Molecular, Pathological, Clinical, and Therapeutic Aspects of Perihematomal Edema in Different Stages of Intracerebral Hemorrhage
- PMID: 36164392
- PMCID: PMC9509250
- DOI: 10.1155/2022/3948921
Molecular, Pathological, Clinical, and Therapeutic Aspects of Perihematomal Edema in Different Stages of Intracerebral Hemorrhage
Abstract
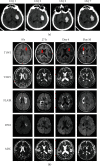
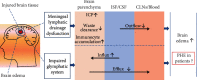
Acute intracerebral hemorrhage (ICH) is a devastating type of stroke worldwide. Neuronal destruction involved in the brain damage process caused by ICH includes a primary injury formed by the mass effect of the hematoma and a secondary injury induced by the degradation products of a blood clot. Additionally, factors in the coagulation cascade and complement activation process also contribute to secondary brain injury by promoting the disruption of the blood-brain barrier and neuronal cell degeneration by enhancing the inflammatory response, oxidative stress, etc. Although treatment options for direct damage are limited, various strategies have been proposed to treat secondary injury post-ICH. Perihematomal edema (PHE) is a potential surrogate marker for secondary injury and may contribute to poor outcomes after ICH. Therefore, it is essential to investigate the underlying pathological mechanism, evolution, and potential therapeutic strategies to treat PHE. Here, we review the pathophysiology and imaging characteristics of PHE at different stages after acute ICH. As illustrated in preclinical and clinical studies, we discussed the merits and limitations of varying PHE quantification protocols, including absolute PHE volume, relative PHE volume, and extension distance calculated with images and other techniques. Importantly, this review summarizes the factors that affect PHE by focusing on traditional variables, the cerebral venous drainage system, and the brain lymphatic drainage system. Finally, to facilitate translational research, we analyze why the relationship between PHE and the functional outcome of ICH is currently controversial. We also emphasize promising therapeutic approaches that modulate multiple targets to alleviate PHE and promote neurologic recovery after acute ICH.
Copyright © 2022 Chao Jiang et al.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- Campbell B. C. V., Khatri P. Stroke. The Lancet . 2020;396(10244):129–142. - PubMed
-
- Hua W., Chen X. M., Wang J. M., et al. Mechanisms and potential therapeutic targets for spontaneous intracerebral hemorrhage. Brain Hemorrhages . 2020;1(2):99–104.
-
- Shoamanesh A., Patrice Lindsay M., Castellucci L. A., et al. Canadian stroke best practice recommendations: management of spontaneous intracerebral hemorrhage, 7th edition update 2020. International journal of stroke . 2021;16(3):321–341. - PubMed
-
- Krishnamurthi R. V., Ikeda T., Feigin V. L. Global, regional and country-specific burden of ischaemic stroke, intracerebral haemorrhage and subarachnoid haemorrhage: a systematic analysis of the global burden of disease study 2017. Neuroepidemiology . 2020;54(2):171–179. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials

