The effect of high-polyphenol Mediterranean diet on visceral adiposity: the DIRECT PLUS randomized controlled trial
- PMID: 36175997
- PMCID: PMC9523931
- DOI: 10.1186/s12916-022-02525-8
The effect of high-polyphenol Mediterranean diet on visceral adiposity: the DIRECT PLUS randomized controlled trial
Abstract
Background: Mediterranean (MED) diet is a rich source of polyphenols, which benefit adiposity by several mechanisms. We explored the effect of the green-MED diet, twice fortified in dietary polyphenols and lower in red/processed meat, on visceral adipose tissue (VAT).
Methods: In the 18-month Dietary Intervention Randomized Controlled Trial PoLyphenols UnproceSsed (DIRECT-PLUS) weight-loss trial, 294 participants were randomized to (A) healthy dietary guidelines (HDG), (B) MED, or (C) green-MED diets, all combined with physical activity. Both isocaloric MED groups consumed 28 g/day of walnuts (+ 440 mg/day polyphenols). The green-MED group further consumed green tea (3-4 cups/day) and Wolffia globosa (duckweed strain) plant green shake (100 g frozen cubes/day) (+ 800mg/day polyphenols) and reduced red meat intake. We used magnetic resonance imaging (MRI) to quantify the abdominal adipose tissues.
Results: Participants (age = 51 years; 88% men; body mass index = 31.2 kg/m2; 29% VAT) had an 89.8% retention rate and 79.3% completed eligible MRIs. While both MED diets reached similar moderate weight (MED: - 2.7%, green-MED: - 3.9%) and waist circumference (MED: - 4.7%, green-MED: - 5.7%) loss, the green-MED dieters doubled the VAT loss (HDG: - 4.2%, MED: - 6.0%, green-MED: - 14.1%; p < 0.05, independent of age, sex, waist circumference, or weight loss). Higher dietary consumption of green tea, walnuts, and Wolffia globosa; lower red meat intake; higher total plasma polyphenols (mainly hippuric acid), and elevated urine urolithin A polyphenol were significantly related to greater VAT loss (p < 0.05, multivariate models).
Conclusions: A green-MED diet, enriched with plant-based polyphenols and lower in red/processed meat, may be a potent intervention to promote visceral adiposity regression.
Trial registration: ClinicalTrials.gov , NCT03020186.
Keywords: Mediterranean; Obesity; Plant-based diet; Polyphenols; Visceral adipose tissue.
© 2022. The Author(s).
Conflict of interest statement
Iris Shai advises the Hinoman, Ltd. nutritional committee. This work was supported by California Walnuts Commission. None of the funding providers was involved in any stage of the design, conduct, or analysis of the study, and they had no access to the study results before publication. All other authors declare that they have no competing interests.
Figures

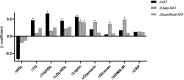

References
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical

