The Renshen Chishao Decoction Could Ameliorate the Acute Lung Injury but Could Not Reduce the Neutrophil Extracellular Traps Formation
- PMID: 36072401
- PMCID: PMC9444383
- DOI: 10.1155/2022/7784148
The Renshen Chishao Decoction Could Ameliorate the Acute Lung Injury but Could Not Reduce the Neutrophil Extracellular Traps Formation
Abstract
The acute lung injury (ALI) causes severe pulmonary diseases, leading to a high mortality rate. The Renshen and Chishao have protective and anti-inflammatory effects against the ALI. To explore the protective effects of the Renshen Chishao (RC) decoction against the ALI, we established the lipopolysaccharide-indued ALI model and randomly divided the mice into seven groups: control group, ALI group, high-dose RC group, middle-dose RC group, low-dose RC group, middle-dose RC group + CXCR2 antagonist group, and ALI + CXCR2 antagonist group. We estimated the lung injury by the hematoxylin and eosin staining, the neutrophil extracellular traps (NETs) formations by the immunofluorescence colocalization and enzyme-linked immunosorbent assay (ELISA), and the CXCR2/CXCL2 pathway by the flow cytometry, ELISA, and real-time polymerase chain reaction. We conducted the high-throughput sequencing and enrichment analyses to explore the potential mechanisms. The results showed that the RC decoction pathologically ameliorated the lipopolysaccharide-induced lung injury and inflammatory response but failed to reduce the circulating and lung tissue NETs formation and the blood neutrophil percent. The high-dose RC decoction increased the plasma CXCL2 level, but the RC decoction had no effects on the neutrophilic CXCR2 levels. Under the inhibition of the CXCR2, the middle-dose RC decoction still decreased the lung injury score but as yet had unobvious influence on the NETs formation. Other potential mechanisms of the RC decoction against the ALI involved the pathways of ribosome and coronavirus disease 2019 (COVID-19); the target genes of inflammatory factors, such as Ccl17, Cxcl17, Cd163, Cxcr5, and Il31ra, and lncRNAs; and the regulations of the respiratory cilia. In conclusion, the RC decoction pathologically ameliorated the lipopolysaccharide-induced lung inflammatory injury via upregulating the CXCL2/CXCR2 pathway but could not reduce the circulating or lung tissue NETs formation.
Copyright © 2022 Miao-En Yao et al.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this article.
Figures



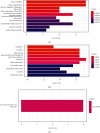





References
LinkOut - more resources
Full Text Sources
Research Materials

