Insertion site of central venous catheter among hospitalized adult patients: A systematic review and network meta-analysis
- PMID: 36106316
- PMCID: PMC9464814
- DOI: 10.3389/fmed.2022.960135
Insertion site of central venous catheter among hospitalized adult patients: A systematic review and network meta-analysis
Abstract
Introduction: Central venous catheterization is a commonly performed procedure, accounting for approximately 8% of hospitalized patients. Based on the current literatures, the most acceptable site for central venous catheterization is inconclusive, considering various complications in hospitalized patients. Herein, we conducted a network meta-analysis to assess the clinically important complications among internal jugular, subclavian, femoral, and peripheral insertion.
Materials and methods: The Cochrane Central Register of Controlled Trials, MEDLINE, Web of Science, Ichushi databases, Clinicaltrials.gov, and International Clinical Trials Registry Platform were searched. Studies including adults aged ≥ 18 years and randomized control trials that compared two different insertion sites (internal jugular, subclavian, femoral, and peripheral vein) were selected. The primary outcomes were clinically important infectious, thrombotic, and mechanical complications.
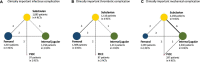
Results: Among the 5,819 records initially identified, 13 trials (6,201 patients) were included for a network meta-analysis. For clinically important infectious complication, subclavian insertion decreased the complication risk, compared with internal jugular [risk ratio (RR), 0.30; 95% confidence interval (CI), 0.11-0.81; moderate certainty], and femoral insertion increased than subclavian insertion (RR 2.56; 95% CI, 1.02-6.44; moderate certainty). Peripheral insertion was also significantly associated with a lower risk compared with internal jugular (RR 0.06; 95% CI, 0.01-0.32; low certainty); subclavian (RR 0.21; 95% CI, 0.05-0.77; moderate certainty); and femoral insertion (RR 0.08; 95% CI, 0.02-0.40; low certainty). For clinically important thrombotic complication, we did not find significant differences between insertion sites. For clinically important mechanical complication, femoral insertion decreased the complication risk, compared with internal jugular (RR 0.42; 95% CI, 0.21-0.82; moderate certainty) and subclavian insertion (RR 0.33; 95% CI, 0.16-0.66; moderate certainty). Peripheral insertion was also associated with the lower complication risk compared with internal jugular (RR 0.39; 95% CI, 0.18-0.85; low certainty) and subclavian insertion (RR 0.31; 95% CI, 0.13-0.75; moderate certainty).
Conclusion: The insertion site of the central venous catheter, which is most likely to cause the fewest complications, should be selected. Our findings can provide the rationale for deciding the insertion site for a central venous catheter.
Systematic review registration: [www.protocols.io], identifier [61375].
Keywords: central venous catheter; complication; hospitalization; insertion site; network meta-analysis.
Copyright © 2022 Sakuraya, Okano, Yoshihiro, Niida and Kimura.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures



Similar articles
-
Meta-analysis of subclavian insertion and nontunneled central venous catheter-associated infection risk reduction in critically ill adults.Crit Care Med. 2012 May;40(5):1627-34. doi: 10.1097/CCM.0b013e31823e99cb. Crit Care Med. 2012. PMID: 22511140
-
The incidence of infectious complications of central venous catheters at the subclavian, internal jugular, and femoral sites in an intensive care unit population.Crit Care Med. 2005 Jan;33(1):13-20; discussion 234-5. doi: 10.1097/01.ccm.0000149838.47048.60. Crit Care Med. 2005. PMID: 15644643
-
Totally implantable venous access ports: A systematic review and meta-analysis comparing subclavian and internal jugular vein punctures.Phlebology. 2022 May;37(4):279-288. doi: 10.1177/02683555211069772. Epub 2022 Feb 24. Phlebology. 2022. PMID: 35200052
-
Catheter type, placement and insertion techniques for preventing catheter-related infections in chronic peritoneal dialysis patients.Cochrane Database Syst Rev. 2019 May 31;5(5):CD004680. doi: 10.1002/14651858.CD004680.pub3. Cochrane Database Syst Rev. 2019. PMID: 31149735 Free PMC article.
-
Complications of femoral and subclavian venous catheterization in critically ill patients: a randomized controlled trial.JAMA. 2001 Aug 8;286(6):700-7. doi: 10.1001/jama.286.6.700. JAMA. 2001. PMID: 11495620 Clinical Trial.
Cited by
-
A Comparison of Techniques of Internal Jugular Vein Cannulation: Anatomical Landmark, Ultrasound Guided Pre-location, and Real-Time Ultrasound Guided.Cureus. 2024 Feb 19;16(2):e54499. doi: 10.7759/cureus.54499. eCollection 2024 Feb. Cureus. 2024. PMID: 38516452 Free PMC article.
-
Risk Assessment and Prevention of Venous Thromboembolism in Critically Ill Patients in Tibet: A Prospective Cohort Study with Historical Controls.Risk Manag Healthc Policy. 2025 Apr 3;18:1171-1179. doi: 10.2147/RMHP.S490160. eCollection 2025. Risk Manag Healthc Policy. 2025. PMID: 40196226 Free PMC article.
-
Cubital vein access provides a practical alternative to internal jugular vein access for coronary sinus catheter placement.J Arrhythm. 2024 Jul 7;40(4):991-997. doi: 10.1002/joa3.13110. eCollection 2024 Aug. J Arrhythm. 2024. PMID: 39139888 Free PMC article.
-
Efficacy and safety of supraclavicular versus infraclavicular approach for subclavian vein catheterisation: An updated systematic review and meta-analysis of randomised controlled trials.Indian J Anaesth. 2023 Jun;67(6):486-496. doi: 10.4103/ija.ija_837_22. Epub 2023 Jun 14. Indian J Anaesth. 2023. PMID: 37476443 Free PMC article.
-
How to improve the efficiency and the safety of real-time ultrasound-guided central venous catheterization in 2023: a narrative review.Ann Intensive Care. 2023 May 25;13(1):46. doi: 10.1186/s13613-023-01141-w. Ann Intensive Care. 2023. PMID: 37227571 Free PMC article. Review.
References
-
- Utsu Y, Masuda S, Watanabe R, Arai H, Nakamura A, Matsui S, et al. Changes in central venous catheter use in the hematology unit with the introduction of ultrasound guidance and a peripherally inserted central venous catheter. Intern Med. (2021) 60:2765–70. 10.2169/internalmedicine.7119-21 - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

