Heart Transplantation With Older Donors: Should There Be an Age Cutoff?
- PMID: 36192208
- PMCID: PMC11181752
- DOI: 10.1016/j.transproceed.2022.07.004
Heart Transplantation With Older Donors: Should There Be an Age Cutoff?
Abstract
Purpose: Heart transplantation remains limited by donor availability. Currently, only some programs accept older donors, and their use remains contentious. We compared outcomes of heart transplant recipients who received donor hearts ≥55 years with those who received donor hearts <55 years.
Methods: Records of first-time adult heart transplant recipients between 2010 and 2019 were reviewed. Endpoints included 30-day and 1-, 3-, and 5-year survival; freedom from cardiac allograft vasculopathy; freedom from nonfatal major adverse cardiac events; and freedom from any rejections. The effect of donor age ≥55 years was analyzed with Cox proportional hazards modeling, 1:2 propensity score matching, and Kaplan-Meier survival analysis.
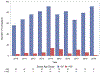
Results: Sixty-six patients received donor hearts ≥55 years and 766 received donor hearts <55 years. In the unmatched cohort, there was no significant difference in survival between the 2 groups at 30 days (93.9% vs 97.3%, P = .127), 1 year (87.9% vs 91.6%, P = .325), 3 years (86.4% vs 86.5%, P = .888), or 5 years (78.8% vs 83.8%, P = .497). The ≥55 years group had a significantly lower freedom from cardiac allograft vasculopathy and fatal major adverse cardiac events. In propensity-matched patients, recipients of donors ≥55 years had similar survival and freedom from cardiac allograft vasculopathy but significantly lower 1-year (76.7% vs 88.3%, P = .026), 3-year (68.3% vs 84.2%, P = .010), and 5-year (63.3% vs 83.3%, P = .002) freedom from nonfatal major adverse cardiac events when compared to recipients of younger donors.
Conclusions: Carefully selected older donors can be considered for a carefully selected group of recipients with acceptable outcomes.
Copyright © 2022 Elsevier Inc. All rights reserved.
Figures
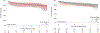

Similar articles
-
Effects of Older Donor Age and Cold Ischemic Time on Long-Term Outcomes of Heart Transplantation.Tex Heart Inst J. 2018 Feb 1;45(1):17-22. doi: 10.14503/THIJ-16-6178. eCollection 2018 Feb. Tex Heart Inst J. 2018. PMID: 29556146 Free PMC article.
-
The policy of placing older donors into older recipients: is it worth the risk?Clin Transplant. 2014 Jul;28(7):802-7. doi: 10.1111/ctr.12382. Epub 2014 Jun 1. Clin Transplant. 2014. PMID: 24801014
-
Outcomes of Early Adolescent Donor Hearts in Adult Transplant Recipients.JACC Heart Fail. 2017 Dec;5(12):879-887. doi: 10.1016/j.jchf.2017.05.004. Epub 2017 Aug 16. JACC Heart Fail. 2017. PMID: 28822746
-
Portable Normothermic Cardiac Perfusion System in Donation After Cardiocirculatory Death: A Health Technology Assessment.Ont Health Technol Assess Ser. 2020 Mar 6;20(3):1-90. eCollection 2020. Ont Health Technol Assess Ser. 2020. PMID: 32190164 Free PMC article.
-
Does ABO-incompatible and ABO-compatible neonatal heart transplant have equivalent survival?Interact Cardiovasc Thorac Surg. 2010 Jun;10(6):1026-33. doi: 10.1510/icvts.2009.229757. Epub 2010 Mar 22. Interact Cardiovasc Thorac Surg. 2010. PMID: 20308266 Review.
Cited by
-
The future of living organ donation: confronting the challenges and embracing the opportunities of an aging donor population.Int J Surg. 2024 Aug 1;110(8):5260-5261. doi: 10.1097/JS9.0000000000001562. Int J Surg. 2024. PMID: 38759690 Free PMC article. No abstract available.
References
-
- Khush KK, Potena L, Cherikh WS, Chambers DC, Harhay MO, Hayes D, et al. The International Thoracic Organ Transplant Registry of the International Society for Heart and Lung Transplantation: 37th adult heart transplantation report—2020; focus on deceased donor characteristics. J Heart Lung Transplant 2020;39:1003–15. - PMC - PubMed
-
- Kobashigawa J, Khush K, Colvin M, Acker M, Van Bakel A, Eisen H, et al. Report from the American Society of Transplantation conference on donor heart selection in adult cardiac transplantation in the United States. Am J Transplant 2017;17:2559–66. - PubMed
-
- Bruschi G, Colombo T, Oliva F, Morici N, Botta L, Cannata A, et al. Orthotopic heart transplantation with donors greater than or equal to 60 years of age: a single-center experience. Eur J Cardiothorac Surg 2011;40:e55–61. - PubMed
-
- Gupta D, Piacentino V 3rd, Macha M, Singhal AK, Gaughan JP, McClurken JB, et al. Effect of older donor age on risk for mortality after heart transplantation. Ann Thorac Surg 2004;78:890–9. - PubMed
-
- Pedotti P, Mattucci DA, Gabbrielli F, Venettoni S, Costa AN, Taioli E. Analysis of the complex effect of donor’s age on survival of subjects who underwent heart transplantation. Transplantation 2005;80:1026–32. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

