Epidemiology of ICU-Onset Bloodstream Infection: Prevalence, Pathogens, and Risk Factors Among 150,948 ICU Patients at 85 U.S. Hospitals
- PMID: 36190259
- PMCID: PMC10829879
- DOI: 10.1097/CCM.0000000000005662
Epidemiology of ICU-Onset Bloodstream Infection: Prevalence, Pathogens, and Risk Factors Among 150,948 ICU Patients at 85 U.S. Hospitals
Abstract
Objectives: Bloodstream infections (BSIs) acquired in the ICU represent a detrimental yet potentially preventable condition. We determined the prevalence of BSI acquired in the ICU (ICU-onset BSI), pathogen profile, and associated risk factors.
Design: Retrospective cohort study.
Data sources: Eighty-five U.S. hospitals in the Cerner Healthfacts Database.
Patient selection: Adult hospitalizations between January 2009 and December 2015 including a (≥ 3 d) ICU stay.
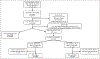
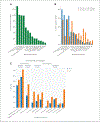
Data extraction and data synthesis: Prevalence of ICU-onset BSI (between ICU Day 3 and ICU discharge) and associated pathogen and antibiotic resistance distributions were compared with BSI present on (ICU) admission (ICU-BSI POA ); and BSI present on ICU admission day or Day 2. Cox models identified risk factors for ICU-onset BSI among host, care setting, and treatment-related factors. Among 150,948 ICU patients, 5,600 (3.7%) had ICU-BSI POA and 1,306 (0.9%) had ICU-onset BSI. Of those with ICU-BSI POA , 4,359 (77.8%) were admitted to ICU at hospital admission day. Patients with ICU-onset BSI (vs ICU-BSI POA ) displayed higher crude mortality of 37.9% (vs 20.4%) ( p < 0.001) and longer median (interquartile range) length of stay of 13 days (8-23 d) (vs 5 d [3-8 d]) ( p < 0.001) (considering all ICU stay). Compared with ICU-BSI POA , ICU-onset BSI displayed more Pseudomonas , Acinetobacter , Enterococcus, Candida , and Coagulase-negative Staphylococcus species, and more methicillin-resistant staphylococci, vancomycin-resistant enterococci, ceftriaxone-resistant Enterobacter , and carbapenem-resistant Enterobacterales and Acinetobacter species, respectively. Being younger, male, Black, Hispanic, having greater comorbidity burden, sepsis, trauma, acute pulmonary or gastrointestinal presentations, and pre-ICU exposure to antibacterial and antifungal agents was associated with greater ICU-onset BSI risk after adjusted analysis. Mixed ICUs (vs medical or surgical ICUs) and urban and small/medium rural hospitals were also associated with greater ICU-onset BSI risk. The associated risk of acquiring ICU-onset BSI manifested with any duration of mechanical ventilation and 7 days after insertion of central venous or arterial catheters.
Conclusions: ICU-onset BSI is a serious condition that displays a unique pathogen and resistance profile compared with ICU-BSI POA . Further scrutiny of modifiable risk factors for ICU-onset BSI may inform control strategies.
Copyright © 2022 by the Society of Critical Care Medicine and Wolters Kluwer Health, Inc. All Rights Reserved.
Conflict of interest statement
Drs. Swihart, Warner, Strich, Follmann, and Kadri received support for article research from the National Institutes of Health. Drs. Swihart, Warner, Strich, Mancera, Follmann, and Kadri disclosed government work. The remaining authors have disclosed that they do not have any potential conflicts of interest.
Figures
Comment in
-
Of Granularity and Generality: ICU-Onset Bloodstream Infections and the Need for Antimicrobial Stewardship and Infection Prevention.Crit Care Med. 2022 Dec 1;50(12):1828-1830. doi: 10.1097/CCM.0000000000005692. Epub 2022 Nov 17. Crit Care Med. 2022. PMID: 36394400 No abstract available.
Similar articles
-
[Current analysis of bloodstream infections in adult intensive care unit patients: a multi-center cohort study of China].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2025 Mar;37(3):232-236. doi: 10.3760/cma.j.cn121430-20240923-00791. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2025. PMID: 40201992 Chinese.
-
Laboratory confirmed bloodstream infection aetiology in an intensive care unit: eight years study.Ann Ig. 2012 Jul-Aug;24(4):269-78. Ann Ig. 2012. PMID: 22913170
-
Methicillin-resistant Staphylococcus aureus central line-associated bloodstream infections in US intensive care units, 1997-2007.JAMA. 2009 Feb 18;301(7):727-36. doi: 10.1001/jama.2009.153. JAMA. 2009. PMID: 19224749
-
Bloodstream infections in the era of the COVID-19 pandemic: Changing epidemiology of antimicrobial resistance in the intensive care unit.J Intensive Med. 2024 Mar 27;4(3):269-280. doi: 10.1016/j.jointm.2023.12.004. eCollection 2024 Jul. J Intensive Med. 2024. PMID: 39035613 Free PMC article. Review.
-
Prevalence, predictors, and mortality of bloodstream infections due to methicillin-resistant Staphylococcus aureus in patients with malignancy: systemic review and meta-analysis.BMC Infect Dis. 2021 Jan 14;21(1):74. doi: 10.1186/s12879-021-05763-y. BMC Infect Dis. 2021. PMID: 33446122 Free PMC article.
Cited by
-
Novel evidence on sepsis-inducing pathogens: from laboratory to bedside.Front Microbiol. 2023 Jun 23;14:1198200. doi: 10.3389/fmicb.2023.1198200. eCollection 2023. Front Microbiol. 2023. PMID: 37426029 Free PMC article. Review.
-
National partnerships address critical needs in infection prevention and control.Antimicrob Steward Healthc Epidemiol. 2024 Dec 2;4(1):e213. doi: 10.1017/ash.2024.447. eCollection 2024. Antimicrob Steward Healthc Epidemiol. 2024. PMID: 39654591 Free PMC article.
-
Multicentre Surveillance of Candida Species from Blood Cultures during the SARS-CoV-2 Pandemic in Southern Europe (CANCoVEU Project).Microorganisms. 2023 Feb 23;11(3):560. doi: 10.3390/microorganisms11030560. Microorganisms. 2023. PMID: 36985134 Free PMC article.
-
Bacterial Infections in Intensive Care Units: Epidemiological and Microbiological Aspects.Antibiotics (Basel). 2024 Mar 5;13(3):238. doi: 10.3390/antibiotics13030238. Antibiotics (Basel). 2024. PMID: 38534673 Free PMC article. Review.
-
Risk and Prognostic Factors for Bloodstream Infections Due to Clonally Transmitted Acinetobacter baumannii ST2 with armA, blaOXA-23, and blaOXA-66: A Retrospective Study.Infect Drug Resist. 2025 Apr 14;18:1867-1879. doi: 10.2147/IDR.S498212. eCollection 2025. Infect Drug Resist. 2025. PMID: 40255460 Free PMC article.
References
-
- Goto M, Al-Hasan MN: Overall burden of bloodstream infection and nosocomial bloodstream infection in North America and Europe. Clin Microbiol Infect 2013; 19:501–509 - PubMed
-
- Garrouste-Orgeas M, Timsit JF, Tafflet M, et al.; OUTCOMEREA Study Group: Excess risk of death from intensive care unit-acquired nosocomial bloodstream infections: A reappraisal. Clin Infect Dis 2006; 42:1118–1126 - PubMed
-
- Vincent JL, Rello J, Marshall J, et al.; EPIC II Group of Investigators: International study of the prevalence and outcomes of infection in intensive care units. JAMA 2009; 302:2323–2329 - PubMed
-
- Tabah A, Koulenti D, Laupland K, et al.: Characteristics and determinants of outcome of hospital-acquired bloodstream infections in intensive care units: The EUROBACT international cohort study. Intensive Care Med 2012; 38:1930–1945 - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

