Tricuspid Valve Damage Related to Transvenous Lead Extraction
- PMID: 36231579
- PMCID: PMC9566121
- DOI: 10.3390/ijerph191912279
Tricuspid Valve Damage Related to Transvenous Lead Extraction
Abstract
Background: Damage to the tricuspid valve (TVD) is now considered either a major or minor complication of the transvenous lead extraction procedure (TLE). As yet, the risk factors and long-term survival after TLE in patients with TVD have not been analyzed in detail.
Methods: This post hoc analysis used clinical data of 2631 patients (mean age 66.86 years, 39.64% females) who underwent TLE procedures performed in three high-volume centers. The risk factors and long-term survival of patients with worsening tricuspid valve (TV) function after TLE were analyzed.
Results: In most procedures (90.31%), TLE had no negative influence on TV function, but in 9.69% of patients, a worsening of tricuspid regurgitation (TR) to varying degrees was noted, including significant dysfunction in 2.54% of patients. Risk factors of TLE relating to severe TVD were: TLE of pacing leads (5.264; p = 0.029), dwell time of the oldest extracted lead (OR = 1.076; p = 0.032), strong connective scar tissue connecting a lead with tricuspid apparatus (OR = 5.720; p < 0.001), and strong connective scar tissue connecting a lead with the right ventricle wall (OR = 8.312; p < 0.001). Long-term survival (1650 ± 1201 [1-5519] days) of patients with severe TR was comparable to patients without tricuspid damage related to TLE.
Conclusions: Severe tricuspid valve damage related to TLE is relatively rare (2.5%). The main risk factors for the worsening of TV function are associated with a longer lead dwell time (more often the pacing lead), causing stronger connective tissue scars connecting the lead to the tricuspid apparatus and right ventricle. TVD is unlikely to affect long-term survival after TLE.
Keywords: long-term survival; risk factors; transvenous lead extraction complications; tricuspid valve damage.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

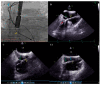
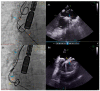
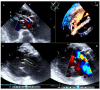
References
-
- Love C.J., Wilkoff B.L., Byrd C.L., Belott P.H., Brinker J.A., Fearnot N.E., Friedman R.A., Furman S., Goode L.B., Hayes D.L., et al. Recommendations for extraction of chronically implanted transvenous pacing and defibrillator leads: Indications, facilities, training. North American Society of Pacing and Electrophysiology Lead Extraction Conference Faculty. Pacing Clin. Electrophysiol. 2000;23:544–551. - PubMed
-
- Wilkoff B.L., Love C.J., Byrd C.L., Bongiorni M.G., Carrillo R.G., Crossley G.H., 3rd, Epstein L.M., Friedman R.A., Kennergren C.E., Mitkowski P., et al. Transvenous lead extraction: Heart Rhythm Society expert consensus on facilities, training, indications, and patient management: This document was endorsed by the American Heart Association (AHA) Heart Rhythm. 2009;6:1085–1104. doi: 10.1016/j.hrthm.2009.05.020. - DOI - PubMed
-
- Deharo J.C., Bongiorni M.G., Rozkovec A., Bracke F., Defaye P., Fernandez-Lozano I., Golzio P.G., Hansky B., Kennergren C., Manolis A.S., et al. Pathways for training and accreditation for transvenous lead extraction: A European Heart Rhythm Association position paper. Europace. 2012;14:124–134. - PubMed
-
- Kusumoto F.M., Schoenfeld M.H., Wilkoff B., Berul C.I., Birgersdotter-Green U.M., Carrillo R., Cha Y.M., Clancy J., Deharo J.C., Ellenbogen KAExner D., et al. 2017 HRS expert consensus statement on cardiovascular implantable electronic device lead management and extraction. Heart Rhythm. 2017;14:e503–e551. doi: 10.1016/j.hrthm.2017.09.001. - DOI - PubMed
-
- Bongiorni M.G., Burri H., Deharo J.C., Starck C., Kennergren C., Saghy L., Rao A., Tascini C., Lever N., Kutarski A., et al. 2018 EHRA expert consensus statement on lead extraction: Recommendations on definitions, endpoints, research trial design, and data collection requirements for clinical scientific studies and registries: Endorsed by APHRS/HRS/LAHRS. Europace. 2012;14:994–1001. doi: 10.1093/europace/euy050. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

