Production and nonclinical evaluation of an autologous iPSC-derived platelet product for the iPLAT1 clinical trial
- PMID: 36149941
- PMCID: PMC9706535
- DOI: 10.1182/bloodadvances.2022008512
Production and nonclinical evaluation of an autologous iPSC-derived platelet product for the iPLAT1 clinical trial
Abstract
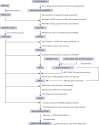
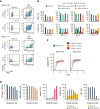
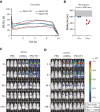
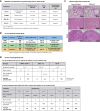
Donor-derived platelets are used to treat or prevent hemorrhage in patients with thrombocytopenia. However, ∼5% or more of these patients are complicated with alloimmune platelet transfusion refractoriness (allo-PTR) due to alloantibodies against HLA-I or human platelet antigens (HPA). In these cases, platelets from compatible donors are necessary, but it is difficult to find such donors for patients with rare HLA-I or HPA. To produce platelet products for patients with aplastic anemia with allo-PTR due to rare HPA-1 mismatch in Japan, we developed an ex vivo good manufacturing process (GMP)-based production system for an induced pluripotent stem cell-derived platelet product (iPSC-PLTs). Immortalized megakaryocyte progenitor cell lines (imMKCLs) were established from patient iPSCs, and a competent imMKCL clone was selected for the master cell bank (MCB) and confirmed for safety, including negativity of pathogens. From this MCB, iPSC-PLTs were produced using turbulent flow bioreactors and new drugs. In extensive nonclinical studies, iPSC-PLTs were confirmed for quality, safety, and efficacy, including hemostasis in a rabbit model. This report presents a complete system for the GMP-based production of iPSC-PLTs and the required nonclinical studies and thus supports the iPLAT1 study, the first-in-human clinical trial of iPSC-PLTs in a patient with allo-PTR and no compatible donor using the autologous product. It also serves as a comprehensive reference for the development of widely applicable allogeneic iPSC-PLTs and other cell products that use iPSC-derived progenitor cells as MCB.
© 2022 by The American Society of Hematology. Licensed under Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0), permitting only noncommercial, nonderivative use with attribution. All other rights reserved.
Conflict of interest statement
Conflict-of-interest disclosure: S.N. and K.E. have applied for patents related to this manuscript. N.S. serves as a consultant for Megakaryon Co. J.K. serves as a consultant for Astellas Pharma and an adviser for Daiichi Sankyo Co, Janssen Pharmaceutical, Megakaryon, SymBio Pharmaceuticals, and Takeda Pharmaceutical and receives research funding from Eisai Co. A. Shigemasa is employed at Megakaryon. A.T-K. serves as an adviser for Megakaryon and receives research funding from Ono Pharmaceutical. K.E. is a founder of Megakaryon and a member of its scientific advisory board without salary and receives research funding from Megakaryon, Otsuka Pharmaceutical, and Kyoto Manufacturing Co. The remaining authors declare no competing financial interests. All the interests were reviewed and are managed by Kyoto University in accordance with its conflict-of-interest policies.
Figures




Comment in
-
Engineered platelets for clinical application: a step closer.Blood. 2022 Dec 1;140(22):2314-2315. doi: 10.1182/blood.2022018291. Blood. 2022. PMID: 36454596 Free PMC article. No abstract available.
References
-
- Szczepiorkowski ZM, Dunbar NM. Transfusion guidelines: when to transfuse. Hematol Am Soc Hematol Educ Prog. 2013;2013:638–644. - PubMed
-
- Estcourt LJ, Birchall J, Allard S, et al. Guidelines for the use of platelet transfusions. Br J Haematol. 2017;176(3):365–394. - PubMed
-
- Stanworth SJ, Navarrete C, Estcourt L, Marsh J. Platelet refractoriness--practical approaches and ongoing dilemmas in patient management. Br J Haematol. 2015;171(3):297–305. - PubMed
-
- Takahashi K, Yamanaka S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell. 2006;126(4):663–676. - PubMed
-
- Takahashi K, Tanabe K, Ohnuki M, et al. Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell. 2007;131(5):861–872. - PubMed

