Temperature management of adult burn patients in intensive care: findings from a retrospective cohort study in a tertiary centre in the United Kingdom
- PMID: 36189905
- PMCID: PMC10156506
- DOI: 10.5114/ait.2022.119131
Temperature management of adult burn patients in intensive care: findings from a retrospective cohort study in a tertiary centre in the United Kingdom
Abstract
Introduction: Patients with major burn injury are prone to hypothermia, potentially resulting in an increase in mortality and length of hospital stay. Our study comprehensively evaluates the practicalities of physiological thermoregulation and temperature control in the largest cohort of critically ill adult burn patients to date.
Material and methods: This retrospective study of routinely collected patient data from the Intensive Care Unit (ICU) of the West Midlands Burn Centre was conducted over a three-year period (2016-2019). Data were analysed to assess temperature control against local and International Society for Burn Injury (ISBI) standards.
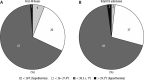
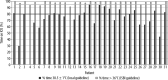
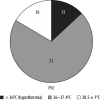
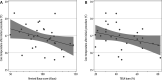
Results: Thirty-one patients with significant burn injuries, requiring active critical care treatment for more than 48 hours were included (total body surface area [TBSA] mean = 42.7%, SD = 18.1%; revised Baux score [rBaux] = 99, SD = 25). The majority were male (77.29%) with an average age of 44 years (17-77 years). The patients were cared for in the ICU for a total of 15 119 hours. Hypothermia, defined as core temperature below 36.0°C, was recorded for 251 hours (2% of total stay). Only 27 patients (87%) had their temperature ≥ 36°C for more than 95% of their admission. Non-survivors were more prone to hypothermia during their stay in ICU. There was an association between rBaux score and post-opera-tive temperature, with a 0.12°C decrease per 10 points increase in rBaux score (P = 0.04).
Conclusions: We have observed a high variability of temperature control between individual patients, especially in non-survivors, and have demonstrated an association between high rBaux score and poor temperature control, specifically during the postoperative period.
Keywords: adult; burn; critical care; hyperthermia; hypothermia; intensive care; intensive therapy; temperature; thermoregulation; surgery.
Conflict of interest statement
none.
Figures

Similar articles
-
Predictive value of quick SOFA and revised Baux scores in burn patients.Burns. 2020 Mar;46(2):347-351. doi: 10.1016/j.burns.2019.03.006. Epub 2019 Dec 16. Burns. 2020. PMID: 31859098
-
Postoperative hypothermia is associated with reduced length of stay in adult acute burn survivors.Burns. 2024 Aug;50(6):1536-1543. doi: 10.1016/j.burns.2024.02.033. Epub 2024 Mar 8. Burns. 2024. PMID: 38705776
-
Long term mortality in critically ill burn survivors.Burns. 2017 Sep;43(6):1155-1162. doi: 10.1016/j.burns.2017.05.010. Epub 2017 Jun 9. Burns. 2017. PMID: 28606748
-
[Management of severe burns during the 1st 72 hours].Ann Fr Anesth Reanim. 1997;16(4):354-69. doi: 10.1016/s0750-7658(97)81462-1. Ann Fr Anesth Reanim. 1997. PMID: 9750581 Review. French.
-
The Revised Baux Score as a Predictor of Burn Mortality: A Systematic Review and Meta-Analysis.J Burn Care Res. 2023 Nov 2;44(6):1278-1288. doi: 10.1093/jbcr/irad075. J Burn Care Res. 2023. PMID: 37220881
Cited by
-
Mind the Gap! Core-Peripheral Temperature Gradient and Its Relationship to Mortality in Major Burns.Eur Burn J. 2025 Mar 2;6(1):11. doi: 10.3390/ebj6010011. Eur Burn J. 2025. PMID: 40137007 Free PMC article.
-
Thermal Imaging as a Method to Indirectly Assess Peripheral Vascular Integrity and Tissue Viability in Veterinary Medicine: Animal Models and Clinical Applications.Animals (Basel). 2023 Dec 31;14(1):142. doi: 10.3390/ani14010142. Animals (Basel). 2023. PMID: 38200873 Free PMC article. Review.
-
An Overview of Recent Developments in the Management of Burn Injuries.Int J Mol Sci. 2023 Nov 15;24(22):16357. doi: 10.3390/ijms242216357. Int J Mol Sci. 2023. PMID: 38003548 Free PMC article. Review.
References
-
- Osilla EV, Marsidi JL, Sharma S. Physiology, Temperature Regulation. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing LLC; 2021. - PubMed
-
- Rizzo JA, Rowan MP, Driscoll IR, Chan RK, Chung KK. Perioperative temperature management during burn care. J Burn Care Res 2017; 38: e277-e283. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
