Impaired hemodynamic response to exercise in patients with peripheral artery disease: evidence of a link to inflammation and oxidative stress
- PMID: 36154490
- PMCID: PMC9602942
- DOI: 10.1152/ajpregu.00159.2022
Impaired hemodynamic response to exercise in patients with peripheral artery disease: evidence of a link to inflammation and oxidative stress
Abstract
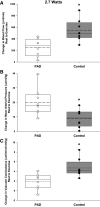
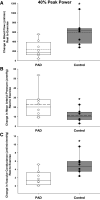
An exaggerated mean arterial blood pressure (MAP) response to exercise in patients with peripheral artery disease (PAD), likely driven by inflammation and oxidative stress and, perhaps, required to achieve an adequate blood flow response, is well described. However, the blood flow response to exercise in patients with PAD actually remains equivocal. Therefore, eight patients with PAD and eight healthy controls completed 3 min of plantar flexion exercise at both an absolute work rate (WR) (2.7 W, to evaluate blood flow) and a relative intensity (40%WRmax, to evaluate MAP). The exercise-induced change in popliteal artery blood flow (BF, Ultrasound Doppler), MAP (Finapress), and vascular conductance (VC) were quantified. In addition, resting markers of inflammation and oxidative stress were measured in plasma and muscle biopsies. Exercise-induced ΔBF, assessed at 2.7 W, was lower in PAD compared with controls (PAD: 251 ± 150 vs. Controls: 545 ± 187 mL/min, P < 0.001), whereas ΔMAP, assessed at 40%WRmax, was greater for PAD (PAD: 23 ± 14 vs. Controls: 11 ± 6 mmHg, P = 0.028). The exercise-induced ΔVC was lower for PAD during both the absolute WR (PAD: 1.9 ± 1.6 vs. Controls: 4.7 ± 1.9 mL/min/mmHg) and relative intensity exercise (PAD: 1.9 ± 1.8 vs. Controls: 5.0 ± 2.2 mL/min/mmHg) trials (both, P < 0.01). Inflammatory and oxidative stress markers, including plasma interleukin-6 and muscle protein carbonyls, were elevated in PAD (both, P < 0.05), and significantly correlated with the hemodynamic changes during exercise (r = -0.57 to -0.78, P < 0.05). Thus, despite an exaggerated ΔMAP response, patients with PAD exhibit an impaired exercise-induced ΔBF and ΔVC, and both inflammation and oxidative stress likely play a role in this attenuated hemodynamic response.
Keywords: blood flow; exercise pressor response; peripheral vascular disease.
Conflict of interest statement
No conflicts of interest, financial or otherwise, are declared by the authors.
Figures

Similar articles
-
Eight weeks of nitrate supplementation improves blood flow and reduces the exaggerated pressor response during forearm exercise in peripheral artery disease.Am J Physiol Heart Circ Physiol. 2018 Jul 1;315(1):H101-H108. doi: 10.1152/ajpheart.00015.2018. Epub 2018 Mar 9. Am J Physiol Heart Circ Physiol. 2018. PMID: 29522355 Free PMC article. Clinical Trial.
-
Systemic and regional hemodynamic response to activation of the exercise pressor reflex in patients with peripheral artery disease.Am J Physiol Heart Circ Physiol. 2020 Apr 1;318(4):H916-H924. doi: 10.1152/ajpheart.00493.2019. Epub 2020 Feb 28. Am J Physiol Heart Circ Physiol. 2020. PMID: 32108523 Free PMC article.
-
Blood pressure and calf muscle oxygen extraction during plantar flexion exercise in peripheral artery disease.J Appl Physiol (1985). 2017 Jul 1;123(1):2-10. doi: 10.1152/japplphysiol.01110.2016. Epub 2017 Apr 6. J Appl Physiol (1985). 2017. PMID: 28385920 Free PMC article.
-
Diagnostic methods for measurement of peripheral blood flow during exercise in patients with type 2 diabetes and peripheral artery disease: a systematic review.Int Angiol. 2019 Feb;38(1):62-69. doi: 10.23736/S0392-9590.18.04051-8. Int Angiol. 2019. PMID: 30860342
-
Skeletal Muscle Pathology in Peripheral Artery Disease: A Brief Review.Arterioscler Thromb Vasc Biol. 2020 Nov;40(11):2577-2585. doi: 10.1161/ATVBAHA.120.313831. Epub 2020 Sep 17. Arterioscler Thromb Vasc Biol. 2020. PMID: 32938218 Free PMC article. Review.
Cited by
-
Bradykinin 2 receptors contribute to the exaggerated exercise pressor reflex in a rat model of simulated peripheral artery disease.Am J Physiol Regul Integr Comp Physiol. 2023 Feb 1;324(2):R183-R195. doi: 10.1152/ajpregu.00274.2022. Epub 2022 Dec 19. Am J Physiol Regul Integr Comp Physiol. 2023. PMID: 36534589 Free PMC article.
-
Zhilong Huoxue Tongyu capsule inhibits hypertensive myocardial fibrosis via balancing TGF-β1/Smad3/Erbb4-IR/miR-29b pathway.Sci Rep. 2025 Jul 11;15(1):25127. doi: 10.1038/s41598-025-10631-9. Sci Rep. 2025. PMID: 40646094 Free PMC article.
-
Selected Plant-Derived Polyphenols as Potential Therapeutic Agents for Peripheral Artery Disease: Molecular Mechanisms, Efficacy and Safety.Molecules. 2022 Oct 21;27(20):7110. doi: 10.3390/molecules27207110. Molecules. 2022. PMID: 36296702 Free PMC article. Review.
References
-
- McDermott MM, Liu K, Greenland P, Guralnik JM, Criqui MH, Chan C, Pearce WH, Schneider JR, Ferrucci L, Celic L, Taylor LM, Vonesh E, Martin GJ, Clark E. Functional decline in peripheral arterial disease: associations with the ankle brachial index and leg symptoms. JAMA 292: 453–461, 2004. doi:10.1001/jama.292.4.453. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

