Clinical application of the "sellar barrier's concept" for predicting intraoperative CSF leak in endoscopic endonasal surgery for pituitary adenomas with a machine learning analysis
- PMID: 36157423
- PMCID: PMC9492953
- DOI: 10.3389/fsurg.2022.934721
Clinical application of the "sellar barrier's concept" for predicting intraoperative CSF leak in endoscopic endonasal surgery for pituitary adenomas with a machine learning analysis
Abstract
Background: Recently, it was defined that the sellar barrier entity could be identified as a predictor of cerebrospinal fluid (CSF) intraoperative leakage. The aim of this study is to validate the application of the sellar barrier concept for predicting intraoperative CSF leak in endoscopic endonasal surgery for pituitary adenomas with a machine learning approach.
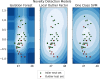
Methods: We conducted a prospective cohort study, from June 2019 to September 2020: data from 155 patients with pituitary subdiaphragmatic adenoma operated through endoscopic approach at the Division of Neurosurgery, Università degli Studi di Napoli "Federico II," were included. Preoperative magnetic resonance images (MRI) and intraoperative findings were analyzed. After processing patient data, the experiment was conducted as a novelty detection problem, splitting outliers (i.e., patients with intraoperative fistula, n = 11/155) and inliers into separate datasets, the latter further separated into training (n = 115/144) and inlier test (n = 29/144) datasets. The machine learning analysis was performed using different novelty detection algorithms [isolation forest, local outlier factor, one-class support vector machine (oSVM)], whose performance was assessed separately and as an ensemble on the inlier and outlier test sets.
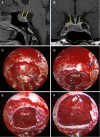
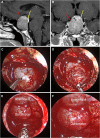
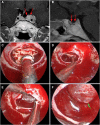
Results: According to the type of sellar barrier, patients were classified into two groups, i.e., strong and weak barrier; a third category of mixed barrier was defined when a case was neither weak nor strong. Significant differences between the three datasets were found for Knosp classification score (p = 0.0015), MRI barrier: strong (p = 1.405 × 10-6), MRI barrier: weak (p = 4.487 × 10-8), intraoperative barrier: strong (p = 2.788 × 10-7), and intraoperative barrier: weak (p = 2.191 × 10-10). We recorded 11 cases of intraoperative leakage that occurred in the majority of patients presenting a weak sellar barrier (p = 4.487 × 10-8) at preoperative MRI. Accuracy, sensitivity, and specificity for outlier detection were 0.70, 0.64, and 0.72 for IF; 0.85, 0.45, and 1.00 for LOF; 0.83, 0.64, and 0.90 for oSVM; and 0.83, 0.55, and 0.93 for the ensemble, respectively.
Conclusions: There is a true correlation between the type of sellar barrier at MRI and its in vivo features as observed during endoscopic endonasal surgery. The novelty detection models highlighted differences between patients who developed an intraoperative CSF leak and those who did not.
Keywords: CSF leak; machine learning; pituitary adenoma; sellar barrier; skull base surgery.
© 2022 Villalonga, Solari, Cuocolo, De Lucia, Ugga, Gragnaniello, Pailler, Cervio, Campero, Cavallo and Cappabianca.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
The sellar barrier on preoperative imaging predicts intraoperative cerebrospinal fluid leak: a prospective multicenter cohort study.Pituitary. 2021 Feb;24(1):27-37. doi: 10.1007/s11102-020-01082-8. Epub 2020 Sep 12. Pituitary. 2021. PMID: 32918661
-
Endoscopic anatomy of the sellar barrier: From the anatomical model to the operating room.Clin Anat. 2020 Apr;33(3):468-474. doi: 10.1002/ca.23566. Epub 2020 Jan 20. Clin Anat. 2020. PMID: 31943393
-
Identification and repair of intraoperative cerebrospinal fluid leaks in endonasal transsphenoidal pituitary surgery: surgical experience in a series of 1002 patients.J Neurosurg. 2018 Aug;129(2):425-429. doi: 10.3171/2017.4.JNS162451. Epub 2017 Sep 29. J Neurosurg. 2018. PMID: 28960156
-
Endoscopic Endonasal Management of Rare Sellar Lesions: Clinical and Surgical Experience of 78 Cases and Review of the Literature.World Neurosurg. 2017 Apr;100:369-380. doi: 10.1016/j.wneu.2016.11.057. Epub 2016 Nov 22. World Neurosurg. 2017. PMID: 27888088 Review.
-
Endonasal Endoscopic Surgery for Pediatric Sellar and Suprasellar Lesions: A Systematic Review and Meta-analysis.Otolaryngol Head Neck Surg. 2020 Aug;163(2):284-292. doi: 10.1177/0194599820913637. Epub 2020 Mar 24. Otolaryngol Head Neck Surg. 2020. PMID: 32204653
Cited by
-
Guanti bianchi technique for resection of selected pituitary adenomas.Brain Spine. 2023 Feb 25;3:101724. doi: 10.1016/j.bas.2023.101724. eCollection 2023. Brain Spine. 2023. PMID: 37383463 Free PMC article.
-
Development of an artificial intelligence-based convolutional neural network for sellar barrier classification using magnetic resonance imaging.Surg Neurol Int. 2025 May 9;16:174. doi: 10.25259/SNI_303_2025. eCollection 2025. Surg Neurol Int. 2025. PMID: 40469315 Free PMC article.
-
Artificial Intelligence, Radiomics, and Computational Modeling in Skull Base Surgery.Adv Exp Med Biol. 2024;1462:265-283. doi: 10.1007/978-3-031-64892-2_16. Adv Exp Med Biol. 2024. PMID: 39523271 Review.
-
Current status of artificial intelligence technologies in pituitary adenoma surgery: a scoping review.Pituitary. 2024 Apr;27(2):91-128. doi: 10.1007/s11102-023-01369-6. Epub 2024 Jan 6. Pituitary. 2024. PMID: 38183582
References
LinkOut - more resources
Full Text Sources
Miscellaneous

