Evaluation of Diffusion-Perfusion Mismatch in Acute Ischemic Stroke with a New Automated Perfusion-Weighted Imaging Software: A Retrospective Study
- PMID: 36201112
- PMCID: PMC9588132
- DOI: 10.1007/s40120-022-00409-w
Evaluation of Diffusion-Perfusion Mismatch in Acute Ischemic Stroke with a New Automated Perfusion-Weighted Imaging Software: A Retrospective Study
Abstract
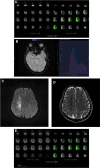
Introduction: The aim of this study was to evaluate the accuracy of automated software (iStroke) on magnetic resonance (MR) apparent diffusion coefficient (ADC) and perfusion-weighted imaging (PWI) against ground truth in assessing infarct core, and compare the hypoperfusion volume and mismatch volume on iStroke with those on Food and Drug Administration-approved software (RAPID) in patients with acute ischemic stroke.
Methods: We used the single-volume decomposition method to develop the iStroke (iStroke; Beijing Tiantan Hospital, Beijing, China) software. Patients with ischemic stroke were collected from two educational hospitals in China with MR-PWI performed in the emergency department within 24 h of symptom onset. Infarct core volume was defined as ADC < 620 × 10-6 mm2/s and hypoperfusion volume was defined as Tmax > 6 s. We compared the accuracy of infarct core volume using iStroke and RAPID (iSchema View Inc, Menlo Park, CA) software with ground truth.
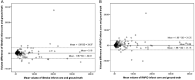
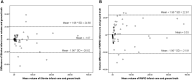
Results: We included 405 patients with acute ischemic stroke with MR ADC and PWI sequences. The infarct core volume on iStroke (median 2.43 ml, interquartile range [IQR] 0.60-10.32 ml) was not significantly different from the ground truth (median 2.89 ml, IQR 0.77-9.17 ml) (P = 0.07); Bland-Altman curves showed that the core volume of iStroke and RAPID software were comparable with each other on individual agreement with ground truth. The hypoperfusion volume and mismatch volume on iStroke were not statistically different from those on the RAPID software, respectively. In patients with large vessel occlusion (n = 74), the agreement between iStroke and RAPID was substantial (kappa = 0.76) according to DEFUSE 3 criteria (infarct core < 70 ml, mismatch volume ≥ 15 ml, and mismatch ratio ≥ 1.8).
Conclusions: The iStroke automatic processing of ADC and PWI is a reliable software for the identification of diffusion-perfusion mismatch in acute ischemic stroke.
Keywords: Infarct; Penumbra; Perfusion-weighted imaging; Software analysis; Stroke.
© 2022. The Author(s).
Figures

Similar articles
-
Assessment of Perfusion Volumes by a New Automated Software for Computed Tomography Perfusion.Stroke Vasc Neurol. 2024 Dec 30;9(6):693-698. doi: 10.1136/svn-2023-002964. Stroke Vasc Neurol. 2024. PMID: 38548327 Free PMC article.
-
Penumbra quantification from MR SWI-DWI mismatch and its comparison with MR ASL PWI-DWI mismatch in patients with acute ischemic stroke.NMR Biomed. 2021 Jul;34(7):e4526. doi: 10.1002/nbm.4526. Epub 2021 Apr 20. NMR Biomed. 2021. PMID: 33880799
-
Automated Perfusion-Diffusion Magnetic Resonance Imaging in Childhood Arterial Ischemic Stroke.Stroke. 2021 Oct;52(10):3296-3304. doi: 10.1161/STROKEAHA.120.032822. Epub 2021 Aug 18. Stroke. 2021. PMID: 34404238
-
Real-time diffusion-perfusion mismatch analysis in acute stroke.J Magn Reson Imaging. 2010 Nov;32(5):1024-37. doi: 10.1002/jmri.22338. J Magn Reson Imaging. 2010. PMID: 21031505 Free PMC article. Review.
-
[Intravenous administration of a tissue plasminogen activator beyond 3 hours of the onset of acute ischemic stroke--MRI-based decision making].Brain Nerve. 2008 Oct;60(10):1173-80. Brain Nerve. 2008. PMID: 18975605 Review. Japanese.
Cited by
-
Rationale and design of Treatment of Acute Ischaemic Stroke with Edaravone Dexborneol II (TASTE-2): a multicentre randomised controlled trial.Stroke Vasc Neurol. 2024 Dec 30;9(6):730-737. doi: 10.1136/svn-2023-002938. Stroke Vasc Neurol. 2024. PMID: 38471696 Free PMC article.
-
Assessment of Perfusion Volumes by a New Automated Software for Computed Tomography Perfusion.Stroke Vasc Neurol. 2024 Dec 30;9(6):693-698. doi: 10.1136/svn-2023-002964. Stroke Vasc Neurol. 2024. PMID: 38548327 Free PMC article.
-
Effect of MR-guided perfusion imaging mismatch profiles within 6 h on endovascular thrombectomy outcomes.Neurol Sci. 2025 Jan;46(1):285-293. doi: 10.1007/s10072-024-07751-x. Epub 2024 Sep 7. Neurol Sci. 2025. PMID: 39242369
References
Grants and funding
LinkOut - more resources
Full Text Sources

