Sociodemographic and clinical factors associated with poor COVID-19 outcomes in patients with rheumatic diseases: data from the SAR-COVID Registry
- PMID: 36201124
- PMCID: PMC9535223
- DOI: 10.1007/s10067-022-06393-8
Sociodemographic and clinical factors associated with poor COVID-19 outcomes in patients with rheumatic diseases: data from the SAR-COVID Registry
Abstract
Background/objective: This study aims to describe the course and to identify poor prognostic factors of SARS-CoV-2 infection in patients with rheumatic diseases.
Methods: Patients ≥ 18 years of age, with a rheumatic disease, who had confirmed SARS-CoV-2 infection were consecutively included by major rheumatology centers from Argentina, in the national, observational SAR-COVID registry between August 13, 2020 and July 31, 2021. Hospitalization, oxygen requirement, and death were considered poor COVID-19 outcomes.
Results: A total of 1915 patients were included. The most frequent rheumatic diseases were rheumatoid arthritis (42%) and systemic lupus erythematosus (16%). Comorbidities were reported in half of them (48%). Symptoms were reported by 95% of the patients, 28% were hospitalized, 8% were admitted to the intensive care unit (ICU), and 4% died due to COVID-19. During hospitalization, 9% required non-invasive mechanical ventilation (NIMV) or high flow oxygen devices and 17% invasive mechanical ventilation (IMV). In multivariate analysis models, using poor COVID-19 outcomes as dependent variables, older age, male gender, higher disease activity, treatment with glucocorticoids or rituximab, and the presence of at least one comorbidity and a greater number of them were associated with worse prognosis. In addition, patients with public health insurance and Mestizos were more likely to require hospitalization.
Conclusions: In addition to the known poor prognostic factors, in this cohort of patients with rheumatic diseases, high disease activity, and treatment with glucocorticoids and rituximab were associated with worse COVID-19 outcomes. Furthermore, patients with public health insurance and Mestizos were 44% and 39% more likely to be hospitalized, respectively.
Study registration: This study has been registered in ClinicalTrials.gov under the number NCT04568421. Key Points • High disease activity, and treatment with glucocorticoids and rituximab were associated with poor COVID-19 outcome in patients with rheumatic diseases. • Some socioeconomic factors related to social inequality, including non-Caucasian ethnicity and public health insurance, were associated with hospitalization due to COVID-19.
Keywords: Argentina; COVID-19; Rheumatic diseases; SARS-CoV-2.
© 2022. The Author(s), under exclusive licence to International League of Associations for Rheumatology (ILAR).
Conflict of interest statement
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: SAR-COVID is a multi-sponsor registry, where Pfizer, Abbvie, and Elea Phoenix provided unrestricted grants. None of them participated or influenced the development of the project, data collection, analysis, interpretation, or writing of the report. They do not have access to the information collected in the database.
Figures
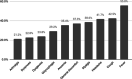

References
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

