Analysis of post COVID-19 condition and its overlap with myalgic encephalomyelitis/chronic fatigue syndrome
- PMID: 36100326
- PMCID: PMC8619886
- DOI: 10.1016/j.jare.2021.11.013
Analysis of post COVID-19 condition and its overlap with myalgic encephalomyelitis/chronic fatigue syndrome
Abstract
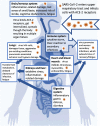
Background: The severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) disease (COVID-19) triggers the development of numerous pathologies and infection-linked complications and exacerbates existing pathologies in nearly all body systems. Aside from the primarily targeted respiratory organs, adverse SARS-CoV-2 effects were observed in nervous, cardiovascular, gastrointestinal/metabolic, immune, and other systems in COVID-19 survivors. Long-term effects of this viral infection have been recently observed and represent distressing sequelae recognised by the World Health Organisation (WHO) as a distinct clinical entity defined as post-COVID-19 condition. Considering the pandemic is still ongoing, more time is required to confirm post COVID-19 condition diagnosis in the COVID-19 infected cohorts, although many reported post COVID-19 symptoms overlap with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
Aims of review: In this study, COVID-19 clinical presentation and associated post-infection sequelae (post-COVID-19 condition) were reviewed and compared with ME/CFS symptomatology.
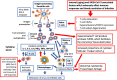
Key scientific concepts of review: The onset, progression, and symptom profile of post COVID-19 condition patients have considerable overlap with ME/CFS. Considering the large scope and range of pro-inflammatory effects of this virus, it is reasonable to expect development of post COVID-19 clinical complications in a proportion of the affected population. There are reports of a later debilitating syndrome onset three months post COVID-19 infection (often described as long-COVID-19), marked by the presence of fatigue, headache, cognitive dysfunction, post-exertional malaise, orthostatic intolerance, and dyspnoea. Acute inflammation, oxidative stress, and increased levels of interleukin-6 (IL-6) and tumor necrosis factor α (TNFα), have been reported in SARS-CoV-2 infected patients. Longitudinal monitoring of post COVID-19 patients is warranted to understand the long-term effects of SARS-CoV-2 infection and the pathomechanism of post COVID-19 condition.
Keywords: Chronic fatigue syndrome; Coronavirus; Fatigue; Myalgic encephalomyelitis; Post COVID-19 condition; Post-infection; SARS-CoV-2; Sequelae.
Copyright © 2022. Production and hosting by Elsevier B.V.
Conflict of interest statement
Declaration of Competing Interest The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures

References
-
- Organization WH. WHO Coronavirus (COVID-19) Dashboard. https://covid19.who.int/; 2021 (accessed 05/08/2021.).
-
- Zhang L., Han C., Zhang S., Duan C., Shang H., Bai T., et al. Diarrhea and altered inflammatory cytokine pattern in severe coronavirus disease 2019: impact on disease course and in-hospital mortality. J Gastroenterol Hepatol. 2021;36(2):421–429. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

