A retrospective study about incidental appendectomy during the laparoscopic treatment of intussusception
- PMID: 36147812
- PMCID: PMC9485678
- DOI: 10.3389/fped.2022.966839
A retrospective study about incidental appendectomy during the laparoscopic treatment of intussusception
Abstract
Purpose: We aim to see incidental appendectomy (IA) was worth or not during the laparoscopic treatment of intussusception.
Methods: This study included forty-eight patients who underwent a laparoscopic procedure for idiopathic intussusception without intestinal resection between April 2014 and April 2021. The Chi-square or Fisher's exact tests for categorical variables and the Student t-test for continuous variables were used to analyze and compare patient characteristics.
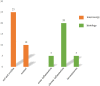
Results: IA was performed on 63% (30/48) of patients after surgical reduction, while 18 (37%), did not. Patients who underwent IA had a higher total cost (16,618 ± 2,174 vs.14,301 ± 5,206, P = 0.036), and a longer mean operation duration (59 ± 19 vs.45 ± 21, P = 0.025). The distribution of the PO time, length of hospital stay, PCs, and RI did not differ significantly. The histopathological evaluation of the 30 resected appendices revealed five (17%) with signs of acute inflammation, 20 (66%) with chronic signs of inflammation, and five (17%) with inconspicuous appendices.
Conclusion: IA is linked to a longer average operation time and a higher total cost. There is insufficient evidence to recommend IA during laparoscopic intussusception treatment. The risks and benefits of IA need further study.
Keywords: child; incidental appendectomy; intussusception; laparoscopy; surgery.
Copyright © 2022 Liu, Wu, Xu, Liu, Sheng and Lv.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Incidental appendectomy during robotic laparoscopic prostatectomy-safe and worth to perform?Langenbecks Arch Surg. 2018 Mar;403(2):265-269. doi: 10.1007/s00423-017-1630-5. Epub 2017 Nov 2. Langenbecks Arch Surg. 2018. PMID: 29098385
-
Outcomes and cost analysis of laparoscopic versus open appendectomy for treatment of acute appendicitis: 4-years experience in a district hospital.BMC Surg. 2014 Mar 19;14:14. doi: 10.1186/1471-2482-14-14. BMC Surg. 2014. PMID: 24646120 Free PMC article.
-
Operative treatment for intussusception: Should an incidental appendectomy be performed?J Pediatr Surg. 2019 Mar;54(3):495-499. doi: 10.1016/j.jpedsurg.2018.10.099. Epub 2018 Nov 26. J Pediatr Surg. 2019. PMID: 30583859
-
[Laparoscopic or open appendectomy. Critical review of the literature and personal experience].G Chir. 2001 Oct;22(10):353-7. G Chir. 2001. PMID: 11816948 Review. Italian.
-
Laparoscopic versus open reduction of intussusception in children: a retrospective review and meta-analysis.J Laparoendosc Adv Surg Tech A. 2014 Jul;24(7):518-22. doi: 10.1089/lap.2013.0415. J Laparoendosc Adv Surg Tech A. 2014. PMID: 24987845 Review.
Cited by
-
Retrospective cohort study of minimally invasive surgical approaches for pediatric intussusception.Sci Rep. 2024 Nov 30;14(1):29763. doi: 10.1038/s41598-024-81654-x. Sci Rep. 2024. PMID: 39613906 Free PMC article.
-
Benign or by Chance: A Case Report on Incidental Appendectomy Revealing a Neuroendocrine Tumor During Traumatic Exploratory Laparotomy.Cureus. 2024 Feb 20;16(2):e54527. doi: 10.7759/cureus.54527. eCollection 2024 Feb. Cureus. 2024. PMID: 38516428 Free PMC article.
References
-
- Coran AG, Adzick NS, Krummel TM, Laberge JM, Shamberger RC, Caldamone AA. Pediatric Surgery. 7th ed. (Philadelphia, PA: ) (2012). p. 441.
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous