Socioeconomic risk markers of congenital Zika syndrome: a nationwide, registry-based study in Brazil
- PMID: 36175039
- PMCID: PMC9528618
- DOI: 10.1136/bmjgh-2022-009600
Socioeconomic risk markers of congenital Zika syndrome: a nationwide, registry-based study in Brazil
Abstract
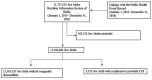
While it is well known that socioeconomic markers are associated with a higher risk of arbovirus infections, research on the relationship between socioeconomic factors and congenital Zika syndrome (CZS) remains limited. This study investigates the relationship between socioeconomic risk markers and live births with CZS in Brazil. We conducted a population-based study using data from all registered live births in Brazil (Live Births Information System) linked with the Public Health Event Record from 1 January 2015 to 31 December 2018. We used logistic regression models to estimate the OR and 95% CIs of CZS based on a three-level framework. In an analysis of 11 366 686 live births, of which 3353 had CZS, we observed that live births of self-identified black or mixed race/brown mothers (1.72 (95% CI 1.47 to 2.01) and 1.37 (95% CI 1.24 to 1.51)) were associated with a higher odds of CZS. Live births from single women compared with married women and those from women with less than 12 years of education compared with those with more than 12 years of education also had higher odds of CZS. In addition, live births following fewer prenatal care appointments had increased odds of CZS in the nationwide data. However, in the analyses conducted in the Northeast region (where the microcephaly epidemic started before the link with Zika virus was established and before preventive measures were known or disseminated), no statistical association was found between the number of prenatal care appointments and the odds of CZS. This study shows that live births of the most socially vulnerable women in Brazil had the greatest odds of CZS. This disproportionate distribution of risk places an even greater burden on already socioeconomically disadvantaged groups, and the lifelong disabilities caused by this syndrome may reinforce existing social and health inequalities.
Keywords: arboviruses; child health; epidemiology; public health.
© Author(s) (or their employer(s)) 2022. Re-use permitted under CC BY. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures

Similar articles
-
Disease burden of congenital Zika virus syndrome in Brazil and its association with socioeconomic data.Sci Rep. 2023 Jul 23;13(1):11882. doi: 10.1038/s41598-023-38553-4. Sci Rep. 2023. PMID: 37482558 Free PMC article.
-
Congenital Zika syndrome and living conditions in the largest city of northeastern Brazil.BMC Public Health. 2022 Jun 20;22(1):1231. doi: 10.1186/s12889-022-13614-x. BMC Public Health. 2022. PMID: 35725427 Free PMC article.
-
Use of infectious disease surveillance reports to monitor the Zika virus epidemic in Latin America and the Caribbean from 2015 to 2017: strengths and deficiencies.BMJ Open. 2020 Dec 12;10(12):e042869. doi: 10.1136/bmjopen-2020-042869. BMJ Open. 2020. PMID: 33310811 Free PMC article.
-
Prevalence of sleep disorders in children with Congenital Zika Syndrome.J Trop Pediatr. 2023 Oct 5;69(6):fmad033. doi: 10.1093/tropej/fmad033. J Trop Pediatr. 2023. PMID: 37794754
-
Serious Concern of Congenital Zika Syndrome (CZS) in India: A Narrative Review.J Pregnancy. 2024 Jun 13;2024:1758662. doi: 10.1155/2024/1758662. eCollection 2024. J Pregnancy. 2024. PMID: 38961858 Free PMC article. Review.
Cited by
-
Maternal and gestational factors associated with congenital anomalies among live births: a nationwide population-based study in Brazil from 2012 to 2020.BMC Pregnancy Childbirth. 2025 Jul 2;25(1):678. doi: 10.1186/s12884-025-07675-0. BMC Pregnancy Childbirth. 2025. PMID: 40604506 Free PMC article.
-
Democratizing Public Health: Participatory Policymaking Institutions, Mosquito Control, and Zika in the Americas.Trop Med Infect Dis. 2023 Jan 5;8(1):38. doi: 10.3390/tropicalmed8010038. Trop Med Infect Dis. 2023. PMID: 36668945 Free PMC article.
-
Prevalence and trends of major congenital anomalies in Brazil: A study from 2011 to 2020.PLoS One. 2025 Jun 6;20(6):e0323654. doi: 10.1371/journal.pone.0323654. eCollection 2025. PLoS One. 2025. PMID: 40478925 Free PMC article.
-
Social determinants impact both viral infections and brain development.Pediatr Res. 2025 Jul 25. doi: 10.1038/s41390-025-04292-7. Online ahead of print. Pediatr Res. 2025. PMID: 40715423 Review.
-
High-Risk Areas for Congenital Zika Syndrome in Rio de Janeiro: Spatial Cluster Detection.Trop Med Infect Dis. 2024 May 7;9(5):105. doi: 10.3390/tropicalmed9050105. Trop Med Infect Dis. 2024. PMID: 38787038 Free PMC article.
References
-
- PAHO/WHO . Regional Zika epidemiological update (Americas) August 25, 2017, 2017. Available: https://www.paho.org/hq/dmdocuments/2017/2017-aug-25-phe-epi-update-zika...
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
