Biliary atresia and congenital disorders of the extrahepatic bile ducts
- PMID: 36051179
- PMCID: PMC9297290
- DOI: 10.4292/wjgpt.v13.i4.33
Biliary atresia and congenital disorders of the extrahepatic bile ducts
Abstract
Biliary atresia (BA) and choledochal cysts are diseases of the intrahepatic and extrahepatic biliary tree. While their exact etiopathogeneses are not known, they should be treated promptly due to the potential for irreversible parenchymal liver disease. A diagnosis of BA may be easy or complicated, but should not be delayed. BA is always treated surgically, and performing the surgery before the age of 2 mo greatly increases its effectiveness and extends the time until the need for liver transplantation arises. While the more common types of choledochal cysts require surgical treatment, some can be treated with endoscopic retrograde cholangiopancreatography. Choledochal cysts may cause recurrent cholangitis and the potential for malignancy should not be ignored.
Keywords: Bilier atresia; Choledochal cyst; Cholestasis; Conjugated hyperbilirubinemia.
©The Author(s) 2022. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: All the authors report no relevant conflicts of interest for this article.
Figures

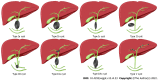
References
-
- Satrom KM, Gourley GR, Neonatal jaundice and disorders of bilirubin metabolism. In: Suchy FJ, Sokol RJ, Balistreri WF, Bezerra JA, Mack CL, Shneider BL, editors. Liver Disease in Children 5th ed. Cambridge: Cambridge University Press; 2021: 182-203.
-
- Fawaz R, Baumann U, Ekong U, Fischler B, Hadzic N, Mack CL, McLin VA, Molleston JP, Neimark E, Ng VL, Karpen SJ. Guideline for the Evaluation of Cholestatic Jaundice in Infants: Joint Recommendations of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition. J Pediatr Gastroenterol Nutr. 2017;64:154–168. - PubMed
-
- Haber BA, Russo P. Biliary atresia. Gastroenterol Clin North Am. 2003;32:891–911. - PubMed
-
- Todani T, Watanabe Y, Toki A, Morotomi Y. Classification of congenital biliary cystic disease: special reference to type Ic and IVA cysts with primary ductal stricture. J Hepatobiliary Pancreat Surg. 2003;10:340–344. - PubMed
-
- Kelley-Quon LI, Shue E, Burke RV, Smith C, Kling K, Mahdi E, Ourshalimian S, Fenlon M, Dellinger M, Shew SB, Lee J, Padilla B, Inge T, Roach J, Marwan AI, Russell KW, Ignacio R, Fialkowski E, Nijagal A, Im C, Azarow KS, Ostlie DJ, Wang K. The need for early Kasai portoenterostomy: a Western Pediatric Surgery Research Consortium study. Pediatr Surg Int. 2022;38:193–199. - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

