Post-laparotomy Hypoxia: A Case Series
- PMID: 36127966
- PMCID: PMC9479121
- DOI: 10.7759/cureus.28096
Post-laparotomy Hypoxia: A Case Series
Abstract
Postoperative hypoxia is a challenge for surgeons. With the advent of better anesthesia and minimal access surgical techniques, the incidence of postoperative hypoxia in elective cases has decreased. However, the incidence in life-saving emergency procedures still poses a possible threat, and cases seem under-reported. We report a series of five cases of postoperative hypoxia after laparotomy. These cases comprise mesenteric laceration, proximal jejunal perforation, perforated duodenal ulcer, abdominal tuberculosis, and fall from height. Despite different etiologies, they landed up with the complication of postoperative hypoxia, which was attributable to the type of procedure they underwent and not the indication of the procedure itself. Thus, they form an interesting collection of post-laparotomy hypoxia cases. We present them with a compilation of probable causes of postoperative hypoxia in such cases. Postoperative hypoxia presents a diagnostic challenge and requires timely suspicion, prompt intervention to eliminate the cause, and good postoperative care. The major causes include incomplete lung re-expansion, pain-induced restriction in chest-wall/diaphragm mobility, prolonged surgery, a complication of pre-existing lung disease, residual effects of some drugs, and iatrogenic causes. We, therefore, recommend the use of postoperative oxygen support and diligent monitoring of vitals in all cases of laparotomy, allowing prompt and timely patient management. Future studies are warranted to explore the prevalence and possible causes of post-laparotomy hypoxia.
Keywords: abdominal surgery; explorative laparotomy; post operative hypoxia; post-laparatomy hypoxia; postoperative care; postoperative hypoxia.
Copyright © 2022, Sharma et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
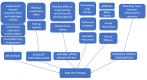
Figures
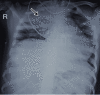
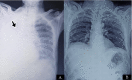


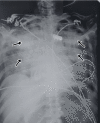
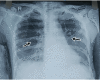
Similar articles
-
Experience with acute perforated duodenal ulcer in a West African population.Niger J Med. 2008 Oct-Dec;17(4):403-6. doi: 10.4314/njm.v17i4.37421. Niger J Med. 2008. PMID: 19048755
-
Successful use of the "patch, drain, and wait" laparotomy approach to perforated necrotizing enterocolitis: is hypoxia-triggered "good angiogenesis" involved?Pediatr Surg Int. 2000;16(5-6):356-63. doi: 10.1007/s003839900337. Pediatr Surg Int. 2000. PMID: 10955562
-
Jejunal perforation in gallstone ileus - a case series.J Med Case Rep. 2007 Nov 28;1:157. doi: 10.1186/1752-1947-1-157. J Med Case Rep. 2007. PMID: 18045463 Free PMC article.
-
Perforated peptic ulcer - an update.World J Gastrointest Surg. 2017 Jan 27;9(1):1-12. doi: 10.4240/wjgs.v9.i1.1. World J Gastrointest Surg. 2017. PMID: 28138363 Free PMC article. Review.
-
Pneumoperitoneum: a review of nonsurgical causes.Crit Care Med. 2000 Jul;28(7):2638-44. doi: 10.1097/00003246-200007000-00078. Crit Care Med. 2000. PMID: 10921609 Review.
References
-
- Postoperative pulmonary complications. Canet J, Mazo V. https://pubmed.ncbi.nlm.nih.gov/20150855/ Minerva Anestesiol. 2010;76:138–143. - PubMed
-
- Postoperative pulmonary complications and associated factors among surgical patients. Denu ZA, Yasin MO, Melekie TB, Berhe A. https://www.longdom.org/open-access/postoperative-pulmonary-complication... J Anesth Clin Res. 2015;6:554.
Publication types
LinkOut - more resources
Full Text Sources
