The role of sleep state and time of day in modulating breathing in epilepsy: implications for sudden unexpected death in epilepsy
- PMID: 36082111
- PMCID: PMC9445500
- DOI: 10.3389/fncir.2022.983211
The role of sleep state and time of day in modulating breathing in epilepsy: implications for sudden unexpected death in epilepsy
Abstract
Sudden unexpected death in epilepsy (SUDEP) is the leading cause of death among patients with refractory epilepsy. While the exact etiology of SUDEP is unknown, mounting evidence implicates respiratory dysfunction as a precipitating factor in cases of seizure-induced death. Dysregulation of breathing can occur in epilepsy patients during and after seizures as well as interictally, with many epilepsy patients exhibiting sleep-disordered breathing (SDB), such as obstructive sleep apnea (OSA). The majority of SUDEP cases occur during the night, with the victim found prone in or near a bed. As breathing is modulated in both a time-of-day and sleep state-dependent manner, it is relevant to examine the added burden of nocturnal seizures on respiratory function. This review explores the current state of understanding of the relationship between respiratory function, sleep state and time of day, and epilepsy. We highlight sleep as a particularly vulnerable period for individuals with epilepsy and press that this topic warrants further investigation in order to develop therapeutic interventions to mitigate the risk of SUDEP.
Keywords: SUDEP; breathing; circadian; epilepsy; sleep.
Copyright © 2022 Joyal, Kreitlow and Buchanan.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
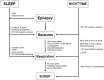
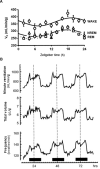
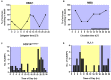
Figures
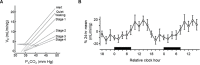
Similar articles
-
The role of monoaminergic neurons in modulating respiration during sleep and the connection with SUDEP.Biomed Pharmacother. 2022 Jun;150:112983. doi: 10.1016/j.biopha.2022.112983. Epub 2022 Apr 19. Biomed Pharmacother. 2022. PMID: 35453009 Review.
-
Time-of-day influences on respiratory sequelae following maximal electroshock-induced seizures in mice.J Neurophysiol. 2017 Nov 1;118(5):2592-2600. doi: 10.1152/jn.00039.2017. Epub 2017 Aug 9. J Neurophysiol. 2017. PMID: 28794189 Free PMC article.
-
Sudden unexpected death in epilepsy: people with nocturnal seizures may be at highest risk.Epilepsia. 2012 Feb;53(2):253-7. doi: 10.1111/j.1528-1167.2011.03360.x. Epub 2011 Dec 22. Epilepsia. 2012. PMID: 22192074
-
Sudden unexpected death in epilepsy (SUDEP) and sleep.Sleep Med Rev. 2011 Aug;15(4):237-46. doi: 10.1016/j.smrv.2010.07.006. Epub 2010 Oct 15. Sleep Med Rev. 2011. PMID: 20951616 Review.
-
The effect of time-of-day and circadian phase on vulnerability to seizure-induced death in two mouse models.J Physiol. 2021 Mar;599(6):1885-1899. doi: 10.1113/JP280856. Epub 2021 Feb 18. J Physiol. 2021. PMID: 33501667 Free PMC article.
Cited by
-
MK-212 precipitates seizure-induced death in amygdala-kindled mice via a non-5-HT2C receptor-mediated mechanism.Epilepsy Behav. 2025 Jun;167:110385. doi: 10.1016/j.yebeh.2025.110385. Epub 2025 Mar 24. Epilepsy Behav. 2025. PMID: 40132446
-
Seizure-related death exhibits a circadian rhythm independent of seizure timing or sleep in a mouse model of Dravet syndrome.J Physiol. 2025 Jun;603(12):3571-3587. doi: 10.1113/JP288697. Epub 2025 Jun 2. J Physiol. 2025. PMID: 40455956 Free PMC article.
-
Peri-ictal activation of dorsomedial dorsal raphe serotonin neurons reduces mortality associated with maximal electroshock seizures.Brain Commun. 2024 Mar 14;6(2):fcae052. doi: 10.1093/braincomms/fcae052. eCollection 2024. Brain Commun. 2024. PMID: 38487550 Free PMC article.
-
Selective Serotonin Reuptake Inhibitors and 5-HT2 Receptor Agonists Have Distinct, Sleep-state Dependent Effects on Postictal Breathing in Amygdala Kindled Mice.Neuroscience. 2023 Mar 1;513:76-95. doi: 10.1016/j.neuroscience.2023.01.016. Epub 2023 Jan 23. Neuroscience. 2023. PMID: 36702372 Free PMC article.
-
Sudden unexpected death in epilepsy.Curr Opin Neurol. 2022 Apr 1;35(2):181-188. doi: 10.1097/WCO.0000000000001034. Curr Opin Neurol. 2022. PMID: 35102124 Free PMC article. Review.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

