Peripheral artery disease, abnormal ankle-brachial index, and prognosis in patients with acute coronary syndrome
- PMID: 36148064
- PMCID: PMC9485724
- DOI: 10.3389/fcvm.2022.902615
Peripheral artery disease, abnormal ankle-brachial index, and prognosis in patients with acute coronary syndrome
Abstract
Objectives: Ankle-brachial index (ABI) is an independent prognostic marker of cardiovascular events among patients with coronary artery disease (CAD). We aimed to investigate the outcome of patients hospitalized with acute coronary syndrome (ACS) and abnormal ABI.
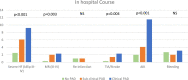
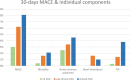
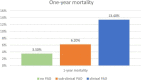
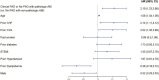
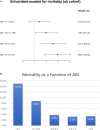
Approach and results: ABI was prospectively measured in 1,047 patients hospitalized due to ACS, who were stratified into three groups, namely, those with clinical peripheral artery disease (PAD) (N = 132), those without clinical PAD but with abnormal (< 0.9) ABI (subclinical PAD; N = 148), and those without clinical PAD with normal ABI (no PAD; N = 767). Patients were prospectively followed for 30-day major adverse cardiovascular event (MACE) and 1-year all-cause mortality. The mean age was 64 years. There was a significant gradual increase throughout the three groups in age, i.e., the incidence of prior stroke, diabetes mellitus, and hypertension (p for trend = 0.001 for all). The in-hospital course showed a gradual rise in the incidence of complications with an increase in heart failure [2.5, 6.1, and 9.2%, (p for trend = 0.001)] and acute kidney injury [2, 4.1, and 11.5%, (p for trend = 0.001)]. At day 30, there was a stepwise increase in MACE, such that patients without PAD had the lowest rate, followed by subclinical and clinical PADs (3.5, 6.8, and 8.1%, respectively, p for trend = 0.009). Similarly, there was a significant increase in 1-year mortality from 3.4% in patients without PAD, through 6.8% in those with subclinical PAD, to 15.2% in those with clinical PAD (p for trend = 0.001).
Conclusion: Subclinical PAD is associated with poor outcomes in patients with ACS, suggesting that routine ABI screening could carry important prognostic significance in these patients regardless of PAD symptoms.
Keywords: acute coronary syndrome; ankle brachial blood pressure index; claudication; peripheral arterial disease (PAD); peripheral vascular disease; vascular disease (PVD).
Copyright © 2022 Berkovitch, Iakobishvili, Fuchs, Atar, Braver, Eisen, Glikson, Beigel and Matetzky.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Subclinical peripheral arterial disease and incompressible ankle arteries are both long-term prognostic factors in patients undergoing coronary artery bypass grafting.J Am Coll Cardiol. 2005 Sep 6;46(5):815-20. doi: 10.1016/j.jacc.2005.05.066. J Am Coll Cardiol. 2005. PMID: 16139130
-
Combination of ankle brachial index and diabetes mellitus to predict cardiovascular events and mortality after an acute coronary syndrome.Int J Cardiol. 2011 Aug 18;151(1):84-8. doi: 10.1016/j.ijcard.2010.04.097. Epub 2010 May 21. Int J Cardiol. 2011. PMID: 20488566
-
Lower extremity peripheral arterial disease in hospitalized patients with coronary artery disease.Vasc Med. 2003 Nov;8(4):233-6. doi: 10.1191/1358863x03vm506ra. Vasc Med. 2003. PMID: 15125482
-
The role of ankle-brachial index for predicting peripheral arterial disease.Maedica (Bucur). 2014 Sep;9(3):295-302. Maedica (Bucur). 2014. PMID: 25705296 Free PMC article. Review.
-
Prognostic Value of Abnormal Ankle-Brachial Index in Patients With Coronary Artery Disease: A Meta-Analysis.Angiology. 2020 Jul;71(6):491-497. doi: 10.1177/0003319720911582. Epub 2020 Mar 13. Angiology. 2020. PMID: 32166959 Review.
Cited by
-
The Association between Percentage of Mean Arterial Pressure and Long-Term Mortality in Acute Myocardial Infarction Patients: An Observational Cohort Study.Int J Med Sci. 2024 Aug 12;21(11):2119-2126. doi: 10.7150/ijms.95430. eCollection 2024. Int J Med Sci. 2024. PMID: 39239551 Free PMC article.
-
An Evaluation of Plasma TNF, VEGF-A, and IL-6 Determination as a Risk Marker of Atherosclerotic Vascular Damage in Early-Onset CAD Patients.J Clin Med. 2024 Mar 18;13(6):1742. doi: 10.3390/jcm13061742. J Clin Med. 2024. PMID: 38541966 Free PMC article.
-
Evaluation of ankle brachial index, serum miR-103 and LP-PLA2 in the prognosis of acute ischemic stroke.Pak J Med Sci. 2024 Mar-Apr;40(4):763-766. doi: 10.12669/pjms.40.4.8716. Pak J Med Sci. 2024. PMID: 38545022 Free PMC article.
-
Prediction of All-Cause Mortality and Cardiovascular Outcomes Using Ambulatory Arterial Stiffness and Ankle-Brachial Indices in Patients with Acute Myocardial Infarction: A Prospective Cohort Study.J Clin Med. 2025 Jun 30;14(13):4627. doi: 10.3390/jcm14134627. J Clin Med. 2025. PMID: 40649001 Free PMC article.
-
Association Between hsTnT and NT-proBNP and Peripheral Artery Disease in People with HIV: A Multicentre Danish Cohort Study.Biomolecules. 2025 Mar 11;15(3):401. doi: 10.3390/biom15030401. Biomolecules. 2025. PMID: 40149937 Free PMC article.
References
-
- Morillas P, Quiles J, Cordero A, Guindo J, Soria F, Mazon P, et al. Prevalence of peripheral arterial disease in patients with acute coronary syndrome I. impact of clinical and subclinical peripheral arterial disease in mid-term prognosis of patients with acute coronary syndrome. Am J Cardiol. (2009) 104:1494–8. 10.1016/j.amjcard.2009.07.014 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

