Factors Predicting 150 and 200 Microgram Adenosine Requirement during Four Increasing Doses of Intracoronary Adenosine Bolus Fractional Flow Reserve Assessment
- PMID: 36140478
- PMCID: PMC9498048
- DOI: 10.3390/diagnostics12092076
Factors Predicting 150 and 200 Microgram Adenosine Requirement during Four Increasing Doses of Intracoronary Adenosine Bolus Fractional Flow Reserve Assessment
Abstract
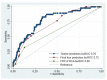
Direct intracoronary adenosine bolus is an excellent alternative to intravenous adenosine fractional flow reserve (FFR) measurement. This study, during four increasing adenosine boluses (50, 100, 150, and 200 mcg), aimed to explore clinical and angiographic predictors of coronary stenotic lesions for which the significant ischemic FFR (FFR ≤ 0.8) occurred at 150 and 200 mcg adenosine doses. Data from 1055 coronary lesions that underwent FFR measurement at the Central Chest Institute of Thailand from August 2011 to July 2021 were included. Baseline clinical and angiographic characteristics were analyzed. The FFR ≤ 0.8 occurred at adenosine 150 and 200 mcg boluses in 47 coronary lesions, while the FFR ≤ 0.8 occurred at adenosine 50 and 100 mcg boluses in 186 coronary lesions. After univariable and multivariable logistic regression analyses, four characteristics, including male sex, younger age, non-smoking status, and FFR procedure of RCA, were predictors of the occurrence of FFR ≤ 0.8 at adenosine 150 and 200 mcg doses. Combining all four predictors as a predictive model resulted in an AuROC of 0.72 (95% CI: 0.68-0.76), an 86% negative predictive value. Comparing these four predictors, the FFR procedure of RCA gave the most predictive power, with the AuROC of 0.60 (95% CI: 0.56-0.63).
Keywords: fractional flow reserve; intracoronary adenosine; percutaneous coronary intervention.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



References
-
- Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) The European Association for Cardio-Thoracic Surgery (EACTS) European Association for Percutaneous Cardiovascular Interventions (EAPCI) Kolh P., Wijns W., Danchin N., Di Mario C., Falk V., Folliguet T., Garg S., et al. Guidelines on myocardial revascularization. Eur. J. Cardio-Thoracic Surg. 2010;38:S1–S52. doi: 10.1016/j.ejcts.2010.08.019. - DOI - PubMed
-
- Levine G.N., Bates E.R., Blankenship J.C., Bailey S.R., Bittl J.A., Cercek B., Chambers C.E., Ellis S.G., Guyton R.A., Hollenberg S.M., et al. 2011 ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention: A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. J. Am. Coll. Cardiol. 2011;58:e44–e122. doi: 10.1016/j.jacc.2011.08.007. - DOI - PubMed
-
- Lotfi A., Jeremias A., Fearon W.F., Feldman M.D., Mehran R., Messenger J.C., Grines C.L., Dean L.S., Kern M.J., Klein L.W. Expert consensus statement on the use of fractional flow reserve, intravascular ultrasound, and optical coherence tomography. Catheter. Cardiovasc. Interv. 2014;83:509–518. doi: 10.1002/ccd.25222. - DOI - PubMed
LinkOut - more resources
Full Text Sources

