Genetic effects of iron levels on liver injury and risk of liver diseases: A two-sample Mendelian randomization analysis
- PMID: 36185655
- PMCID: PMC9523310
- DOI: 10.3389/fnut.2022.964163
Genetic effects of iron levels on liver injury and risk of liver diseases: A two-sample Mendelian randomization analysis
Abstract
Background and aims: Although iron homeostasis has been associated with liver function in many observational studies, the causality in this relationship remains unclear. By using Mendelian Randomization analyses, we aimed to evaluate the genetic effects of increased systemic iron levels on the risk of liver injury and various liver diseases. Moreover, in light of the sex-dependent iron regulation in human beings, we further estimated the sex-specific effect of iron levels in liver diseases.
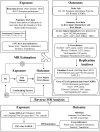
Methods: Independent single nucleotide polymorphisms associated with systemic iron status (including four indicators) at the genome-wide significance level from the Genetics of Iron Status (GIS) Consortium were selected as instrumental variables. Summary data for six liver function biomarkers and five liver diseases were obtained from the UK Biobank, the Estonian Biobank, the eMERGE network, and FinnGen consortium. Mendelian Randomization assessment of the effect of iron on liver function and liver diseases was conducted.
Results: Genetically predicted iron levels were positively and significantly associated with an increased risk of different dimensions of liver injury. Furthermore, increased iron status posed hazardous effects on non-alcoholic fatty liver disease, alcoholic liver disease, and liver fibrosis/cirrhosis. Sex-stratified analyses indicated that the hepatoxic role of iron might exist in NAFLD and liver fibrosis/cirrhosis development among men. No significantly causal relationship was found between iron status and viral hepatitis.
Conclusion: Our study adds to current knowledge on the genetic role of iron in the risk of liver injury and related liver diseases, which provides clinical and public health implications for liver disease prevention as iron status can be modified.
Keywords: iron; liver fibrosis/ cirrhosis; liver injury; mendelian randomization; non-alcoholic fatty liver disease.
Copyright © 2022 Wang, Yang, Zhang, Yang and Jiang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures





Similar articles
-
Iron status and non-alcoholic fatty liver disease: A Mendelian randomization study.Nutrition. 2024 Feb;118:112295. doi: 10.1016/j.nut.2023.112295. Epub 2023 Nov 2. Nutrition. 2024. PMID: 38103266
-
Associations of non-alcoholic fatty liver disease and cirrhosis with liver cancer in European and East Asian populations: A Mendelian randomization study.Cancer Rep (Hoboken). 2024 Jan;7(1):e1913. doi: 10.1002/cnr2.1913. Epub 2023 Oct 16. Cancer Rep (Hoboken). 2024. PMID: 37840448 Free PMC article.
-
Causal impacts of educational attainment on chronic liver diseases and the mediating pathways: Mendelian randomization study.Liver Int. 2023 Nov;43(11):2379-2392. doi: 10.1111/liv.15669. Epub 2023 Jul 6. Liver Int. 2023. PMID: 37409353
-
Causal relationships between metabolic-associated fatty liver disease and iron status: Two-sample Mendelian randomization.Liver Int. 2022 Dec;42(12):2759-2768. doi: 10.1111/liv.15455. Epub 2022 Oct 28. Liver Int. 2022. PMID: 36226474
-
Folic acid supplementation and malaria susceptibility and severity among people taking antifolate antimalarial drugs in endemic areas.Cochrane Database Syst Rev. 2022 Feb 1;2(2022):CD014217. doi: 10.1002/14651858.CD014217. Cochrane Database Syst Rev. 2022. PMID: 36321557 Free PMC article.
Cited by
-
Exploring the Role of Metabolic Hyperferritinaemia (MHF) in Steatotic Liver Disease (SLD) and Hepatocellular Carcinoma (HCC).Cancers (Basel). 2025 Feb 28;17(5):842. doi: 10.3390/cancers17050842. Cancers (Basel). 2025. PMID: 40075688 Free PMC article. Review.
-
Genetically determined circulating micronutrients and the risk of nonalcoholic fatty liver disease.Sci Rep. 2024 Jan 11;14(1):1105. doi: 10.1038/s41598-024-51609-3. Sci Rep. 2024. PMID: 38212362 Free PMC article.
-
Iron Homeostasis as a Mediator Linking Central Obesity with MASLD and Primary Liver Cancer: A Two-Step Mendelian Randomization Study.Biomedicines. 2025 Jul 4;13(7):1641. doi: 10.3390/biomedicines13071641. Biomedicines. 2025. PMID: 40722713 Free PMC article.
-
Contribution of Aflatoxin B1 Exposure to Liver Cirrhosis in Eastern Ethiopia: A Case-Control Study.Int J Gen Med. 2023 Aug 16;16:3543-3553. doi: 10.2147/IJGM.S425992. eCollection 2023. Int J Gen Med. 2023. PMID: 37605782 Free PMC article.
-
Associations of genetically predicted iron status with 24 gastrointestinal diseases and gut microbiota: a Mendelian randomization study.Front Genet. 2024 Aug 7;15:1406230. doi: 10.3389/fgene.2024.1406230. eCollection 2024. Front Genet. 2024. PMID: 39170693 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources

