Reaction of SARS-CoV-2 antibodies with other pathogens, vaccines, and food antigens
- PMID: 36211404
- PMCID: PMC9537454
- DOI: 10.3389/fimmu.2022.1003094
Reaction of SARS-CoV-2 antibodies with other pathogens, vaccines, and food antigens
Abstract
It has been shown that SARS-CoV-2 shares homology and cross-reacts with vaccines, other viruses, common bacteria and many human tissues. We were inspired by these findings, firstly, to investigate the reaction of SARS-CoV-2 monoclonal antibody with different pathogens and vaccines, particularly DTaP. Additionally, since our earlier studies have shown immune reactivity by antibodies made against pathogens and autoantigens towards different food antigens, we also studied cross-reaction between SARS-CoV-2 and common foods. For this, we reacted monoclonal and polyclonal antibodies against SARS-CoV-2 spike protein and nucleoprotein with 15 different bacterial and viral antigens and 2 different vaccines, BCG and DTaP, as well as with 180 different food peptides and proteins. The strongest reaction by SARS-CoV-2 antibodies were with DTaP vaccine antigen, E. faecalis, roasted almond, broccoli, soy, cashew, α+β casein and milk, pork, rice endochitinase, pineapple bromelain, and lentil lectin. Because the immune system tends to form immune responses towards the original version of an antigen that it has encountered, this cross-reactivity may have its advantages with regards to immunity against SARS-CoV-2, where the SARS-CoV-2 virus may elicit a "remembered" immune response because of its structural similarity to a pathogen or food antigen to which the immune system was previously exposed. Our findings indicate that cross-reactivity elicited by DTaP vaccines in combination with common herpesviruses, bacteria that are part of our normal flora such as E. faecalis, and foods that we consume on a daily basis should be investigated for possible cross-protection against COVID-19. Additional experiments would be needed to clarify whether or not this cross-protection is due to cross-reactive antibodies or long-term memory T and B cells in the blood.
Keywords: SARS-CoV-2; antibodies; food antigens; molecular mimicry; pathogens; vaccines.
Copyright © 2022 Vojdani, Vojdani, Melgar and Redd.
Conflict of interest statement
Corresponding author Aristo Vojdani is the co-owner, CEO and Technical Director of Immunosciences Lab., Inc. He is also the Chief Scientific Advisor of Cyrex Labs, LLC on a consultancy basis. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be constructed as a potential conflict of interest.
Figures

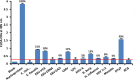

 , 1:400
, 1:400  , and 1:800
, and 1:800  . Note that in proportion to the dilution of the antigens, a significant decline in antibody-antigen reaction is observed. Each determination of antibody-antigen reaction was performed in triplicate. The SDs for all the reactions were less than 0.1, and are shown as error bars.
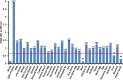
. Note that in proportion to the dilution of the antigens, a significant decline in antibody-antigen reaction is observed. Each determination of antibody-antigen reaction was performed in triplicate. The SDs for all the reactions were less than 0.1, and are shown as error bars.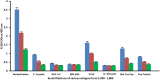
 , 1:400
, 1:400  , and 1:800
, and 1:800  . Note that in proportion to the dilution of the antigens, a significant decline in antibody-antigen reaction is observed only in the antigens with ODs that are >0.5. Each determination of antibody-antigen reaction was performed in triplicate. The SDs for all the reactions were 0.1 or less, and are shown as error bars. .
. Note that in proportion to the dilution of the antigens, a significant decline in antibody-antigen reaction is observed only in the antigens with ODs that are >0.5. Each determination of antibody-antigen reaction was performed in triplicate. The SDs for all the reactions were 0.1 or less, and are shown as error bars. .
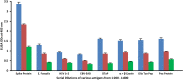
 or nucleoprotein
or nucleoprotein  . Each determination of antigen-antibody reaction was performed in quadruplicate. The SDs for all the reactions were 0.1 or less, and are shown as error bars. * = Antigens whose reactions were under the cutoff and/or close to the blank. WGA, Wheat Germ Agglutinin; Peanut Agg, Peanut Agglutinin; Soy Agg, Soy Agglutinin; PHA, Phytohemagglutinin. Percentages of significant reactivity are also shown.
. Each determination of antigen-antibody reaction was performed in quadruplicate. The SDs for all the reactions were 0.1 or less, and are shown as error bars. * = Antigens whose reactions were under the cutoff and/or close to the blank. WGA, Wheat Germ Agglutinin; Peanut Agg, Peanut Agglutinin; Soy Agg, Soy Agglutinin; PHA, Phytohemagglutinin. Percentages of significant reactivity are also shown.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

