Suppression of bile acid synthesis as a tipping point in the disease course of primary sclerosing cholangitis
- PMID: 36176935
- PMCID: PMC9513776
- DOI: 10.1016/j.jhepr.2022.100561
Suppression of bile acid synthesis as a tipping point in the disease course of primary sclerosing cholangitis
Abstract
Background & aims: Farnesoid X receptor (FXR) agonists and fibroblast growth factor 19 (FGF19) analogues suppress bile acid synthesis and are being investigated for their potential therapeutic efficacy in cholestatic liver diseases. We investigated whether bile acid synthesis associated with outcomes in 2 independent populations of people with primary sclerosing cholangitis (PSC) not receiving such therapy.
Methods: Concentrations of individual bile acids and 7α-hydroxy-4-cholesten-3-one (C4) were measured in blood samples from 330 patients with PSC attending tertiary care hospitals in the discovery and validation cohorts and from 100 healthy donors. We used a predefined multivariable Cox proportional hazards model to evaluate the prognostic value of C4 to predict liver transplantation-free survival and evaluated its performance in the validation cohort.
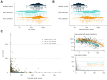
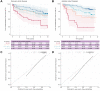
Results: The bile acid synthesis marker C4 was negatively associated with total bile acids. Patients with fully suppressed bile acid synthesis had strongly elevated total bile acids and short liver transplantation-free survival. In multivariable models, a 50% reduction in C4 corresponded to increased hazards for liver transplantation or death in both the discovery (adjusted hazard ratio [HR] = 1.24, 95% CI 1.06-1.43) and validation (adjusted HR = 1.23, 95% CI 1.03-1.47) cohorts. Adding C4 to established risk scores added value to predict future events, and predicted survival probabilities were well calibrated externally. There was no discernible impact of ursodeoxycholic acid treatment on bile acid synthesis.
Conclusions: Bile acid accumulation-associated suppression of bile acid synthesis was apparent in patients with advanced PSC and associated with reduced transplantation-free survival. In a subset of the patients, bile acid synthesis was likely suppressed beyond a tipping point at which any further pharmacological suppression may be futile. Implications for patient stratification and inclusion criteria for clinical trials in PSC warrant further investigation.
Lay summary: We show, by measuring the level of the metabolite C4 in the blood from patients with primary sclerosing cholangitis (PSC), that low production of bile acids in the liver predicts a more rapid progression to severe disease. Many people with PSC appear to have fully suppressed bile acid production, and both established and new drugs that aim to reduce bile acid production may therefore be futile for them. We propose C4 as a test to find those likely to respond to these treatments.
Keywords: 7α-Hydroxy-4-cholesten-3-one; AOM, Amsterdam–Oxford model; ASBT, apical sodium-dependent bile acid cotransporter; Biliary disease; C4; C4, 7α-hydroxy-4-cholesten-3-one; CYP7A1, cytochrome P450 family 7 subfamily A member 1; Cholestasis; Cholestatic liver disease; FGF19, fibroblast growth factor 19; FXR, farnesoid X receptor; GUDCA, glycooursodeoxycholic acid; HR, hazard ratio; IBAT, ileal bile acid transporter; Liver transplantation; Liver transplantation-free survival; MELD, model for end-stage liver disease; PBC, primary biliary cholangitis; PSC, primary sclerosing cholangitis; STROBE, Strengthening the Reporting of Observational Studies in Epidemiology; TUDCA, tauroursodeoxycholic acid; UDCA, ursodeoxycholic acid; UPLC-MS/MS, ultraperformance liquid chromatography–tandem mass spectrometry; Ursodeoxycholic acid; c-index, concordance index; liver.
© 2022 The Authors.
Conflict of interest statement
JRH reports receiving consultant fees from Novartis and Orkla Health, lecture honoraria from Roche, and research funding from Biogen, none of which relate to this work. HUM reports receiving consultant fees from Calliditas, Mirum, and Zealand, and lecture honoraria from Albireo, none of which relate to this work. MV reports receiving lecture honoraria from Siemens Healthineers and Intercept, none of which relate to this work. Please refer to the accompanying ICMJE disclosure forms for further details.
Figures


Similar articles
-
Prolonged fibroblast growth factor 19 response in patients with primary sclerosing cholangitis after an oral chenodeoxycholic acid challenge.Hepatol Int. 2017 Jan;11(1):132-140. doi: 10.1007/s12072-016-9769-7. Epub 2016 Sep 30. Hepatol Int. 2017. PMID: 27696157 Free PMC article.
-
Protective potential of the gallbladder in primary sclerosing cholangitis.JHEP Rep. 2022 Dec 17;5(4):100649. doi: 10.1016/j.jhepr.2022.100649. eCollection 2023 Apr. JHEP Rep. 2022. PMID: 36923239 Free PMC article.
-
Loss of apical sodium bile acid transporter alters bile acid circulation and reduces biliary damage in cholangitis.Am J Physiol Gastrointest Liver Physiol. 2023 Jan 1;324(1):G60-G77. doi: 10.1152/ajpgi.00112.2022. Epub 2022 Nov 21. Am J Physiol Gastrointest Liver Physiol. 2023. PMID: 36410025 Free PMC article.
-
A Current Understanding of Bile Acids in Chronic Liver Disease.J Clin Exp Hepatol. 2022 Jan-Feb;12(1):155-173. doi: 10.1016/j.jceh.2021.08.017. Epub 2021 Aug 23. J Clin Exp Hepatol. 2022. PMID: 35068796 Free PMC article. Review.
-
PPAR-Mediated Bile Acid Glucuronidation: Therapeutic Targets for the Treatment of Cholestatic Liver Diseases.Cells. 2024 Aug 1;13(15):1296. doi: 10.3390/cells13151296. Cells. 2024. PMID: 39120326 Free PMC article. Review.
Cited by
-
Bile Acids-Based Therapies for Primary Sclerosing Cholangitis: Current Landscape and Future Developments.Cells. 2024 Oct 4;13(19):1650. doi: 10.3390/cells13191650. Cells. 2024. PMID: 39404413 Free PMC article. Review.
-
Primary sclerosing cholangitis.Nat Rev Dis Primers. 2025 Mar 13;11(1):17. doi: 10.1038/s41572-025-00600-x. Nat Rev Dis Primers. 2025. PMID: 40082445 Review.
-
Fecal deoxycholic acid associates with diet, intestinal microbes, and total bilirubin in primary sclerosing cholangitis.JHEP Rep. 2024 Aug 22;6(12):101188. doi: 10.1016/j.jhepr.2024.101188. eCollection 2024 Dec. JHEP Rep. 2024. PMID: 39624235 Free PMC article.
-
Alterations in bile acid kinetics after bariatric surgery in patients with obesity with or without type 2 diabetes.EBioMedicine. 2024 Aug;106:105265. doi: 10.1016/j.ebiom.2024.105265. Epub 2024 Aug 2. EBioMedicine. 2024. PMID: 39096744 Free PMC article.
-
Bile Acid Signaling in Metabolic and Inflammatory Diseases and Drug Development.Pharmacol Rev. 2024 Oct 16;76(6):1221-1253. doi: 10.1124/pharmrev.124.000978. Pharmacol Rev. 2024. PMID: 38977324 Review.
References
-
- Boonstra K., Weersma R.K., van Erpecum K.J., Rauws E.A., Spanier B.W.M., Poen A.C., et al. Population-based epidemiology, malignancy risk, and outcome of primary sclerosing cholangitis. Hepatology. 2013;58:2045–2055. - PubMed
-
- Corpechot C., Gaouar F., El Naggar A., Kemgang A., Wendum D., Poupon R., et al. Baseline values and changes in liver stiffness measured by transient elastography are associated with severity of fibrosis and outcomes of patients with primary sclerosing cholangitis. Gastroenterology. 2014;146:970–979. - PubMed
-
- Vesterhus M., Hov J.R., Holm A., Schrumpf E., Nygård S., Godang K., et al. Enhanced liver fibrosis score predicts transplant-free survival in primary sclerosing cholangitis. Hepatology. 2015;62:188–197. - PubMed
-
- de Vries E.M.G., Färkkilä M., Milkiewicz P., Hov J.R., Eksteen B., Thorburn D., et al. Enhanced liver fibrosis test predicts transplant-free survival in primary sclerosing cholangitis, a multi-centre study. Liver Int. 2017;37:1554–1561. - PubMed
-
- Vesterhus M., Holm A., Hov J.R., Nygård S., Schrumpf E., Melum E., et al. Novel serum and bile protein markers predict primary sclerosing cholangitis disease severity and prognosis. J Hepatol. 2017;66:1214–1222. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

