[Gastrointestinal Emergencies in Neonates: What We Should Know]
- PMID: 36238170
- PMCID: PMC9432200
- DOI: 10.3348/jksr.2020.81.4.770
[Gastrointestinal Emergencies in Neonates: What We Should Know]
Abstract
Newborn gastrointestinal tract emergency diseases include various disorders that occur anywhere along the digestive tract. Most of them are congenital malformations, not acquired diseases. Many of them cannot be confirmed on prenatal examination, and consequently, postnatal evaluation is required. Unlike adults, in newborn babies, detailed evaluations with computed tomography (CT) and magnetic resonance imaging (MRI) are often limited, so making the diagnosis based on early abdominal radiography is most important. Therefore, it is necessary to be familiar with the radiologic findings that may be seen on imaging studies. In addition, it is important to understand abdominal ultrasound and fluoroscopy findings, which can be used in addition to simple radiography and indications that can be used for further diagnosis and appropriate treatment. Therefore, this study describes and organizes the various imaging findings that may occur in neonatal gastrointestinal emergencies.
신생아 위장관 응급 질환은 소화관을 따라 어디에서나 발생하는 다양한 장애를 포함한다. 이러한 질환들의 경우 대부분 후천성 질환이 아닌 선천성 기형에 의한 것이나 산전 검사에서 확인되지 않은 경우도 많아 이에 대한 산후 평가가 필요하게 된다. 이 시기의 신생아의 경우 성인과 달리 전산화단층촬영(computed tomography; 이하 CT)과 자기공명영상(magnetic resonance imaging; 이하 MRI)이 제한적인 경우가 많아 초기 복부 방사선 촬영에서의 진단이 중요하게 되어 복부 방사선 촬영에서 보일 수 있는 소견들에 대해 숙지하는 것이 필요하다. 또한 추가적으로 진단에 사용될 수 있는 복부 초음파, 투시 검사의 소견, 적응증에 대해 이해하는 것이 진단과 이에 따른 적절한 처치를 위해 중요하다. 이에 이 논문에서는 신생아 위장관 응급 질환에서 나타날 수 있는 다양한 영상 소견에 대해 기술하고 정리하였다.
Copyrights © 2020 The Korean Society of Radiology.
Conflict of interest statement
Conflicts of Interest: The authors have no potential conflicts of interest to disclose.
Figures








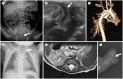

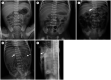

Similar articles
-
Neonatal gastrointestinal emergencies: a radiological review.Arch Pediatr. 2022 Apr;29(3):159-170. doi: 10.1016/j.arcped.2022.01.016. Epub 2022 Mar 3. Arch Pediatr. 2022. PMID: 35249799 Free PMC article. Review.
-
Fetal Neurosonogaphy: Ultrasound and Magnetic Resonance Imaging in Competition.Ultraschall Med. 2016 Dec;37(6):555-557. doi: 10.1055/s-0042-117142. Epub 2016 Dec 15. Ultraschall Med. 2016. PMID: 27978593 English.
-
Usefulness of additional fetal magnetic resonance imaging in the prenatal diagnosis of congenital abnormalities.Arch Gynecol Obstet. 2012 Dec;286(6):1443-52. doi: 10.1007/s00404-012-2474-4. Epub 2012 Aug 9. Arch Gynecol Obstet. 2012. PMID: 22875047
-
[Neonatal gastrointestinal emergencies].Radiologe. 2000 Jan;40(1):63-71. doi: 10.1007/s001170050010. Radiologe. 2000. PMID: 10663165 Review. German.
-
Clinical assessment and brain findings in a cohort of mothers, fetuses and infants infected with ZIKA virus.Am J Obstet Gynecol. 2018 Apr;218(4):440.e1-440.e36. doi: 10.1016/j.ajog.2018.01.012. Epub 2018 Jan 17. Am J Obstet Gynecol. 2018. PMID: 29353032
Cited by
-
Incidentally Diagnosed Duodenal Web in Infancy.Taehan Yongsang Uihakhoe Chi. 2022 May;83(3):724-729. doi: 10.3348/jksr.2021.0047. Epub 2022 Apr 20. Taehan Yongsang Uihakhoe Chi. 2022. PMID: 36238499 Free PMC article.
-
[Malrotation and Midgut Volvulus in Children: Diagnostic Approach, Imaging Findings, and Pitfalls].J Korean Soc Radiol. 2024 Jan;85(1):124-137. doi: 10.3348/jksr.2023.0002. Epub 2023 Nov 15. J Korean Soc Radiol. 2024. PMID: 38362395 Free PMC article. Review. Korean.
References
-
- Vinocur DN, Lee EY, Eisenberg RL. Neonatal intestinal obstruction. AJR Am J Roentgenol. 2012;198:W1–W10. - PubMed
-
- Hernanz-Schulman M. Imaging of neonatal gastrointestinal obstruction. Radiol Clin North Am. 1999;37:1163–1186. vi-vii. - PubMed
-
- McAlister WH, Kronemer KA. Emergency gastrointestinal radiology of the newborn. Radiol Clin North Am. 1996;34:819–844. - PubMed
-
- Rao P. Neonatal gastrointestinal imaging. Eur J Radiol. 2006;60:171–186. - PubMed
-
- Cumming WA, Williams JL. Neonatal gastrointestinal imaging. Clin Perinatol. 1996;23:387–407. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

