Modification of the eighth AJCC/UICC staging system for perihilar cholangiocarcinoma: An alternative pathological staging system from cholangiocarcinoma-prevalent Northeast Thailand
- PMID: 36250068
- PMCID: PMC9561347
- DOI: 10.3389/fmed.2022.893252
Modification of the eighth AJCC/UICC staging system for perihilar cholangiocarcinoma: An alternative pathological staging system from cholangiocarcinoma-prevalent Northeast Thailand
Abstract
Aim: This study aims to improve the classification performance of the eighth American Joint Committee on Cancer (AJCC) staging system for perihilar cholangiocarcinoma (pCCA) by proposing the Khon Kaen University (KKU) staging system developed in cholangiocarcinoma-prevalent Northeast Thailand.
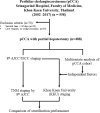
Method: Four hundred eighty-eight patients with pCCA who underwent partial hepatectomy between 2002 and 2017 at the Srinagarind Hospital, Faculty of Medicine, Khon Kaen University, Thailand, were included. Overall survival (OS) related to clinicopathological features was analyzed using the Kaplan-Meier method. Logrank test was performed in univariate analysis to compare OS data of clinicopathological features to determine risk factors for poor survival. Significant features were further analyzed by multivariate analysis (Cox regression) to identify prognostic factors which were then employed to modify the eighth AJCC staging system.
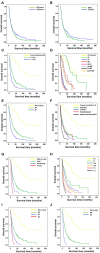
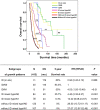
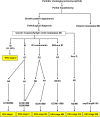
Results: Multivariate analysis showed that growth pattern (HR = 4.67-19.72, p < 0.001), moderately and poorly differentiated histological grades (HR = 2.31-4.99, p < 0.05 and 0.001, respectively), lymph node metastasis N1 and N2 (HR = 1.37 and 2.18, p < 0.05 and 0.01, respectively), and distant metastasis (HR = 2.11, p < 0.001) were independent factors when compared to their respective reference groups. There was a clear separation of patients with pCCA into KKU stage: I [OS = 116 months (mo.)], II (OS = 46 mo.), IIIA (OS = 24 mo.), IIIB (11 mo.), IVA (OS = 7 mo.), and IVB (OS = 6 mo.).
Conclusion: The new staging system was based on the incorporation of growth patterns to modify the eighth AJCC staging system. The classification performance demonstrated that the KKU staging system was able to classify and distinctly separate patients with pCCA into those with good and poor outcomes. It was also able to improve the stratification performance and discriminative ability of different stages of pCCA classification better than the eighth AJCC staging system. Hence, the KKU staging system is proposed as an alternative model to augment the accuracy of survival prognostication and treatment performance for patients with pCCA.
Keywords: KKU staging system; classification; eighth AJCC/UICC staging; growth pattern; perihilar cholangiocarcinoma.
Copyright © 2022 Aphivatanasiri, Sa-Ngiamwibool, Sangkhamanon, Intarawichian, Kunprom, Thanee, Prajumwongs, Khuntikeo, Titapun, Jareanrat, Thanasukarn, Srisuk, Luvira, Eurboonyanun, Promsorn, Loilome, Wee and Koonmee.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures




Similar articles
-
Modification of the AJCC/UICC 8th edition staging system for intrahepatic cholangiocarcinoma: proposal for an alternative staging system from cholangiocarcinoma-prevalent Northeast Thailand.HPB (Oxford). 2022 Nov;24(11):1944-1956. doi: 10.1016/j.hpb.2022.06.004. Epub 2022 Jun 20. HPB (Oxford). 2022. PMID: 35810105
-
External validation study of the 8th edition of the American Joint Committee on Cancer staging system for perihilar cholangiocarcinoma: a single-center experience in China and proposal for simplification.J Gastrointest Oncol. 2021 Apr;12(2):806-818. doi: 10.21037/jgo-20-348. J Gastrointest Oncol. 2021. PMID: 34012668 Free PMC article.
-
A new clinically based staging system for perihilar cholangiocarcinoma.Am J Gastroenterol. 2014 Dec;109(12):1881-90. doi: 10.1038/ajg.2014.327. Epub 2014 Nov 11. Am J Gastroenterol. 2014. PMID: 25384902 Free PMC article.
-
Surgical management of perihilar cholangiocarcinoma: a Khon Kaen experience.J Hepatobiliary Pancreat Sci. 2014 Aug;21(8):521-4. doi: 10.1002/jhbp.74. Epub 2014 Jan 27. J Hepatobiliary Pancreat Sci. 2014. PMID: 24464976 Review.
-
The pros and cons of the PCC staging system to guide surgical resectability and prognosis.J Cancer. 2022 Oct 9;13(13):3444-3451. doi: 10.7150/jca.76696. eCollection 2022. J Cancer. 2022. PMID: 36313036 Free PMC article. Review.
Cited by
-
Improvement of survival outcomes of cholangiocarcinoma by ultrasonography surveillance: Multicenter retrospective cohorts.Heliyon. 2024 Sep 20;10(18):e38191. doi: 10.1016/j.heliyon.2024.e38191. eCollection 2024 Sep 30. Heliyon. 2024. PMID: 39381227 Free PMC article.
-
Endobiliary radiofrequency ablation in recurrence and unresectable Perihilar cholangiocarcinoma.BMC Gastroenterol. 2025 Jul 7;25(1):501. doi: 10.1186/s12876-025-04104-6. BMC Gastroenterol. 2025. PMID: 40619373 Free PMC article. Clinical Trial.
-
Improving postoperative survival in cholangiocarcinoma: development of surgical strategies with a screening program in the epidemic region.World J Surg Oncol. 2024 Oct 31;22(1):287. doi: 10.1186/s12957-024-03573-5. World J Surg Oncol. 2024. PMID: 39478620 Free PMC article.
-
Liraglutide exhibits potential anti-tumor effects on the progression of intrahepatic cholangiocarcinoma, in vitro and in vivo.Sci Rep. 2024 Jun 14;14(1):13726. doi: 10.1038/s41598-024-64774-2. Sci Rep. 2024. PMID: 38877189 Free PMC article.
-
Opisthorchis viverrini-Current Understanding of the Neglected Hepatobiliary Parasite.Pathogens. 2023 Jun 2;12(6):795. doi: 10.3390/pathogens12060795. Pathogens. 2023. PMID: 37375485 Free PMC article. Review.
References
-
- Banales JM, Cardinale V, Carpino G, Marzioni M, Andersen JB, Invernizzi P, et al. . Expert consensus document: cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European network for the study of cholangiocarcinoma (ENS-CCA). Nat Rev Gastroenterol Hepatol. (2016) 13:261–80. 10.1038/nrgastro.2016.51 - DOI - PubMed
-
- Elkins DB, Haswell-Elkins MR, Mairiang E, Mairiang P, Sithithaworn P, Kaewkes S, et al. . A high frequency of hepatobiliary disease and suspected cholangiocarcinoma associated with heavy Opisthorchis viverrini infection in a small community in north-east Thailand. Trans R Soc Trop Med Hyg. (1990) 84:715–9. 10.1016/0035-9203(90)90159-c - DOI - PubMed
LinkOut - more resources
Full Text Sources

