Prevalence of microcephaly and Zika virus infection in a pregnancy cohort in Kenya, 2017-2019
- PMID: 36100910
- PMCID: PMC9470235
- DOI: 10.1186/s12916-022-02498-8
Prevalence of microcephaly and Zika virus infection in a pregnancy cohort in Kenya, 2017-2019
Abstract
Background: Zika virus (ZIKV), first discovered in Uganda in 1947, re-emerged globally in 2013 and was later associated with microcephaly and other birth defects. We determined the incidence of ZIKV infection and its association with adverse pregnancy and fetal outcomes in a pregnancy cohort in Kenya.
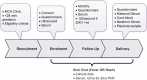
Methods: From October 2017 to July 2019, we recruited and followed up women aged ≥ 15 years and ≤ 28 weeks pregnant in three hospitals in coastal Mombasa. Monthly follow-up included risk factor questions and a blood sample collected for ZIKV serology. We collected anthropometric measures (including head circumference), cord blood, venous blood from newborns, and any evidence of birth defects. Microcephaly was defined as a head circumference (HC) < 2 standard deviations (SD) for sex and gestational age. Severe microcephaly was defined as HC < 3 SD for sex and age. We tested sera for anti-ZIKV IgM antibodies using capture enzyme-linked immunosorbent assay (ELISA) and confirmed positives using the plaque reduction neutralization test (PRNT90) for ZIKV and for dengue (DENV) on the samples that were ZIKV neutralizing antibody positive. We collected blood and urine from participants reporting fever or rash for ZIKV testing.
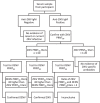
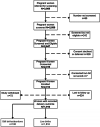
Results: Of 2889 pregnant women screened for eligibility, 2312 (80%) were enrolled. Of 1916 recorded deliveries, 1816 (94.6%) were live births and 100 (5.2%) were either stillbirths or spontaneous abortions (< 22 weeks of gestation). Among 1236 newborns with complete anthropometric measures, 11 (0.9%) had microcephaly and 3 (0.2%) had severe microcephaly. A total of 166 (7.2%) participants were positive for anti-ZIKV IgM, 136 of whom became seropositive during follow-up. Among the 166 anti-ZIKV IgM positive, 3 and 18 participants were further seropositive for ZIKV and DENV neutralizing antibodies, respectively. Of these 3 and 18 pregnant women, one and 13 (72.2%) seroconverted with antibodies to ZIKV and DENV, respectively. All 308 samples (serum and urine samples collected during sick visits and samples that were anti-ZIKV IgM positive) tested by RT-PCR were negative for ZIKV. No adverse pregnancy or neonatal outcomes were reported among the three participants with confirmed ZIKV exposure. Among newborns from pregnant women with DENV exposure, four (22.2%) were small for gestational age and one (5.6%) had microcephaly.
Conclusions: The prevalence of severe microcephaly among newborns in coastal Kenya was high relative to published estimates from facility-based studies in Europe and Latin America, but little evidence of ZIKV transmission. There is a need for improved surveillance for microcephaly and other congenital malformations in Kenya.
Keywords: Kenya; Microcephaly; Pregnancy; Zika virus.
© 2022. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

