Spatial Relation Between White Matter Hyperintensities and Incident Lacunes of Presumed Vascular Origin: A 14-Year Follow-Up Study
- PMID: 36189679
- PMCID: PMC9698104
- DOI: 10.1161/STROKEAHA.122.039903
Spatial Relation Between White Matter Hyperintensities and Incident Lacunes of Presumed Vascular Origin: A 14-Year Follow-Up Study
Abstract
Background: The underlying mechanisms of incident lacunes regarding their spatial distribution remain largely unknown. We investigated the spatial distribution pattern and MRI predictors of incident lacunes in relation to white matter hyperintensity (WMH) over 14 years follow-up in sporadic small vessel disease.
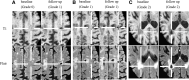
Methods: Five hundred three participants from the ongoing prospective single-center Radboud University Nijmegen Diffusion Tensor and Magnetic resonance Cohort (RUN DMC) were recruited with baseline assessment in 2006 and follow ups in 2011, 2015, and 2020. Three hundred eighty-two participants who underwent at least 2 available brain MRI scans were included. Incident lacunes were systematically identified, and the spatial relationship between incident lacunes located in subcortical white matter and WMH were determined using a visual rating scale. Adjusted multiple logistic regression and linear mixed-effect regression models were used to assess the association between baseline small vessel disease markers, WMH progression, and incident lacunes. Participants with atrial fibrillation were excluded in multivariable analysis.
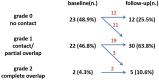
Results: Eighty incident lacunes were identified in 43 patients (mean age 66.5±8.2 years, 37.2% women) during a mean follow-up time of 11.2±3.3 years (incidence rate 10.0/1000 person-year). Sixty percent of incident lacunes were in the white matter, of which 48.9% showed no contact with preexisting WMH. Baseline WMH volume (odds ratio=2.5 [95% CI, 1.6-4.2]) predicted incident lacunes after adjustment for age, sex, and vascular risk factors. WMH progression was associated with incident lacunes independent of age, sex, baseline WMH volume, and vascular risk factors (odds ratio, 3.2 [95% CI, 1.5-6.9]). Baseline WMH volume and progression rate were higher in participants with incident lacunes in contact with preexisting WMH. No difference in vascular risk factors was observed regarding location or relation with preexisting WMH.
Conclusions: The 2 different distribution patterns of lacunes regarding their relation to WMH may suggest distinct underlying mechanisms, one of which may be more closely linked to a similar pathophysiology as that of WMH. The longitudinal relation between WMH and lacunes further supports plausible shared mechanisms between the 2 key markers.
Keywords: incident lacunes; magnetic resonance imaging; small vessel disease; spatial distribution; white matter hyperintensities.
Figures

References
-
- Wardlaw JM, Smith EE, Biessels GJ, Cordonnier C, Fazekas F, Frayne R, Lindley RI, O’Brien JT, Barkhof F, Benavente OR., et al. Neuroimaging standards for research into small vessel disease and its contribution to ageing and neurodegeneration. Lancet Neurol. 2013;12:822–838. doi: 10.1016/S1474-4422(13)70124-8 - PMC - PubMed
-
- van Dijk EJ, Prins ND, Vrooman HA, Hofman A, Koudstaal PJ, Breteler MM. Progression of cerebral small vessel disease in relation to risk factors and cognitive consequences: rotterdam scan study. Stroke. 2008;39:2712–2719. doi: 10.1161/STROKEAHA.107.513176 - PubMed
-
- van Leijsen EMC, Kuiperij HB, Kersten I, Bergkamp MI, van Uden IWM, Vanderstichele H, Stoops E, Claassen J, van Dijk EJ, de Leeuw FE., et al. Plasma abeta (amyloid-beta) levels and severity and progression of small vessel disease. Stroke. 2018;49:884–890. doi: 10.1161/STROKEAHA.117.019810 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

