Nonalcoholic fatty liver disease and diabetes
- PMID: 36188142
- PMCID: PMC9521438
- DOI: 10.4239/wjd.v13.i9.668
Nonalcoholic fatty liver disease and diabetes
Abstract
Nonalcoholic fatty liver disease (NAFLD) is the most prevalent chronic liver disease in the world and represents a clinical-histopathologic entity where the steatosis component may vary in degree and may or may not have fibrotic progression. The key concept of NAFLD pathogenesis is excessive triglyceride hepatic accumulation because of an imbalance between free fatty acid influx and efflux. Strong epidemiological, biochemical, and therapeutic evidence supports the premise that the primary pathophysiological derangement in most patients with NAFLD is insulin resistance; thus the association between diabetes and NAFLD is widely recognized in the literature. Since NAFLD is the hepatic manifestation of a metabolic disease, it is also associated with a higher cardio-vascular risk. Conventional B-mode ultrasound is widely adopted as a first-line imaging modality for hepatic steatosis, although magnetic resonance imaging represents the gold standard noninvasive modality for quantifying the amount of fat in these patients. Treatment of NAFLD patients depends on the disease severity, ranging from a more benign condition of nonalcoholic fatty liver to nonalcoholic steatohepatitis. Abstinence from alcohol, a Mediterranean diet, and modification of risk factors are recommended for patients suffering from NAFLD to avoid major cardiovascular events, as per all diabetic patients. In addition, weight loss induced by bariatric surgery seems to also be effective in improving liver features, together with the benefits for diabetes control or resolution, dyslipidemia, and hypertension. Finally, liver transplantation represents the ultimate treatment for severe nonalcoholic fatty liver disease and is growing rapidly as a main indication in Western countries. This review offers a comprehensive multidisciplinary approach to NAFLD, highlighting its connection with diabetes.
Keywords: Bariatric surgery; Diabetes; Hepatic steatosis; Liver fibrosis; Nonalcoholic fatty liver disease; Nonalcoholic steatohepatitis.
©The Author(s) 2022. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors have no conflicts of interest to declare.
Figures
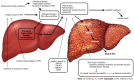

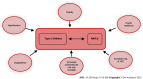
References
-
- Younossi ZM, Golabi P, de Avila L, Paik JM, Srishord M, Fukui N, Qiu Y, Burns L, Afendy A, Nader F. The global epidemiology of NAFLD and NASH in patients with type 2 diabetes: A systematic review and meta-analysis. J Hepatol. 2019;71:793–801. - PubMed
-
- Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M. Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology. 2016;64:73–84. - PubMed
-
- Le MH, Yeo YH, Li X, Li J, Zou B, Wu Y, Ye Q, Huang DQ, Zhao C, Zhang J, Liu C, Chang N, Xing F, Yan S, Wan ZH, Tang NSY, Mayumi M, Liu X, Rui F, Yang H, Yang Y, Jin R, Le RHX, Xu Y, Le DM, Barnett S, Stave CD, Cheung R, Zhu Q, Nguyen MH. 2019 Global NAFLD Prevalence: A Systematic Review and Meta-analysis. Clin Gastroenterol Hepatol. 2021 - PubMed
-
- Loomba R, Schork N, Chen CH, Bettencourt R, Bhatt A, Ang B, Nguyen P, Hernandez C, Richards L, Salotti J, Lin S, Seki E, Nelson KE, Sirlin CB, Brenner D Genetics of NAFLD in Twins Consortium. Heritability of Hepatic Fibrosis and Steatosis Based on a Prospective Twin Study. Gastroenterology. 2015;149:1784–1793. - PMC - PubMed
-
- Caldwell SH, Oelsner DH, Iezzoni JC, Hespenheide EE, Battle EH, Driscoll CJ. Cryptogenic cirrhosis: clinical characterization and risk factors for underlying disease. Hepatology. 1999;29:664–669. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

