Comparison of treatment methods for submacular hemorrhage in neovascular age-related macular degeneration: conservative versus active surgical strategy
- PMID: 36050401
- PMCID: PMC9436992
- DOI: 10.1038/s41598-022-18619-5
Comparison of treatment methods for submacular hemorrhage in neovascular age-related macular degeneration: conservative versus active surgical strategy
Abstract
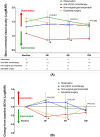
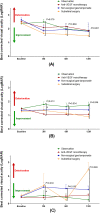
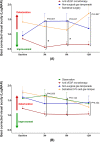
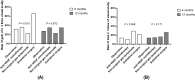
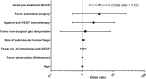
The optimal treatment of submacular hemorrhage (SMH) following neovascular age-related macular degeneration (nAMD) is controversial. This study aimed to compare visual outcomes of conservative versus active surgical treatment. Two hundred thirty-six eyes of 236 patients with SMH (≥ 1 disc diameter) were stratified into four groups: observation (n = 21); anti-vascular endothelial growth factor (VEGF) monotherapy (n = 161); non-surgical gas tamponade (n = 31); and subretinal surgery (n = 23). The primary outcome was best-corrected visual acuity (BCVA) at 12 months. The baseline BCVAs of the observation, anti-VEGF monotherapy, non-surgical gas tamponade, and subretinal surgery groups were 1.50 ± 0.70, 1.09 ± 0.70, 1.31 ± 0.83, and 1.62 ± 0.77 logarithm of minimal angle resolution (LogMAR), respectively. The mean BCVAs at 12 months were 1.39 ± 0.84, 0.90 ± 0.83, 1.35 ± 0.88, and 1.44 ± 0.91 LogMAR, respectively. After adjusting for age, baseline BCVA, SMH size, and the number of intravitreal anti-VEGF injections before SMH, the mean BCVA showed no significant difference among treatments at 12 months (P = 0.204). The anti-VEGF monotherapy group showed better mean BCVA significantly at 3 months (P < 0.001). Only baseline BCVA was associated with VA gain at 12 months (Odds ratio = 3.53, P < 0.001). This study demonstrated that there was no difference in 12 month visual outcomes among treatments and a better early visual outcome can be expected with anti-VEGF monotherapy.
© 2022. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Intravitreal anti-vascular endothelial growth factor monotherapy for large submacular hemorrhage secondary to neovascular age-related macular degeneration.Eye (Lond). 2015 Sep;29(9):1141-51. doi: 10.1038/eye.2015.131. Epub 2015 Aug 14. Eye (Lond). 2015. PMID: 26272443 Free PMC article.
-
The role of pigment epithelial detachment in AMD with submacular hemorrhage treated with vitrectomy and subretinal co-application of rtPA and anti-VEGF.Graefes Arch Clin Exp Ophthalmol. 2017 Jun;255(6):1115-1123. doi: 10.1007/s00417-017-3620-2. Epub 2017 Mar 9. Graefes Arch Clin Exp Ophthalmol. 2017. PMID: 28280989
-
Vitrectomy, subretinal Tissue plasminogen activator and Intravitreal Gas for submacular haemorrhage secondary to Exudative Age-Related macular degeneration (TIGER): study protocol for a phase 3, pan-European, two-group, non-commercial, active-control, observer-masked, superiority, randomised controlled surgical trial.Trials. 2022 Jan 31;23(1):99. doi: 10.1186/s13063-021-05966-3. Trials. 2022. PMID: 35101110 Free PMC article.
-
Comparison of subretinal versus intravitreal injection of recombinant tissue plasminogen activator with gas for submacular hemorrhage secondary to wet age-related macular degeneration: treatment outcomes and brief literature review.Int Ophthalmol. 2021 Dec;41(12):4037-4046. doi: 10.1007/s10792-021-01976-x. Epub 2021 Jul 30. Int Ophthalmol. 2021. PMID: 34331185 Review.
-
Antiplatelet and anticoagulant therapy in patients with submacular hemorrhage caused by neovascular age-related macular degeneration.Graefes Arch Clin Exp Ophthalmol. 2023 May;261(5):1413-1421. doi: 10.1007/s00417-022-05885-2. Epub 2022 Nov 29. Graefes Arch Clin Exp Ophthalmol. 2023. PMID: 36445445 Free PMC article. Review.
Cited by
-
Comparison of different treatment options in submacular haemorrhage.BMC Ophthalmol. 2024 Dec 9;24(1):525. doi: 10.1186/s12886-024-03794-y. BMC Ophthalmol. 2024. PMID: 39654042 Free PMC article.
-
Pneumatic displacement of submacular haemorrhage secondary to neovascular age-related macular degeneration and polypoidal choroidal vasculopathy.Eye (Lond). 2024 Dec;38(17):3374-3381. doi: 10.1038/s41433-024-03318-4. Epub 2024 Sep 19. Eye (Lond). 2024. PMID: 39294233
-
Comparison Between Intravitreal Anti-Vascular Endothelial Growth Factor Monotherapy and Vitrectomy in Age-Related Macular Degeneration with Large Submacular Hemorrhages.J Clin Med. 2025 Feb 22;14(5):1477. doi: 10.3390/jcm14051477. J Clin Med. 2025. PMID: 40094950 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

