Two cases of extramedullary plasmacytoma of the small intestine presenting with ileus: A case report
- PMID: 36221423
- PMCID: PMC9542664
- DOI: 10.1097/MD.0000000000030842
Two cases of extramedullary plasmacytoma of the small intestine presenting with ileus: A case report
Abstract
Background: Extramedullary (extraosseous) plasmacytoma (EMP) of the small intestine is a rare plasma cell neoplasm (PCN) that presents with abdominal pain, nausea, vomiting, etc. We describe 2 cases of EMP of the small intestine that presented with ileus.
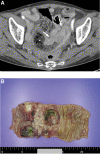
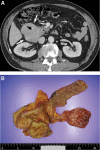
Methods: A 78-year-old woman and 68-year-old man visited our clinic with complaints of abdominal discomfort and obstruction. Abdominal computed tomography (CT) revealed a thickened lesion with multiple enlarged mesenteric lymph nodes (LNs) in the ileum and duodenum. The female patient underwent segmental resection in the ileum. The male patient underwent Whipple's operation in the duodenum.
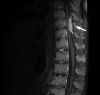
Results: Histopathological examination and immunohistochemical staining of resected specimens from the 2 patients confirmed a PCN. In the surgical specimens of 2 cases, immunoglobulin heavy-chain rearrangement was confirmed by polymerase chain reaction amplification, but no Epstein-Barr virus (EBV)-infected cells were found by EBV-in situ hybridization. Bone marrow aspirate and trephine biopsies were negative for the type of PCN. Bone marrow cytogenetics and fluorescence in situ hybridization revealed no abnormalities. Serum β2-microglobulin levels were within normal limits. Additionally, none of the patients showed an M-spike in serum or urine protein electrophoresis. Therefore, the patients were diagnosed with a solitary EMP of the small intestine. The female patient refused treatment. At follow-up 3 months postoperatively, her disease progressed and she newly developed multiple LNs and nodular lesions in the right pelvic side wall. She was treated with dexamethasone. The male patient experienced back pain 25 days after Whipple's operation. Spine series magnetic resonance imaging revealed an intermediate signal intensity mass in the posterior epidural space from T8/9 to T10. The mass was removed, and the same histologic features were identified as duodenal masses. He was treated with dexamethasone and radiotherapy.
Conclusions: EMPs of the small intestine are easy to overlook because they rarely occur in the small intestine. Although surgery is not required for diagnosis, surgical resection can be a good option for EMPs of the small intestine, instead of local radiation therapy. However, close follow-up is required due to the possibility of relapse or progression to plasma cell myeloma.
Copyright © 2022 the Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures


References
-
- Alexiou C, Kau RJ, Dietzfelbinger H, et al. . Extramedullary plasmacytoma: tumor occurrence and therapeutic concepts. Cancer. 1999;85:2305–14. - PubMed
-
- Lopes da SR. Extramedullary plasmacytoma of the small intestine: clinical features, diagnosis and treatment. J Dig Dis. 2012;13:10–8. - PubMed
-
- Group IMW. Criteria for the classification of monoclonal gammopathies, multiple myeloma and related disorders: a report of the International Myeloma Working Group. Br J Haematol. 2003;121:749–57. - PubMed
-
- Chao MW, Gibbs P, Wirth A, et al. . Radiotherapy in the management of solitary extramedullary plasmacytoma. Intern Med J. 2005;35:211–5. - PubMed
-
- Liebross RH, Ha CS, Cox JD, et al. . Clinical course of solitary extramedullary plasmacytoma. Radiother Oncol. 1999;52:245–9. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

