous waveform analysis detects acute right ventricular failure in a rat respiratory arrest model
Abstract
Background: Peripheral intravenous analysis (PIVA) has been shown to be more sensitive than central venous pressure (CVP) for detecting hemorrhage and volume overload. We hypothesized that PIVA is superior to CVP for detecting right ventricular (RV) failure in a rat model of respiratory arrest.
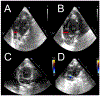
Methods: Eight Wistar rats were studied in accordance with the ARRIVE guidelines. CVP, mean arterial pressure (MAP), and PIVA were recorded. Respiratory arrest was achieved with IV Rocuronium. PIVA utilizes Fourier transform to quantify the amplitude of the peripheral venous waveform, expressed as the "f1 amplitude". RV diameter was measured with transthoracic echocardiography.
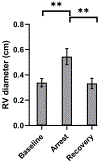
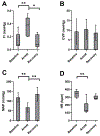
Results: RV diameter increased from 0.34 to 0.54 cm during arrest, p = 0.001, and returned to 0.33 cm post arrest, p = 0.97. There was an increase in f1 amplitude from 0.07 to 0.38 mmHg, p = 0.01 and returned to 0.08 mmHg, p = 1.0. MAP decreased from 119 to 67 mmHg, p = 0.004 and returned to 136 mmHg, p = 0.50. There was no significant increase in CVP from 9.3 mmHg at baseline to 10.5 mmHg during respiratory arrest, p = 0.91, and recovery to 8.6 mmHg, p = 0.81.
Conclusions: This study highlights the utility of PIVA to detect RV failure in small-caliber vessels, comparable to peripheral veins in the human pediatric population.
Impact: Right ventricular failure remains a diagnostic challenge, particularly in pediatric patients with small vessel sizes limiting invasive intravascular monitor use. Intravenous analysis has shown promise in detecting hypovolemia and volume overload. Intravenous analysis successfully detects right ventricular failure in a rat respiratory arrest model. Intravenous analysis showed utility despite utilizing small peripheral venous access and therefore may be applicable to a pediatric population. Intravenous analysis may be helpful in differentiating various types of shock.
© 2022. The Author(s), under exclusive licence to the International Pediatric Research Foundation, Inc.
Conflict of interest statement
Figures


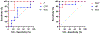
References
-
- Morray JP et al. Anesthesia-Related Cardiac Arrest in Children: Initial Findings of the Pediatric Perioperative Cardiac Arrest (Poca) Registry. Anesthesiology 93, 6–14 (2000). - PubMed
-
- McMahon CJ et al. Preterm Infants with Congenital Heart Disease and Bronchopulmonary Dysplasia: Postoperative Course and Outcome after Cardiac Surgery. Pediatrics 116, 423–430 (2005). - PubMed
-
- de Boer JM, Kuipers IM, Klitsie LM, Blom NA & Ten Harkel AD Decreased Biventricular Longitudinal Strain Shortly after Congenital Heart Defect Surgery. Echocardiography 34, 446–452 (2017). - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

