FDG-PET Predicts Neoadjuvant Therapy Response and Survival in Borderline Resectable/Locally Advanced Pancreatic Adenocarcinoma
- PMID: 36075389
- PMCID: PMC12001712
- DOI: 10.6004/jnccn.2022.7041
FDG-PET Predicts Neoadjuvant Therapy Response and Survival in Borderline Resectable/Locally Advanced Pancreatic Adenocarcinoma
Abstract
Background: Neoadjuvant therapy (NAT) is used in borderline resectable/locally advanced (BR/LA) pancreatic ductal adenocarcinoma (PDAC). Anatomic imaging (CT/MRI) poorly predicts response, and biochemical (CA 19-9) markers are not useful (nonsecretors/nonelevated) in many patients. Pathologic response highly predicts survival post-NAT, but is only known postoperatively. Because metabolic imaging (FDG-PET) reveals primary tumor viability, this study aimed to evaluate our experience with preoperative FDG-PET in patients with BR/LA PDAC in predicting NAT response and survival.
Methods: We reviewed all patients with resected BR/LA PDAC who underwent NAT with FDG-PET within 60 days of resection. Pre- and post-NAT metabolic (FDG-PET) and biochemical (CA 19-9) responses were dichotomized in addition to pathologic responses. We compared post-NAT metabolic and biochemical responses as preoperative predictors of pathologic responses and recurrence-free survival (RFS) and overall survival (OS).
Results: We identified 202 eligible patients. Post-NAT, 58% of patients had optimization of CA 19-9 levels. Major metabolic and pathologic responses were present in 51% and 38% of patients, respectively. Median RFS and OS times were 21 and 48.7 months, respectively. Metabolic response was superior to biochemical response in predicting pathologic response (area under the curve, 0.86 vs 0.75; P<.001). Metabolic response was the only univariate preoperative predictor of OS (odds ratio, 0.25; 95% CI, 0.13-0.40), and was highly correlated (P=.001) with pathologic response as opposed to biochemical response alone. After multivariate adjustment, metabolic response was the single largest independent preoperative predictor (P<.001) for pathologic response (odds ratio, 43.2; 95% CI, 16.9-153.2), RFS (hazard ratio, 0.37; 95% CI, 0.2-0.6), and OS (hazard ratio, 0.21; 95% CI, 0.1-0.4).
Conclusions: Among patients with post-NAT resected BR/LA PDAC, FDG-PET highly predicts pathologic response and survival, superior to biochemical responses alone. Given the poor ability of anatomic imaging or biochemical markers to assess NAT responses in these patients, FDG-PET is a preoperative metric of NAT efficacy, thereby allowing potential therapeutic alterations and surgical treatment decisions. We suggest that FDG-PET should be an adjunct and recommended modality during the NAT phase of care for these patients.
Figures

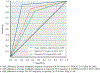
References
-
- Zakem SJ, Mueller AC, Meguid C, et al. Impact of neoadjuvant chemotherapy and stereotactic body radiation therapy (SBRT) on R0 resection rate for borderline resectable and locally advanced pancreatic cancer. HPB (Oxford) 2021;23:1072–1083. - PubMed
-
- Hue JJ, Dorth J, Sugumar K, et al. Neoadjuvant radiotherapy is associated with improved pathologic outcomes and survival in resected stage II-III pancreatic adenocarcinoma treated with multiagent neoadjuvant chemotherapy in the modern era. Am Surg 2021;87:1386–1395. - PubMed
-
- Tempero MA, Malafa MP, AI-Hawary M, et al. NCCN Clinical Practice Guidelines in Oncology: Pancreatic Adenocarcinoma. Version 2.2021 Accessed October 1, 2021. To view the most recent version, visit NCCN.org
-
- Wagner M, Antunes C, Pietrasz D, et al. CT evaluation after neoadjuvant FOLFIRINOX chemotherapy for borderline and locally advanced pancreatic adenocarcinoma. Eur Radiol 2017;27:3104–3116. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

