PPARδ Agonist Promotes Type II Cartilage Formation in a Rabbit Osteochondral Defect Model
- PMID: 36230897
- PMCID: PMC9564068
- DOI: 10.3390/cells11192934
PPARδ Agonist Promotes Type II Cartilage Formation in a Rabbit Osteochondral Defect Model
Abstract
Osteoarthritis (OA) is a chronic degenerative joint disease accompanied by an inflammatory milieu that results in painful joints. The pathogenesis of OA is multifactorial, with genetic predisposition, environmental factors, and traumatic injury resulting in the direct or indirect loss of cartilage. The articular cartilage can also be damaged by direct focal traumatic injury. Articular cartilage provides a smooth, deformable bearing surface with a low coefficient of friction, increased contact area, and reduced contact stress. Articular type II hyaline cartilage lines the synovial joints and, when injured, has a limited ability for repair, except for the most superficial layers via diffusion from the synovial fluid, secondary to no blood supply, a complex structure, and a low metabolic rate. Restoring the articular surface can relieve pain and restore function. Although many strategies have been developed to regenerate type II collagen based on the extent of the lesion, surgical treatments are still evolving. The peroxisome proliferator-activated receptor delta (PPARδ) agonist and collagen treatment of mesenchymal stem cells (MSCs) enhance the chondrogenic capacity in vitro. We present a novel technique for cartilage restoration in a rabbit cartilage osteochondral defect model using a PPARδ agonist (GW0742)-infused 3D collagen scaffold to induce type II cartilage from MSCs.
Keywords: 3D collagen scaffold; mesenchymal stem cells; osteoarthritis; peroxisome proliferator-activated receptor delta; type II collagen; type II hyaline cartilage.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



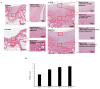

References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

