Anticoagulation Strategies during Extracorporeal Membrane Oxygenation: A Narrative Review
- PMID: 36079084
- PMCID: PMC9457503
- DOI: 10.3390/jcm11175147
Anticoagulation Strategies during Extracorporeal Membrane Oxygenation: A Narrative Review
Abstract
The development of extracorporeal life support technology has added a new dimension to the care of critically ill patients who fail conventional treatment options. Extracorporeal membrane oxygenation (ECMO)-specialized temporary life support for patients with severe cardiac or pulmonary failure-plays a role in bridging the time for organ recovery, transplant, or permanent assistance. The overall patient outcome is dependent on the underlying disease, comorbidities, patient reaction to critical illness, and potential adverse events during ECMO. Moreover, the contact of the blood with the large artificial surface of an extracorporeal system circuit triggers complex inflammatory and coagulation responses. These processes may further lead to endothelial injury and disrupted microcirculation with consequent end-organ dysfunction and the development of adverse events like thromboembolism. Therefore, systemic anticoagulation is considered crucial to alleviate the risk of thrombosis and failure of ECMO circuit components. The gold standard and most used anticoagulant during extracorporeal life support is unfractionated heparin, with all its benefits and disadvantages. However, therapeutic anticoagulation of a critically ill patient carries the risk of clinically relevant bleeding with the potential for permanent injury or death. Similarly, thrombotic events may occur. Therefore, different anticoagulation strategies are employed, while the monitoring and the balance of procoagulant and anticoagulatory factors is of immense importance. This narrative review summarizes the most recent considerations on anticoagulation during ECMO support, with a special focus on anticoagulation monitoring and future directions.
Keywords: ECMO; adverse events; anticoagulation; complications; extracorporeal life support; future directions; inflammation; monitoring; mortality.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

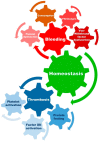
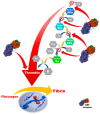
References
-
- Schechter M.A., Ganapathi A.M., Englum B.R., Speicher P.J., Daneshmand M.A., Davis R.D., Hartwig M.G. Spontaneously Breathing Extracorporeal Membrane Oxygenation Support Provides the Optimal Bridge to Lung Transplantation. Transplantation. 2016;100:2699–2704. doi: 10.1097/TP.0000000000001047. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

