Body Weight Counts-Cardioversion with Vernakalant or Ibutilide at the Emergency Department
- PMID: 36078991
- PMCID: PMC9456766
- DOI: 10.3390/jcm11175061
Body Weight Counts-Cardioversion with Vernakalant or Ibutilide at the Emergency Department
Abstract
Aim: Medication for the pharmacological cardioversion of atrial fibrillation (AF) and atrial flutter (AFL) is applied either in a fixed dose or adapted to body weight. Individual body weight might be a relevant confounder for anti-arrhythmic treatment success. Therefore, the aim of this study was to elucidate the impact of body weight on pharmacological cardioversion success, comparing weight adapted (Vernakalant) and fixed dose (Ibutilide) pharmacotherapeutic cardioversion regimes.
Methods: Within this prospective observational trial, a total of 316 episodes of AF and AFL were enrolled. Patients were stratified in either a Vernakalant (n = 181) or Ibutilide (n = 135) treatment arm, based on the chosen regime, for direct comparison of treatment efficacy.
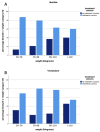
Results: Conversion to sinus rhythm was achieved in 76.3% of all cases. Of note, there was no difference comparing the Vernakalant and Ibutilide treatment arms (Vernakalant 76.2% vs. Ibutilide 76.3%; p = 0.991). Within the whole study population, decreasing conversion rates with increasing body weight (adjusted odds ratio (OR) = 0.69 (0.51-0.94); p = 0.018) were observed. An independent effect of body weight within the Ibutilide treatment arm was noted, which remained stable after adjustment for potential confounders (adjusted OR = 0.55 (0.38-0.92), p = 0.022.
Conclusion: Both, the Vernakalant and Ibutilide treatment arms showed comparable rates of treatment success in pharmacotherapeutic cardioversion of AF and AFL. Of utmost importance, we observed that the fixed dose of Ibutilide-as compared to the weight-adapted dose of Vernakalant-showed a reduced treatment success with increasing body weight.
Keywords: atrial fibrillation; body weight; cardioversion; pharmacological cardioversion.
Conflict of interest statement
Patients treated for AF at the Department of Emergency Medicine, Medical University of Vienna, Austria, have in the past been included in the “Spectrum” registry (Cardiome Pharma Corp.). However, no funding was provided for the current academic study, and there was no influence on the design, conduction, or interpretation of the study in any way.
Figures
References
-
- Hindricks G., Potpara T., Dagres N., Arbelo E., Bax J.J., Blomström-Lundqvist C., Boriani G., Castella M., Dan G., Dilaveris P.E., et al. 2020 ESC guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association of Cardio-Thoracic Surgery (EACTS) Eur. Heart J. 2020;42:373–498. doi: 10.1093/eurheartj/ehaa612. - DOI - PubMed
-
- Stiell I.G., Sivilotti M.L.A., Taljaard M., Birnie D., Vadeboncoeur A., Hohl C.M., McRae A.D., Morris J., Mercier E., Macle L., et al. A randomized, controlled comparison of electrical versus pharmacological cardioversion for emergency department patients with acute atrial flutter. Can. J. Emerg. Med. 2021;23:314–324. doi: 10.1007/s43678-020-00067-7. - DOI - PubMed
-
- Stiell I.G., Sivilotti M.L.A., Taljaard M., Birnie D., Vadeboncoeur A., Hohl C.M., McRae A.D., Morris J., Mercier E., Macle L., et al. Electrical versus pharmacological cardioversion for emergency department patients with acute atrial fibrillation (RAFF2) Lancet. 2020;395:339–349. doi: 10.1016/S0140-6736(19)32994-0. - DOI - PubMed
-
- Denis R., Craig M.P., Torp-Pedersen C., Wyse D.G., Egon T., Juul-Moller S., Nielsen T., Rasmussen S.L., Stiell L.G., Coutu B., et al. Vernakalant hydrochloride for rapid conversion of atrial fibrillation. Circulation. 2008;117:1518–1525. - PubMed
LinkOut - more resources
Full Text Sources