Prevalence and associated factors of metabolic body size phenotype in children and adolescents: A national cross-sectional analysis in China
- PMID: 36093090
- PMCID: PMC9452664
- DOI: 10.3389/fendo.2022.952825
Prevalence and associated factors of metabolic body size phenotype in children and adolescents: A national cross-sectional analysis in China
Abstract
Background: Metabolically healthy obesity (MHO) is a group of subjects with overweight/obesity who present a metabolically healthy profile; however, associated factors are complex and are far from completely understood. The aim of the current study was to estimate the prevalence of different metabolic body size phenotypes and investigate the associated factors in Chinese children and adolescents.
Methods: A cross-sectional survey was conducted of 12,346 children and adolescents aged 7-18 years from seven provinces in China in 2013. Anthropometric, blood pressure, and biochemical measurements were obtained. A multi-component questionnaire covering demographic, neonatal, and lifestyle characteristics was administered. The classification of metabolic body size phenotype based on three definitions was compared. With metabolically healthy with normal weight (MHNW) as a reference group, logistic regression analyses were used to estimate the potential effects of associated risk factors, with adjustment for age, sex, single-child status, and residence area.
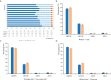
Results: The prevalence of MHNW, MHO, metabolically unhealthy with normal weight (MUNW), and metabolically unhealthy overweight/obesity (MUO) phenotype was 68.6%, 2.0%, 26.4%, and 3.0%, respectively. There were 39.3% MHO and 60.7% MUO among obese participants and 72.2% MHNW and 27.8% MUNW among those with normal weight. Compared to cardiometabolic risk factor (CMRF) criteria and metabolic syndrome (MetS) component definition, the application of the 2018 consensus-based definition may identify more children with abnormal cardiovascular risks, independent of weight status. Compared to younger children, older-aged adolescents were positively associated with higher risks of MUNW (odds ratio (OR) = 1.38, 95% CI = 1.27-1.50) and MUO (OR = 1.29, 95% CI = 1.04-1.60), while factors positively associated with MHO were younger age, single-child status, urban residence, high birth weight, prolonged breastfeeding duration, parental overweight/obesity status, long screen time, and less physical activity.
Conclusion: There were still a high proportion of children and adolescents at high cardiometabolic risk in China. Our findings reinforce the need for cardiometabolic risk prevention in children and adolescents irrespective of their weight statuses, such as parental educational programs and healthy lifestyle interventions.
Keywords: associated factors; children and adolescents; metabolic health; obesity; prevalence.
Copyright © 2022 Liu, Ma, Chen, Ma, Li, Gao, Ma, Wang, Chen, Zhang, Dong, Song and Ma.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Organization WH . World health statistics 2020: monitoring health for the SDGs, sustainable development goals. Geneva (Switzerland: World Health Organization; (2020).
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources